- InterviewPenguin.com – Your best job interview coach since 2011

How quickly do you adapt to new technology? Interview questions answered
Technology is ever-present nowadays. Doesn’t matter whether we like it or not. We simply cannot avoid working with it, and it impacts us heavily in anything we do. What’s more, technology evolves quickly , almost at a scary pace. A ground-breaking application or hardware this year can become completely obsolete by the end of the next year. What can we do to keep up with the trends? We can either adapt , or pack our stuff and leave to live alone in the mountains in some hermitage. And while I fancy the second option at times, I am pretty sure you don’t. So what to say in the interviews, in order to impress the hiring managers with your attitude , and to eventually get the job?
Let’s have a look at 7 sample answers to the question. I tried to include both longer and shorter answers on my list (shorter may work better for job applications, since you typically have a limited space to express your thoughts on the application form), answers for people without previous working experience , and also some unconventional answers that may make the hiring managers think–should that be your goal in the interviews. Do not forget to check also text below the sample answers, for additional hints on how to make the most out of your answer to this interesting question.
7 sample answers to “How quickly do you adapt to new technology?” interview question
- Based on my experience from the last job in a smaller web hosting company, I can adapt quickly, and I actually enjoy the process . The company I worked for before tried to stay on the top of the pack, and hence they were always testing new things and applying new technologies on the servers. I can honestly say that I enjoyed the process, and didn’t mind learning something new every day. It actually made the job more interesting. Judging by this experience, I do not think I will have any problems adapting to the technologies you use in your business.
- To be honest I don’t know, since this is my first job application . Of course I’ve had a smartphone since I was 12 years old , and worked and played with plethora of applications. It helped me to build my computer intelligence, and I typically do not struggle to find my way around some new app or game. But I do not know what technologies you use here, and it can happen that I find them difficult to handle, at least from the start. Having said that, I want to ensure you that I do not give up easily . I am ready to devote my time to learn to work with any technology that I need to use in the job with you.
- It takes me time to adapt , since I do not belong to the generation that grew up with a tablet in the cradle. Having said that, I realize that computers are everywhere nowadays, and we cannot avoid working with them, unless we live in monastery perhaps, or in prison. Therefor I attend an evening course, and I also devote a lot of my free time to practice with various software, to make myself ready for my new job. I honestly believe that I can bring a lot onboard , a variety of strengths. Maybe I do not adapt easily to new technology, but I believe it shouldn’t be a showstopper in this interview.
- In my opinion, most of the new technology is over-rated . Just look at a typical workplace nowadays. People use Slack, Monday.com, and what not. We have online chats and meetings, and everyone tries to make the processes more effective. Yet do we really get more done as before? I do not think so. For me, email, MS Excel, and quick face to face meeting are still the best “tools” out there. No need for fancy apps that are supposed to help us save time , or collaborate better. Having said that, no doubt I can quickly learn to work with any new technology. I just feel that it isn’t the most important thing, and perhaps we put too much value on it.
- To be honest I do not like to adapt to the pervasiveness of technology in our daily life . Are we still human beings, or are we slowly changing to robots? Do we still use technology, or is the technology using us , controlling us, conditioning us, without us being aware of it happening? That’s a question most people prefer not asking themselves, for a good reason… Anyway, I try to limit my use of technology , and put emphasis on human contact, and soft skills . And I honestly believe each team needs such a person, and hope you will give me the chance to prove my words in the job.
- I’ve worked as an accountant in a middle-sized company before. During three years we changed three different software solutions , simply because the managers were looking for the most cost-effective way of running the business. Each of these accounting software packages had different interface and functionality, and I always had to learn to work with it from scratch. And I always did it, and adapted quickly to the changes. Do I think it was necessary, or beneficial for the company, to change the software often? I don’t. But it wasn’t my responsibility to make decisions . Hence I did what I could from my position, which means adapting to the software, and learning to work with it as quickly as I could.
- Based on my experience, it depends on my effort and attitude . Most people oppose changes and hate to learn to work with any new technology. And I had the same attitude in the past. However, I quickly realized that if I wanted to stay at the front of the pack, and to get the most out of my professional career, I had to change my attitude. And that’s exactly what I did. Now I can say that I adapt well and quickly to new technology , simply because I am open to such changes and give my best effort to learn to work with new technologies, instead of opposing them.
Practical example of a quick adaptation from the past is the best answer
Saying that you adapt quickly to changes, or new technologies, without elaborating on it, won’t take you far in the interviews . You should say something that demonstrates your ability to do so. For example, you can narrate a story from your last job. The company decided to get a new software, or implemented a new technology, and you had to adapt to it quickly. So you gave it your best effort , read tutorials, went to the course, and eventually learned to work with it, and applied it successfully in your work.

Unconventional answers can sometimes win you a job contract
As a rule of thumb, when they inquire about your ability to adapt to something in your new job (for example new technology), it means that you will face such situations at work . Perhaps they innovate a lot, or they simply use some unique custom-made software or technology each new employee in the department has to learn to work with, without having any previous experience. Hence you should try to convince them that you have such an ability, or at least want to give it your best effort.
Having said that, you can also opt for an unconventional answer. You can either say you do not like the pervasive role technology plays in our life (sample answer no. 5), and prefer to focus on “human touch” instead. Or you can claim that most new technology and applications are overrated, and employees who want to get the work done manage to get it done with the tools we’ve known for decades–email, Excel, etc (check sample answer no. 6 for a good example). Such answer will help you stand out, and may even lead to an interesting discussion with the hiring managers, which is always a good thing…
Ready to answer the question? I hope so! Do not forget to check also 7 sample answers to other tricky interview questions:
- Give an example of a time when you delivered on your commitment.
- Tell us more about your skills with MS Excel .
- How well do you adapt to new situations?
- Recent Posts
© InterviewPenguin.com
Privacy Policy

Sample essay about humans adapting to technology
Home » IELTS BAND 9 ESSAYS » Sample essay about humans adapting to technology
Should humans adapt to technology or should technology be adapted to us? Is technology making us intellectually weaker or more intelligent?
Whether the development of modern technology should be permitted to advance unhindered, or improved only with specific regard to human need, is a contentious issue. Since learning to use new technologies strengthens intellect, I believe that new devices should be developed without limits in order to challenge people.
The achievements of humanity over the last century have only been made possible by the development of modern technology. Driven by the need to discover, people have created countless innovations in fields such as electronics, medicine and engineering which have improved the lives of billions.
Additionally, many key discoveries throughout history were made while investigating something else entirely, such as with penicillin or the microwave oven. Establishing controls over what may or may not be investigated could therefore severely limit new discoveries.
This style of innovation also provides intellectual benefits for both the inventor and the consumer, since both must work hard in order to either create or use the new device. A constant flow of new discoveries maintains mental stimulation amongst those who choose to make use of them.
The computer, for example, has enabled humans to achieve remarkable things, but only after we adapted our behaviour and learned to use it fully. Also, those people who have maintained a good degree of computer literacy are now able to seek the best professional opportunities, which is further known to be intellectually beneficial.
In conclusion, I believe that technology should be allowed to develop freely and that humans should adapt their behaviour to emerging discoveries. This will keep us intellectually strong and ensure that the maximum good can come from scientific endeavour.
More help for IELTS exam
For a FREE ebook of our top 10 sample task 2 essays, click here!
For more help with your IELTS task 2 preparation, take a look at our tutorials to help prepare for the IELTS exam .
- IELTS writing task 2 questions
- Get ideas for your task 2
- Full guide to academic collocations for task 2
- How to start your agree/disagree essay
- Useful sentences for IELTS writing task 2
- IELTS writing task 2 tips
For band 9 IELTS writing samples, click here.

- IELTS Speaking Test Simulator (free)
- Free Essay Band Score Evaluation
- Sign up to claim your free IELTS materials
- Jump to Band 7 or it’s Free
- IELTS Writing Evaluation
- IELTS Band Score Calculator
- Book Your Online IELTS Test
- Sample Topic Answers
- Useful Sentences
- Sample Task 2 Questions 2022
- Introduction to Paraphrasing
- Model Band 9 Essay
- Five Band 9 Words
- Model Band 7 Essay
- Differences Band 9 vs Band 7 Essay
- Band 6.5 Essay
- Academic Collocations
- Topic Sentences
- Discuss Both Views
- Tutorial: To What Extent Essays
- Paraphrasing Introductions
- Essay Structures
- Essay Plans
- Describe a Pie Chart
- Using Percentages
- Map Vocabulary
- Describe Flow Charts
- Describe a Bar Chart
- How to get Band 9
- AT 1 Sample Questions 2022
- Describe a Graphic
- GT Task 1 Questions 2022
- IELTS Vocabulary
- Google Play / Podcasts
- Apple Podcast
- Android App
- Task 2 Sample Questions
- AT 1 Questions
Company addresses: HK Office: BW ENGLISH SERVICES HK Ltd, Unit 2512, 25/F, Langham Place Office Tower, 8 Argyle Street, Mongkok, Hong Kong UK Office: BW ENGLISH SERVICES, 120 High Road, East Finchley, N29ED, London, England, United Kingdom +44 20 3951 8271 ($1/min).

- Youth Program
- Wharton Online
- Business Journal Articles
- Entrepreneurs & Leaders
- Science & Technology
- Student Essays
Student Essay: Helping the Older Generation Embrace Technology

Share Article:
Google Classroom:
Jordan Mittler, a sophomore at The Ramaz Upper School in New York City and a participant in the Wharton Global Youth Summer Program, is the founder of Mittler Senior Technology, a company that helps senior citizens adapt to the world of technology. In this student essay, Jordan shares the story of how he started his business and why it has become so critical during this time of social isolation — especially in New York City, the epicenter of the coronavirus pandemic in the U.S.
In the next few months, Wharton Global Youth will be featuring a new essay every week, written by students around the world who are at home and eager to share their stories of entrepreneurship, leadership and experiences with business.
Five years ago, I gifted my grandparents, Janet and Mark Mittler, iPhones because it was painful for me to watch them still using flip phones! I have always been passionate about technology. I needed to get my grandparents, with whom I am very close, on board with the latest gadgets. It never even occurred to me that they would have no idea how to use an iPhone. They did not know how to perform many of the basic functions that come so easily to my generation, such as texting, Facetiming, photographing — and the list goes on.
And so, the idea for my business was born. I knew I needed to help this older generation, who missed the technology boom and was literally scared of trying to figure out our new connected world. As a result of this very real fear, they were often left alone and out of touch because they couldn’t communicate like everyone else.
Bonnie’s Got Mail
I decided to test my market concept at the local nursing home. I will never forget walking through those doors. I was only 11 at the time, and the director looked at me as if I had 10 heads. I went to the recreation floor and asked over a microphone: “Who would like free technology help?” I only had one taker. Her name was Bonnie Fisher, and I sat with her one-on-one for more than a year providing technology lessons. You should have seen Bonnie light up when she figured out how to connect with her sister and friends over email! I needed to figure out a way to reach a bigger audience.
I reached out to my synagogue, Congregation Kehilath Jeshrun, and asked if they would send a letter by mail promoting free technology help to all of their members over the age of 65. The synagogue was flooded with phone calls from interested seniors looking to enroll in tech class each Sunday. My temple, affiliated with my school, also let me use the school’s computer lab to hold my weekly classes. So many seniors showed interest that I had to maintain a waitlist. I got them into the classroom and taught them everything from texting to FaceTime and how to navigate the internet.
Fast forward to February 2020, and my classes were booming. I had even inspired some of my friends to join me in volunteering their time as teaching assistants. I had just added another class to fit in as many beginner and intermediate seniors as possible, and I felt like I was in a very good position to start scaling my business to reach even more learners.
We all know what happened next. Coronavirus swept through the world and our country, hitting the senior population the hardest and having a grim impact on New York City (reporting nearly 4,500 deaths through the beginning of April). During this time, I canceled my Sunday classes as my own schedule moved to at-home online learning.
I also realized, however, that senior citizens were suddenly even more cut off than ever. This new world of distancing was going to throw the older generation into more social isolation than they had ever experienced. One of my students, Roz Zuger, is 94 years old. I knew she would be disappointed without her weekly dose of tech class. So, I decided that I would attempt to continue my classes online via Zoom and walk all of my seniors through setting up the application and account. I started with Roz, spending endless phone calls with her to get her set up and comfortable with the online meeting platform. Roz had lots of trouble with the audio function on Zoom, and we slowly worked through this together.
After missing only one in-person class – and sending multiple texts and reminder calls — I had my whole class plus others online with me for our first virtual session. I updated my curriculum to be most helpful for seniors during this time when they were homebound and alone. For example, Rabbi Haskel Lookstein, the Rabbi Emeritus of my synagogue and Principal Emeritus of my school, needed help creating a group chat so he could communicate with all his children at one time. He was having particular trouble setting this up. I was able to show him virtually how to work through all the issues.
Facetiming and Ordering Groceries Online
The key to my teaching success with the older generation is showing, not just explaining. For seniors, talking in technology terms is less effective than presenting them with a visual of how to do something. They’re just not used to the language of technology. Roz, for example, was only able to launch Zoom after I Facetimed with her and sent her pictures via text of the next steps she needed to take. I helped Rabbi Lookstein by sharing visuals with him from my own computer screen.
In the past few weeks, we have been figuring this out as we go along – and it’s working. I started to record all of my Zoom sessions, so the seniors could replay any section of our class for review. After each online session, I send out a link to the recording, as well as a message with everything covered in class that day. My updated curriculum includes showing my students (which total some 80 seniors) how to order groceries online, how to order from Amazon, how to Facetime to stay connected, how to access online newspapers, and, of course, how to mute and unmute their Zoom audio.
It has been really rewarding for me to help so many people become tech-savvy during a time when technology has never been more fundamental to our daily lives. Social distancing has helped me bridge even further the gap between generations – and empower older people with the very valuable tool of connection.
Related Links
- Teen Vogue: Teens Are Helping Seniors Stay Connected
Conversation Starters
How did Jordan Mittler think like an entrepreneur in a time of crisis? Need help? Check out this Wharton Global Youth article for guidance.
Initially, Jordan only had one customer. Why was Bonnie so important to the growth of his idea and his business?
Have you used innovation to respond to needs during the coronavirus pandemic? Share your story in the Comment section of this article.
35 comments on “ Student Essay: Helping the Older Generation Embrace Technology ”
Wow! It’s incredible how technology can connect everyone. Many people often say that technology drifts us apart, but I’d like to disagree. In the current age, technology lets people from all walks of life to seamlessly connect. From Jordan’s example of how he helped local senior citizens be accustom to technology, it indeed shows how something as small as a smartphone can bridge generational divides.
Moreover, I’d like to add that I’ve seen a similar experience with my grandparents. My grandparents currently reside in India while I live in the US. This poses a problem as we cannot communicate readily. However, I found a solution to that vexing issue last summer. My family and I decided it was time for a change in the technology my grandparents were using, so we bought them iPhones. I helped them understand the ins and outs of how to use the technology which they were not familiar with. Because of this, they often facetime us from India and have even become like teenagers, as now they are glued to their phones.
Hi Vishnu, I really enjoyed reading your anecdote about your grandparents in India. I could relate to this issue since my grandparents live in Maryland, while I reside in New Jersey. Pre-isolation, my extended family and I would visit them almost bimonthly. This was crucial to their well-being, as they live alone in a rural area. During the quarantine, I helped introduce them to Zoom, which has been a useful online tool. Now that they are capable of using it, our entire family has weekly digital chats. In relation to this article, our examples of giving help to our grandparents exemplify the responsibility of younger generations to take initiative with technology. Jordan allowing the Rabbi Emeritus of his synagogue to communicate with all his children at once is an important example of lending knowledge and skills to older generations to maximize efficiency and happiness during these times of uncertainty.
I understand that technology helps connect people, especially during this time of endless quarantines. It is beneficial that the older generation is taking an interest in technology, breaking the stereotype that the elderly reject new ideas. After all, technology was and is made to make humans’ lives easier. However, while reading both your comments, Vishnu and Charlie, along with the article, I see that in all the cases of older people using technology, it is because the elderly generation have no other ways to stay connected. Now, this sparked a curious thought inside me—the elderly are using tech because especially during this time period, they really need it to prevent themselves from becoming isolated. But when it comes to young people, we just use tech because we are so addicted to it. We reach for a phone because it’s just what teens do. We text, FaceTime, and play multiplayer games with each other simultaneously. For the elderly, the chance to be able to connect with their loved ones is a big highlight in their life. They have not experienced such ease and luxury for much of their lives.
In contrast, teens have grown up around technology. We should try to bring back a culture that is less focused on technology usage to grow up appreciating the time we use technology, especially to connect with others. The younger generation is so desensitized by constant interaction through texting and voice/video calls that we often fail to appreciate it. I was surprised by the enthusiasm of the elderly when Jordan offered classes, but now I realize that it’s because they have realized its value and are taking efforts to gain the most out of it. For me, it took spending some time in quarantine to realize this. My friends and I are always complaining how we are so lonely, when we have actually been texting and calling daily before the COVID-19 outbreak. Teens need to shift a little bit away from the constant technology usage and take time to do other things that do not require technology—perhaps even teaching their elderly relatives about technology, as Jordan did.
I also have another major concern: older people are already at huge risk to scams and privacy issues, and presenting them with increased technology would give others more opportunities to take advantage of the elderly. I already admire Jordan very much for being able to accomplish the feat of teaching the elderly about technology, and I am also very impressed at how he runs his program so professionally and in such an organized way. But I also hope that Jordan, along with you, Vishnu and Charlie, for your grandparents, have presented the gift of technology as well as explained the dangers that come with technology. There are many scammers and hackers that target the elderly, as they are known to take weaker security measures without knowing the consequences. They are more susceptible to common false alerts on the internet and on phone calls. When we think of introducing technology to the elderly, thinking about their tech security and scam-awareness are not the first things that come to mind, so I think there should be further steps taken to make that a priority. Still, I understand that connecting with loved ones is a priority in this case, as it is a good thing that your grandparents have been able to establish a system of communication to maximize the time you all share. I hope there will be more cases similar to that of yours and Jordan’s students. That way, the world can truly be connected and everyone will FEEL connected!
Daniel It is interesting that you note that students now are doing school from home and despite being tech savvy, they miss the socialization of school and may have to find other ways of relating to their friends or spending their time. They can stimulate their minds thinking about how they can contribute to society, or better their reading and writing skills.
Charlie It is important for children and grandchildren to recognize that their senior relatives can benefit from learning technology, and a little patience in instructing them will make them so happy. On a personal note, my Rabbi has done so much for my family and has been there for all of our family’s life events, so it gave me personal pleasure to help teach him how to connect with his family in new ways during these challenging times.
I love your personal experience with your grandparents. Your thoughts remind me that helping the older generation learn the use of technology also help us connects our lives with theirs.
Vishnu This is wonderful to hear that you got your grandparents iPhones and they are now using FaceTime. It is interesting that you point out that technology sometimes causes people to drift apart, maybe because it is often something people do alone without communicating with others. There are so many elements of technology like face time or zoom that allow people to connect virtually.
Hey Vishnu,
It sounds like we both share Jordan’s experience with the elderly population. I definitely agree that technology has connected us all and bridged generations. While your grandparents are in India, mine are in Florida. I know it’s not quite as far away, but for them, it’s far enough. Similar to how you guys had to cater your lessons to what their generation was used to, I have had my share of challenging but also rewarding experiences. For Jordan, it was FaceTime and Zoom; for me, it was Gmail.
My grandpa called me one day because his friend had sent out a party invite as a list. Grandpa spent about forty minutes trying to find it. I told him to look carefully and like Santa, check his list twice. He didn’t think that was funny. I realized that his friend’s email probably went to his Spambox. I told him to look to the left to find Spambox and click on it. He replied “My Gmail must be different from yours; I don’t have a Spambox folder.” After a few minutes of trying to describe it to him, I FaceTimed him. I looked on his screen and realized that he needed to scroll down in order to find Spambox.
For me, I had always automatically scrolled down to find it without even realizing that I did this. To me, every action or click is like a knee-jerk reflex, but I realized that for grandpa, his reflexes needed a bit more time to kick in. Jordan is absolutely right in that the elderly need more hands-on and visual support. Remember, they grew up with things that required more physical interaction like holding a thick hardcovered book or applying their index finger on a rotary phone. Even my mom tells me she used to love watching each digit of the rotary phone make its way back!
Anyways, thank goodness for FaceTime. I showed grandpa how to scroll down to find his Spambox. And sure enough, the mysterious party invite miraculously appeared. I thought about teaching Grandpa how to move that conversation to his Inbox, but he was so elated that I decided to save this lesson for another day.
I found this article very relatable as I have as well tried to teach my grandparents how to use a mobile phone. At the end I was only able to teach my grandmother how to play candy crush and how to select who she wanted to call without needing to type the number every time. But nothing more. She kept refusing to learn the “new and unnecessary technologies”.
What he is doing very important, specially during the coronavirus epidemic. I have found the elderly are the ones who suffer the most isolation, as they are the ones that are less connected. It reminds me of a video what was viral in social media about a grandmother who sang happy birthday to herself, alone, in her house. It broke my heart. This is why seemingly-small ideas like these can really make an impact and change people’s lives for the better.
Hi Alejandra! I can totally relate to your experience. Due to the COVID-19 pandemic, I have been sympathizing for the elderly in nursing homes, who are not able to interact with families. Therefore, I started Facetime sessions with the elderly, either playing piano for them or chatting with them to help time pass by for them. However, I came across some obstacles, such as having difficulties getting on the video chat. She told me that although she enjoys having a companion to talk to, it is really hard for her to work with the technology, such as logging onto the computer. I was dejected for not being able to teach her about technology usage due to the quarantine lockdown.
Furthermore, I live on the opposite side of the globe from my grandmother. The only form of communicating and interacting is through technology. However, she also has hard time using it as well, and it really is painful to think that I am not able to spend most of the time actually talking rather than being lost on using the technology to communicate, especially when I want to spend as much time with her.
As of in the near future, I would like to create a nonprofit business, putting an emphasis on sharing our knowledge of technology to those who are not efficient with it.
Alejandra Seniors are often fixed in their ways and unwilling to change. They like what has been working for so many years. They have to be told that is ok to try things with their phone and not to be afraid to make a mistake. Your grandmother liked to make calls but she may like to learn how to text if she is encouraged to do so, and understand this is a popular way to communicating these days. If she tries it maybe she will like it. She may appreciate someone texting her an image or picture, something you can’t do over the phone.
This article really reflects the present situation of contemporary society.In just 20 years, from cover phones to smartphones, from 2G to 5G, from 8GB to 512GB, the change is so fast and dramatic that the elderly feel disjointed by the society. Take my family for instance. In the 5 years ago, my grandparents don’t know how to use the smartphones. But now, they can use the app like Wechat to communicate with others. When they go out and buy stuffs, they use the apple pay instead of paying the cash. This paves the convenient for them because the elderly will be easy to lost cash or coins on the way home. You know that they will be disappointed and complaint when they know they just lost several dollars. This problem can be solved now. The another advantage that I discovered is that seeing the doctor online. In the past, my grandfather had to get up early around 5.am and go to the hospital to make an appointment. In the morning, the temperature is very low and it is so tired for him to register. But now, they can make the appointment online through the app. This can largely save the time on the way to the hospital and queuing outside the gate. After finishing the doctor, The medicine will be mailed to the home, so that grandpa would not have to go to the hospital to get it again and again. This class sounds great since it helped a lot of “students” to learn the advanced technology. Nowadays, many young people are busy with their work and don’ have enough time to teach their parents to use the phones. This class just solves this embarrassment. Recently, my grandparents know a lot of knowledge about the prevention of COVID-19 and buying the food online without going to the market to reduce the risk of infection. The phones really make the life more convenient and these classes should be encouraged by the public. We should try our best to make the contribution to the society.
I agree with you, YuTao. The article really emphasizes the change that technology has brought onto the modern world and the transformational effect it can have on someone’s life. As technology evolves every day, so does mankind. And in this time and day, it’s up to the newer generation to educate the older generations about this change. Being part of the new generation myself, I’ve had to teach many family members about technology as well, such as setting up an app, purchasing something, or helping them understand how to communicate with their friends through the use of WeChat and similar apps. A couple of years ago, we went back to China to visit our family, and at the end of the trip, because the thought of saying goodbye and not speaking to them for a long time was so painful, we decided to get them new phones and teach them how to use them so we could communicate with the touch of a button whenever we missed each other. My cousin and I had to teach our uncles, aunts, and grandparents how to set up their new phones and WeChat because technology was still foreign to them at the time. And now, they use their phones just like anyone would in this day and time, despite the large age gap between us. At home, my mom constantly asks me questions about technology because she isn’t very technologically advanced, due to the fact that she immigrated here from China back when there was little technology available. However, now that she has one, she constantly asks me how to set things up, how to search things up, or how to manage her WeChat when she wants to call or FaceTime some of her friends. She’s also learned to use her phone to go places by using Google Maps. Using handheld maps and knowing the routes by heart is no longer needed with the advancement of technology. Because of the elderly’s age, getting places and doing things by themselves is not as easy as it was when they were younger. They aren’t able to support themselves, and their kids may be too busy with work and their own lives to be around them every hour of the day. With their newfound technology, they can call for assistance by simply pressing a button that will notify help, or call someone in case of an emergency. Technology could very well save someone’s life. Moreover, I feel like the class that Jordan has decided to teach could end up helping everyone, not just his students. His teaching the classes means that the elderly’s kids don’t need to teach them themselves, and instead can focus on working and supporting their family as a whole. They can rest assured knowing that their parents are safe and that they know what to do in case of an emergency. In addition, they could also learn to download some games for their own entertainment. It’s important to acknowledge Jordan for everything he’s done and to appreciate him for giving us this opportunity to experience something new that can help many. This example shows just how much technology has evolved over these years.
YuTao Thank you for your kind words. More people are no longer using money, so it would be helpful for seniors to use their phone to pay for things, maybe with credit card or Apple Pay. It is very helpful for seniors to be able to use electronics for medical purposes, like emailing with a doctor. I also teach in my class about a healthcare app where seniors can keep all of their medical information.
Experience is key in entrepreneurship. One of the few ways we have to better ourselves as entrepreneurs, and our businesses as life experiences, is going through an initial process of practice and learning, often a synonym for failure. Bonnie’s role in the case of this fantastic entrepreneurial story is exactly this one: giving Jordan a starting point, from which acknowledging the actions necessary to improve the quality of the business. As often stated throughout the article, connecting people has never had such an importance in the terrible crisis we are facing due to the Coronavirus outbreak. Older people are being left behind, not only technologically, but unfortunately socially too: missing tools, such as the previously discussed iPhones and laptops, and absent experience, make it much more difficult for grandmas and grandpas to go beyond the standard, old-fashioned phone call, in a world, in a time, where the closer we can get to having real-life meeting with our loved ones is joining a Zoom call. I personally find this a wonderful example of how we, as youngsters, can personally engage in making these terrible times lighter and less burdensome: each small action can make a difference, regardless of the size of our targeted audience, and our duty as world-citizen, I think, has never had such an important role in our everyday life.
Jacopo I’ve been very fortunate to have this entrepreneurial experience at this early age, and I hope to continue through my high school years so that I will be able to expand this program and scale it so it helps so many more people.
Similar to your experiences, I am also a sophomore and also volunteer to aid senior individuals in adapting to new technology! As a branch director in an organization called Teach Seniors Technology, I could not relate more on the initial difficulties in gaining customers. A few years ago, when I walked into my local community center to give my first lesson, there were only one or two students. In fact, there were many times during my first couple of months volunteering where no students had signed up for my weekly lessons! Though I wasn’t necessarily successful at first, I was also forced to adapt for these reasons. After reaching out to the community center staff, I was able to secure a classroom and promotion materials for my service which now serves several seniors each week.
Yet, I believe the “success” of my organization is determined by much more than the number of seniors who I teach. I often serve seniors from China, who have to bridge both the language barrier and the technological gap here in the United States. One of the ladies at my branch literally burst into joy when I taught her how to use Google Translate! In a world which is becoming increasingly interconnected and reliant on technology, I find that “success” of my volunteering branch rests on reintegrating these seniors into the technological area of society. I am overjoyed by the fact that there are other who share so much similarity with me. As more and more technological advancements are made, we must learn to bridge generational gaps so that our society as a whole can progress together with the technology that is being invented.
Jason It is wonderful to hear of another sophomore participating in a similar type of program.
Just like you, I help senior citizens but also adults from Central and South America with the technology and language barrier that thousands of people face in the United States. Technology is not common for lower classes in third world countries which makes it difficult for these adults and senior citizens to understand what seems like the basics of a smartphone for the majority of people in the US. It is such a joy when I see those which I help finally being able to communicate through Google Translate (An incredible tool I must say) and doing tasks like buying on Amazon, Instacart, or any online store. Observing this has made me come to the conclusion that we must come together as the new technology generation and help all of those individuals who have not gotten the opportunity to learn the incredible benefits the tech world brings; together we can close the digital divide across all ages, races, and socioeconomic statuses. We are the future and have yet to see great things created through technology.
Great response, Rossana! Do I see a team of digital-divide change makers forming here?
Technology helps join people, specially for the duration of this time of infinite quarantines. It is recommended that the older era is taking an hobby in technology, breaking the stereotype that the elderly reject new ideas. After all, technological know-how was once and is made to make humans’ lives easier. However, whilst analyzing each your comments, Vishnu and Charlie, alongside with the article, I see that in all the instances of older humans the use of technology, it is due to the fact the aged era have no different approaches to remain connected. Now, this sparked a curious thinking internal me—the aged are the use of tech due to the fact particularly at some stage in this time period, they genuinely want it to forestall themselves from turning into isolated. But when it comes to younger people, we simply use tech due to the fact we are so addicted to it. We attain for a smartphone due to the fact it’s simply what teenagers do. We text, FaceTime, and play multiplayer video games with every different simultaneously. For the elderly, the hazard to be in a position to join with their cherished ones is a massive spotlight in their life. They have no longer skilled such ease and luxurious for a great deal of their lives.
Despite efforts to teach the older generation about the newest developments in technology, it is saddening how much of the older generation is still very ignorant about it, especially since it is an era of technology.
One summer, I went to China to see my relatives, especially my grandmother. My grandmother lived in more rural parts of Sichuan, in Dazu. She didn’t need to use any technology; as long as she knew how to open the television and call using her corded home telephone, she could live happily growing plants in the back yard and raising chickens. She rarely went into the city to where my other relatives lived, they always visited her instead. However, to my delightful surprise, she proactively volunteered to wait for my arrival in Chongqing, one of the busiest cities in Sichuan.
When I arrived at my aunt’s apartment, where my grandma stayed, I asked jokingly why she decided to finally come to the city, she replied that it was because she hadn’t been here for so long. It was boring back home, and my grandma wanted to experience what life is like in the city for a while. She said that she would stay in the city until I left for America in a few weeks.
I was delighted and planned to take her to all sorts of fun places with great food that I had remembered from my last visit here. In Dazu, you could hardly find such boisterousness due to the lack of crowds. I was sure that she would enjoy it.
One morning, after I had officially settled in at my aunt’s house, my aunt and her husband told me that they were going to go somewhere for the rest of the day and needed me to take care of my grandmother. They said I could take my grandmother out to walk or do some other activities, but to be careful. I agreed with a smile.
My grandma was very happy this particular morning as well. She told me that she wanted to try exercising in the nearby park with some other old people; she wanted to make some friends here. I happily agreed. I walked her to the park and watched her dance and make merry with the folks there. After a few minutes, she could tell that I was a little restless and told me to play on my own and insisted that she could manage herself well. She said that she would go home when she wanted to and told me not to worry. I reluctantly agreed, told her the directions to the apartment building, and gave her the corresponding card. The apartment wasn’t that far, only one block away from the park. Then, I went off to a nearby stationary store to buy some souvenirs for my friends in America.
After some time, I picked the gifts that caught my fancy and went on the line to pay. The store was very popular and so the line was very long as well. After waiting for a quarter of an hour, I finally got out of the line and started my way home. In the distance, I saw a familiar figure. I panicked and hurriedly ran to the entrance of the apartment.
My grandma stood in the burning sun, her arms hung down at her sides, watching the pedestrians. Apparently, she had a squabble with the people from the park almost immediately after I left. She wasn’t in the mood to dance anymore, so she went home. However, the problem is that she didn’t know how to open the more technologically advanced apartment door. To me, the door system was very simple, you just had to swipe a card, but my grandmother never had to use this sort of system, she only ever needed a key. My grandma thought that you just had to press the card against the door or something. She also forgot how to call using the smartphone that was given to her. I also didn’t think it was necessary enough to teach my grandmother how to open the door since it seemed natural to me.
This story truly shows the importance of communication and the need to help the older generation with technology.
“When are you coming back?” These words were music to my 15-year-old ears. I had just helped fix the internet connectivity issue for Ms. Jacobson, one of the residents at Sequoias’, a senior residential facility, where I was volunteering to help seniors with their tech issues in the summer after my freshman year. Ms. Jacobson sent a very nice thank you note about the help she received from me to the Services Director at Sequoias who passed it on to me. The note, painstakingly written in spidery cursive must have taken Ms. Jacobson some time to write and is still cherished by me. The experience with helping seniors with their tech issues and entertaining them with piano recitals helped me get more attuned to the needs of my own grandparents. My two sets of grandparents are separated by a decade and come from similar backgrounds but have very different life experiences. One set of grandparents who live with us are older, technologically challenged, and can call on us anytime to help them operate the phone, the TV and other gadgets. They prefer to read the actual newspaper despite efforts to get them to read news online, and prefer talking on the phone instead of using Facetime. The younger set of grandparents who live in India have a large social circle, live on their own, and while still technologically challenged, have learned the basics of how to use a smartphone, browse the internet, and order online. Jordan’s article made me reflect on my experience working with seniors, both in my own family and outside and I realized that seniors face the same challenges that students of all ages face. First of all, every student learns in their own unique way, much like some of Jordan’s students – Roz and Rabbi Haskel. Some are visual learners, some need more time to read and absorb information on their own, etc. Secondly, each student has different capabilities and interests. Some like one set of my grandparents did not have much interest in learning how to use technology as they were happy with the old ways and could always ask us for help if they needed it. The other set of grandparents found ways to learn the basics that they needed to fulfill their needs as they were living on their own. There is also a social and cultural context to this. More and more seniors are now forced to live on their own, either in their homes or in senior facilities. Those that do not live with family face loneliness among other issues, and do need to know some basics such as texting, online searching and ordering, connecting with their medical provider online, etc. to stay safe, independent, and connected. The need to stay connected has been exacerbated by the COVID-19 pandemic. However, the issue with being connected is that not only are seniors more vulnerable to scams, they are also very gullible when it comes to fake news. I have had to constantly remind my grandparents who treat WhatsApp and Facebook as reliable news sources that everything they read there is not always true. The other issue is the plethora of apps, tools, and websites that can be overwhelming for seniors. I noticed this issue after working with a couple of seniors at Sequoias and created a home page for every senior I worked with, that contained shortcuts/icons for their most frequently used apps and websites for easy access. Perhaps in all of this, there is an opportunity to create senior-friendly apps and devices, but unfortunately, this is not a coveted demographic for tech companies and marketers. There is certainly a need to help seniors learn tech basics which can enrich and simplify their life. I applaud Jordan’s efforts to provide this valuable service to seniors in his community. However, the bigger question I ponder is that why are seniors put into this position in the first place where instead of enjoying time with their families, they are forced to learn new skills, especially when many have impacted cognitive skills which makes learning new things harder. Additionally, we are only talking about a subset of the senior population. There is a big population of seniors living in poverty who have more pressing issues such as survival to deal with. My own experience with my grandparents and with seniors I worked with is that every single one of them would have preferred to live with their families, surrounded by their children and grandchildren instead of connecting with them over facetime and group chats. In fact, the percentage of multigenerational families in the United States has continued to rise, primarily due to financial necessity. While one size does not fit all and every family has their own unique challenges, perhaps it’s time for us as a society to take a closer look at how best to support the needs of our senior population, given the increased life expectancy in the United States.
Hey, Jatin. I really enjoyed reading your thoughtful post and response. What I love most is that you bring up some broader issues that really add value to the “seniors and technology” conversation. I’ve always admired certain cultures — India for one — where families place more emphasis on caring for and living with their elders, the people without whom they would not even exist. The questions you raise about supporting our senior population are so important! We deliver them meals, help them connect, even give them a ride to the market, but we don’t go beyond to the point of human companionship and connection at a time when they need it most.
The age of smartphones has progressed so quickly that the fact the first iPhone originated just over ten years ago may come as a surprise to many. This development is only one example of a world industrializing at an unprecedented rate. Despite making communication and practically every other aspect of life easier, this revolution may not apply to all — the elderly, as you stated, are often not kept up to date to these new technologies. However, it must be noted that other adults may also not be kept up to date. I believe my parents are a prime example of this. They both immigrated to the United States in the 1980s and made a decent living running a restaurant. However, when it came time to digitalize, they struggled and required my older sister’s assistance to facilitate this new aspect of the business. Now that she’s off to college, it’s my turn to fulfill this position of filling out online documents and forms. This is a growing problem as it is a given that technology will only advance forward, regardless of whether there are those who are unable to utilize these new advantages. That is why I find programs like yours to be so fascinating and thoughtful. My mother has recently taken up taking computer classes, where she learns basic computer navigation skills. It is essential for the whole population to collectively adapt as a whole.
Alvin I appreciate the idea of showing seniors how to fill out forms online, and all of the elements involved in that process.
I certainly agree with Jordan that technology helps us stay connected. It is very important that we help the elderly members of the society on the use of technology. It is not easy to teach the older generation to use technology, as they are not quite familiar with it.
Moreover, I have also had a similar experience with my grandmother who just got a new iPhone and she did not know how to use it properly. Though she was able to make her daily phone calls and read her WhatsApp messages, she did not know how to access the Internet, do Face time and little other stuff. One day during the never-ending lockdown, I decided to teach my grandmother how to use her new phone. Since, she was having sleepless nights due to the change in her sleep cycle because of lockdown, I first taught her how to use YouTube so that she could put spiritual music on it and have good sleep. As days progressed I taught her how to access the daily news online, face timing, texting and many more things. This also gave me an opportunity to spend quality time with my grandmother, which I could not during my school days. My grandmother had a habit of doing all her office-work on paper so, later I started teaching her to use the laptop to check few mails and tally her accounts. This whole process not only helped her a great deal by making her work a lot easier, but also it helped me become more patient by answering the same quarries that she had again and again.
There have been vast advancements in technology over the years and it has helped us in many ways, such as online classes and courses, which are the most helpful things at the moment. By helping the elderly members of the society as to how technology can be used, bridges the generation gap and will help the society progress faster.
I’ve spent a lot of time helping relatives with technology and sometimes it can get very frustrating but I remember that they didn’t grow up with this like we did. So I am more patient and don’t get mad because I love my relatives. What Jordan is doing is really important, especially during this pandemic. The elderly are the most impacted in my opinion, because many of them lack technological experience. His Zoom meetings are a great idea though, keeping the elderly learning and up to date with technology so they can stay connected.
The younger generation is lucky. Since we were young, we have had access to electronic products. Elders often see their grandchildren typing like a speed of light with two thumbs on the keyboard or on the phone, while they themselves can only type letter by letter or word by word with their index fingers. Many elders have only had access to technologies in the past 15 to 20 years. We sometimes get annoyed when they want to learn how to use technology. But when thinking about our situations, aren’t we like them when we are trying to figure out how to solve a simple math question? We see the technologies are easy for us to learn and use, but the elders must take a long time to get used to using technologies.
The last time I saw my grandmother in person was five years ago, but we are able to FaceTime each other at least once a week. When I visited her in China five years ago, I saw her struggling to send a message on WeChat or even make a simple phone call. She would forget which group chat is which and would constantly send private messages in group chats with other family members in it. When I started teaching her how to use WeChat, I saw my grandma was listening to what I was saying very carefully. I taught her how to use WeChat for video calls, voice calls, and many other functions of the app. Later, she took her cellphone and just pressed on it casually trying to use the phone herself. This makes me think that the elders are still very curious to learn new things and look forward to more connections with others so as not to be disconnected from society.
Although she still struggles with using keyboards, my grandma has greatly increased her ability to use her phone. Now she is able to shop online and play simple games on her phone like mahjong and Candy Crush. She sends us many photos of places she has visited and writes that she wishes to take me on one of her trips. Communication is a bridge to build interpersonal relationships. From sharing feelings to expressing ideas, the world requires us to communicate with others. Not just through face-to-face communication, but also through technologies, we are able to share our feelings with others through a simple call or message. Especially during the COVID-19 pandemic, we find communication important with family members or friends or co-workers through technologies. We have stayed home for more than one and a half months, and we would need to communicate with our parents almost every day and stay with them 24/7 face-to-face. We might not know how to have a conversation with them before, but with this pandemic, we might have no choice but to speak with them. We have learned that communicating with them is not as hard as we thought, and moreover, it is enjoyable to hear stories from our parents or other elders in the family. The elders are aging every day and we are growing up every day. It is hard for us to frequently see each other in real life, so technology is how we would connect and communicate with them.
What a sensational experience, Jordan! I enjoyed reading your stories, and I was astonished at how your involvement with elders related to mine.
As another member of Generation Z, technology and the rapid advancement of modern devices have always piqued my interest. Due to my eagerness, I grew up as a tech nerd, earning the title of “tech guy” in the family. “Alvin, why is my wifi not connecting?” “Alvin, what’s wrong with our TV?” “Alvin, why is my Bluetooth not connecting?” At least five times a day, I would hear such questions from my parents and brothers. From simple wifi connection problems to complicated home appliance control systems, I had to be present if the issues involved technology.
My title became significant as COVID invaded our lives. Similar to your experience, my grandparents struggled the most as the majority of platforms and services turned online. Since my grandparents were in a higher-risk group for exposure to COVID, they had to be extremely cautious. They could not go outside to get food or to their workplace. Whether they liked it or not, they had to stay home and adapt to online platforms to order food and attend Zoom meetings. And, as the “tech guy” of the family, I was responsible for providing comfort for my grandparents. Starting from scratch, I had to water down difficult technological terminologies such as Airdrop, iCloud, and Bluetooth to help them rapidly adapt to new lifestyles. Such experiences were similar to teaching elementary schoolers about calculus, in which I realized how uncomfortable it was for my grandparents to utilize new technologies. For instance, Bluetooth features offer wireless connections within the comfort of one’s own vicinity, which is one of the reasons why younger generations utilize Bluetooth: it provides comfort. On the other hand, older generations have an arduous time figuring out how to connect devices using Bluetooth since they are unfamiliar with such features. It is true that consumers are attracted to more comfortable features, and businesses provide new technologies that could reduce time management for consumers. However, it creates a downside for older generations, making them take longer to do something. While convenience for the younger generations increases with the use of technology, the older generations are having difficulty adapting to rapid technological advancement.
By observing the hardships of older generations from my grandparents’ perspective, I thought there was a need for action. Although there are various ways to address such issues, I focused on a fundamental need for everyone: food.
Therefore, I gathered up my close friends, Robert and Kaiden, who shared similar visions regarding this issue, and we came up with an accessible software that will make it approachable for elders to order food from nearby food centers. Essentially, our solution focused on a sustainable, healthy, and accessible approach that is similar to your experience helping elders order groceries. We developed a food ordering app that sends prepackaged, nutritious meals to seniors who sign up for it. Our sign-up system is very simple since it could be pre-installed on phones, involves one click of a button, and has well-explained and accessible payment methods; for example, this service allows the program to automatically extract money from the elder’s source of payment which minimizes the complicated process of payment process every. Ultimately, elders can readily receive healthy and hearty meals at their doorstep. We also utilized the Zoom recording function to create tutorials to help elders navigate through our process. These methods of solution could sound ironic at first, but I believe the most effective solution for elders who are uncomfortable with technology is to expose them to an extent of unfamiliarity to reduce their discomfort.
Like most other start-ups, our application lacks feasibility, so initially, we must test it on a small group of elders and make adjustments. If our test proves to be successful, we will launch our application, which will familiarize elders with technology and aid them in accepting and embracing modern devices. Moreover, I would like to expand this business into providing food and holding online classes about ordering goods, entertainment, media, and safe technology use for elders. I would happily like to share words with you about this matter, and I want to resemble your helping and enthusiastic attitude towards social advancement.
Wow! This is a really beautiful essay. It inspires me to see a fellow teenager making such a positive impact in the world today.
Technology is one of the major generational gaps we have today, and it is very refreshing and encouraging to see someone trying to bridge that gap. I love your teaching strategy of showing instead of just telling. That is truly one of the best ways to explain. You made an astounding impact in a dreary and challenging time for many. As someone who teaches children in a local orphanage home, I can relate to the indescribable feeling of joy you get when your student finally understands.
I will also like to place emphasis on not just teaching seniors how to navigate the internet, but also on teaching them how to be safe while navigating the internet! Cyber crimes are increasing in a very tremendous way all over the world, as more people look for illegal means to usurp unknowing people. This is one of the major fears of seniors and the older generation concerning technology. I believe that teaching them how to best stay safe in the ‘dangerous’ global world provided by the internet would not just be beneficial to them, but it would also help in further bridging the generational gap.
Chidera, your comment is one that caught my attention. Your comment highlights a crucial aspect of our society today: the technology generation gap. Most importantly, the issue of cyber crimes. Indeed, with the rapid advancement of technology, it becomes increasingly challenging for elderly to keep up. Even some of us from younger generations struggle with mastering the intricacies of various tools and software, like navigating Google spreadsheets.
But you draw attention to the pressing issue of cybersecurity and cybercrime, which poses a significant threat to people of all ages, including the elderly. Even myself, who is clearly not an elderly person, receives tons and tons of spam messages and emails trying to trick me of my money. While these scams may not work on us, they can be extremely tempting for the elderly, who may be more vulnerable to such tactics.
For example, my friend’s grandma was a victim to these scams, falling victim to a company promising to save money for her granddaughter’s college tuition fee. This just highlights your point on the emphasis and awareness that should be put on cyber crimes. It demonstrates how easily elderly individuals can be targeted and deceived and the urgency of addressing the dangers they face while navigating the Internet.
Likewise, in the effort to bridge the technology generation gap, I believe that it is crucial to not only teach the elderly how to use technology but also raise awareness to the public about the prevalence of cybercrime and the importance of robust cybersecurity. By empowering people of all ages with knowledge and strategies to protect themselves online, we can help them become more confident and secure users of digital tools.
I truly believe that with stronger cybersecurity implementation and the awareness we can teach people about, the challenges of cyber crimes is one we can focus less on. Allowing us to focus more on bridging this generational gap, being able to facetime our loved ones, and even send them cool gadgets.
I think this is an amazing and much needed program! People tend to alienate the elderly from our evolving world, waving them off as they say, “You can’t teach an old dog new tricks.” This is incredibly isolating and unfair to them. A month ago, I helped organize a ceremony for my high school, and many senior citizens came to support their grandchildren. The program for the ceremony was online, and I watched many of them struggle to scan a QR code. It was clear they were embarrassed, and they deserve to spend the day celebrating their family rather than feeling ashamed.
It’s also important to recognize that technology can help them stay busy. Many of the elderly cannot drive or live very far from their families. My grandparents live across the world in India. They are retired, and travel is very hard for them. They don’t typically have much to do, and they can get bored and demoralized. However, my grandpa stays busy and keeps his mind sharp by playing sudoku on his iPad. My grandma loves to play candy crush or call her relatives. Teaching the elderly how to use technology can be more helpful than most realize.
Your example with your grandparents proves an important point about how technology is capable of managing and improving the quality of life of older adults through continuous mental stimulation and social contact.
More specifically, we should consider how within health care for the elderly, technology could play a role. It is now possible to bring medical assistance right into the living room of senior citizens through telemedicine, which is more particularly necessary for those who are immobile or far from healthcare facilities. In addition, wearable health devices track vital signs and warn caregivers or healthcare professionals of emergencies for increased safety and peace of mind.
By accepting and showing old people how to use this technology, we can contribute to maintaining independence and improving the quality of life of every population. It touches both their practical needs and makes them feel valued and included in our rapidly changing world. I strongly find that it is highly commendable on your part and Jordan’s regarding bridging this gap and thus inspiring others to identify and act on the potential benefits the technology offers to our senior population.
Jordan’s story is truly inspiring as his project helps us, as a society, to see the value of empowering our elders. Equipping and educating senior citizens on technology use does more than just allow them to connect with their families and friends but I believe it also improves their mental health via their perception of self-worth and identity. In the last decade, I’ve seen my grandparents withdraw more and more from society as the young grandchildren, who they often took to school and parks, did not need them anymore and their physical health began to decline. Too often the elderly suffer isolation from not only their families and friends but also the evolving world.The isolation in a physical and digital sense stops this flow of information, and thus education for them. My grandparents used to sit in silence with an expression of deep sadness and a personal confession of despairing uselessness. It seems that they are unable to feel that sense of accomplishment that we as students may experience when we receive that favorable mark on an exam.
However, when I successfully taught my grandparents to use their new phones they lit up with the excitement of being able to do things for themselves again. I saw them smile while reading the latest news online and laugh with old friends over the phone, leaving the fog of melancholy behind. Thus, I strongly believe in the potential to further the use of technology and educating senior citizens to help them discover new hobbies (ie. digital art, writing blogs, virtual dance classes) new selves, and their own power that makes them so unique, human, and worthy of all.
Leave a Reply Cancel reply
Your email address will not be published. Required fields are marked *
Save my name, email, and website in this browser for the next time I comment.
Related Articles
The allure of artificial intelligence, moniola odunsi fights for racial justice.
New Technology’s Influence on the Future Essay
Introduction, main innovations, innovation problems, blockchain technology, autonomous systems, electric cars.
Doing business is a precarious business. First, it is necessary to decide on the type of business, all the technical characteristics, and other equally important details. Recently the market has changed a lot, thanks to a large number of innovations and technologies that are introduced not gradually but almost immediately. Each of them allows companies to bypass their competitors and attract many new customers with unique features of both the product itself and methods of production. This paper will focus on the analysis of this problem and what innovations in the current world are important and able to change the market industry in the future.
One of the most trending and controversial innovations is using artificial intelligence in creative tasks. In the last few years, the augmented reality and machine learning industries have reached great heights, affecting artists, writers, and designers, who have already started to lose their jobs. Virtual reality is one of the most important innovations which can replace many aspects of life. The most important are social interaction and the learning process. Using a virtual world, a person can get much knowledge without reference to the teacher and communicate with other people through chats and video calls and by having close contact with their avatars (Granja & Moreira, 2019). It is also worth noting another element that can change the usual perception of the world, namely alternative fuel sources. Thanks to the use of electric batteries, the oil industry was almost destroyed, and a large number of people working in the industry lost their jobs.
All these technologies exist, but in limited quantities, as the main problem with their implementation is the high cost. Only some people are ready to spend a large sum of money to buy all the necessary equipment. In addition, an important role is also played by the development degree of these projects, as most of them are at an early stage of development and implementation (Orbach, 2020). All these technologies require more time for refinement and development of functionality, which may affect their future availability and lower the threshold of entering the world of new technologies.
New technologies have the potential to significantly influence the future and shape the way we live and work. Some examples of emerging technologies that are likely to have a significant impact include:
Artificial Intelligence (AI) is the computer systems simulation of human intelligence processes. These processes include learning, reasoning, and self-correction. AI has the ability to analyze and understand complex data, make predictions, and adapt to new situations. AI technology is being applied in many industries, from healthcare to finance to transportation, to improve efficiency and decision-making (Costello, 2018). Examples of AI applications include virtual personal assistants, self-driving cars, and medical diagnosis systems. Despite the many potential benefits of these technologies, they also raise many challenges and concerns. Some of the leading innovation problems include:
Privacy and security risks: Many new technologies, especially those that rely on data collection and sharing, raise serious privacy and security concerns. Ensuring that personal data is protected and that systems are secure is crucial to gaining widespread trust and adopting these technologies (Orbach, 2020). In addition to these risks, there are also aspects of economic and social impact. New technologies have the potential to create winners and losers, as some jobs and industries are disrupted while others are made. Addressing these technologies’ economic and social impact is essential for ensuring that the benefits are widely shared.
Blockchain technology is a digital ledger that records transactions on a decentralized network. Each block in the chain contains a record of multiple transactions, and every participant in the network has access to the entire ledger. The decentralized nature of the network means that there is no single point of failure, and transactions are recorded immutably. This makes blockchain technology highly secure and resistant to tampering. It has been used to create digital currencies such as Bitcoin but is applied in other industries such as supply chain management, voting systems, and real estate. Virtual and augmented reality are also gaining momentum in recent years. Virtual Reality (VR) provides a computer-generated simulation of a three-dimensional environment that can be interacted with using specialized equipment, such as head-mounted displays (Costello, 2018). On the other hand, Augmented Reality (AR) involves superimposing computer-generated information on the user’s view of the real world. VR and AR can be applied in various industries, from gaming to education, real estate, healthcare, and many more. The target market for this technology can be the sales area, where the option of buying goods for cryptocurrency is already being implemented today.
With the advancement of technology comes the question of sustainability and ethical implications. With increasing energy consumption, electronic waste, and data center energy consumption, we must consider the environmental impact of the technology we are developing (Costello, 2018). Furthermore, integrating technology into our lives has led to the ethical question of how we use this technology, such as issues like surveillance, privacy, and the balance between accessibility and security.
Another important technology that is shaping the future is the technology of autonomous systems. Autonomous systems are capable of sensing, adapting, and operating independently from human intervention. Autonomous systems are used in many areas, such as automotive, military, and emergency technology (Matthews et al., 2021). The most common examples of autonomous systems are self-driving cars and drones, but the technology can also be applied to other systems, such as robots and spacecraft. The advantages of autonomous systems include improved safety, increased efficiency, and the ability to operate in environments that are not safe for humans. However, this technology also raises important questions about liability and regulation, especially in the case of accidents involving autonomous systems. As mentioned above, the target market for this innovation is various services that may need to carry out dangerous operations remotely.
The Internet of Things (IoT) refers to the interconnectedness of physical devices and objects through the internet. These devices are equipped with sensors, software, and network connectivity, allowing them to collect and share data. This data can be used to improve efficiency, automate processes, and make better decisions. Examples of IoT devices include smart home devices, industrial control systems, and wearables. The Internet of Things is used today in medicine, programming, artificial intelligence, and communication (Nord et al., 2019). By connecting devices to the internet, IoT collects and analyzes data on a massive scale, enabling new insights and improvements in various domains. Biotechnology is also important, particularly in the field of synthetic biology. This technology aims to design and build new biological parts, devices, and systems that do not exist in the natural world. Synthetic biology can be applied to developing new drugs, vaccines, biofuels, and even food production. Technology has the potential to revolutionize many industries and improve human lives, but it also raises essential ethical considerations about the creation of life forms and their impact on the environment.
Speaking about each of these aspects in more detail, there are several unique features to note. The development of artificial intelligence can bring changes in the labor market of professions. People who have spent years learning their craft in the first place are left without proper recognition and the opportunity to develop their creativity further (Orbach, 2020). In the creative fields, for example, the market will shift toward quickly generated content, reducing the number of in-demand live professionals. This makes the situation much more manageable. However, the project is still underdeveloped at this stage because neural networks cannot act on the same level as human perception (Costello, 2018). The main benefit to clients is that the task they need will be completed as quickly as possible, lowering the price of the work, and removing the problem of finding a professional. The main requirement for the technology is a quality and fast solution to the necessary tasks.
As for the situation with the development of the virtual world, there are many uncertainties and assumptions. It opens the door to a world where nothing is accurate, and there is the possibility of making mistakes. Virtual reality is changing the education and entertainment market. It made it possible to move a large portion of the population to distance learning and work during the pandemic. This technology will change the entertainment market, which will hit the amusement parks. On the other hand, customers will be able to close part of their need for travel and joy with one purchase because, thanks to virtual reality, a person can get into any world without leaving home (Costello, 2018). Very often, examples of virtual reality can be seen in the classes of doctors and nurses, who are not yet ready for actual patients but need a full-fledged practice. The main requirements are to lower the price of the technology to make it more accessible, expand the options and customize it for different activities. The target market for electric cars is people who are interested in new technologies and care about nature.
The only technology that will not completely replace human labor, but will change lives for the better, is electric cars. The market for electric cars is getting higher every year, significantly affected by the demands of EU countries for cars to reduce emissions to the outside world (Granja & Moreira, 2019). This technology will hurt the market of cars with internal combustion engines and the market of gasoline. Customers will get a car that meets the requirement of many states and will save on gasoline and car repairs. The general requirement for this technology is adopting the state law on protecting the environment, advertising electric cars, and reducing their prices.
Advances in technology will change the world as we know it in many ways. People continue to look for ways to simplify life, even though there are consequences. Throughout history, humanity has adapted to change, and it is an inherent part of history that continues to repeat itself repeatedly, leading to new unpredictable outcomes. Therefore, we can conclude that despite progress, these technologies are still far from perfect and have the potential to change the marketplace. However, people in certain professions already need to be prepared now that a new era is coming in which technology is becoming a higher priority.
Costello, A. M. (2018). Credit market disruptions and liquidity spillover effects in the supply chain . SSRN Electronic Journal . Web.
Granja, J., & Moreira, S. (2019). Product innovation and credit market disruptions . SSRN Electronic Journal . Web.
Matthews, G., Hancock, P. A., Lin, J., Panganiban, A. R., Reinerman-Jones, L. E., Szalma, J. L., & Wohleber, R. W. (2021). Evolution and revolution: Personality research for the coming world of robots, artificial intelligence, and autonomous systems . Personality and individual differences , 169 , 109969. Web.
Nord, J. H., Koohang, A., & Paliszkiewicz, J. (2019). The Internet of Things: Review and theoretical framework . Expert Systems with Applications , 133 , 97-108. Web.
Orbach, B. (2020). Antitrust in the shadow of market disruptions . SSRN Electronic Journal . Web.
- Microwave Radiation's Impact on Different Microorganisms
- The Impact of Smartphones on Mental and Emotional Well-Being
- Blockchain and Bitcoin Technology
- Blockchain and Internet-of-Things in Agriculture
- Monitoring Health Statistics Using Blockchain
- Modern Technologies: Impact on Employment
- The Impact of Spotify on the Consumption Industry
- The Impact of Photoshop on Graphic Design
- PayPal and Human-Computer Interaction
- Industrial Revolution in Agriculture
- Chicago (A-D)
- Chicago (N-B)
IvyPanda. (2024, January 10). New Technology's Influence on the Future. https://ivypanda.com/essays/new-technologys-influence-on-the-future/
"New Technology's Influence on the Future." IvyPanda , 10 Jan. 2024, ivypanda.com/essays/new-technologys-influence-on-the-future/.
IvyPanda . (2024) 'New Technology's Influence on the Future'. 10 January.
IvyPanda . 2024. "New Technology's Influence on the Future." January 10, 2024. https://ivypanda.com/essays/new-technologys-influence-on-the-future/.
1. IvyPanda . "New Technology's Influence on the Future." January 10, 2024. https://ivypanda.com/essays/new-technologys-influence-on-the-future/.
Bibliography
IvyPanda . "New Technology's Influence on the Future." January 10, 2024. https://ivypanda.com/essays/new-technologys-influence-on-the-future/.
- To find inspiration for your paper and overcome writer’s block
- As a source of information (ensure proper referencing)
- As a template for you assignment
IvyPanda uses cookies and similar technologies to enhance your experience, enabling functionalities such as:
- Basic site functions
- Ensuring secure, safe transactions
- Secure account login
- Remembering account, browser, and regional preferences
- Remembering privacy and security settings
- Analyzing site traffic and usage
- Personalized search, content, and recommendations
- Displaying relevant, targeted ads on and off IvyPanda
Please refer to IvyPanda's Cookies Policy and Privacy Policy for detailed information.
Certain technologies we use are essential for critical functions such as security and site integrity, account authentication, security and privacy preferences, internal site usage and maintenance data, and ensuring the site operates correctly for browsing and transactions.
Cookies and similar technologies are used to enhance your experience by:
- Remembering general and regional preferences
- Personalizing content, search, recommendations, and offers
Some functions, such as personalized recommendations, account preferences, or localization, may not work correctly without these technologies. For more details, please refer to IvyPanda's Cookies Policy .
To enable personalized advertising (such as interest-based ads), we may share your data with our marketing and advertising partners using cookies and other technologies. These partners may have their own information collected about you. Turning off the personalized advertising setting won't stop you from seeing IvyPanda ads, but it may make the ads you see less relevant or more repetitive.
Personalized advertising may be considered a "sale" or "sharing" of the information under California and other state privacy laws, and you may have the right to opt out. Turning off personalized advertising allows you to exercise your right to opt out. Learn more in IvyPanda's Cookies Policy and Privacy Policy .
The future of the workplace: Embracing change and fostering connectivity

Partners with organizations to provide research-backed expertise on leadership, talent management, learning and development, and future of work topics.

Partners with clients across a variety of sectors on topics regarding analytics-led organizational transformations, with expertise in future of work and talent management to drive lasting impact
June 21, 2021 COVID-19 has changed the workplace as we have known it. While the physical space still exists, the overall idea of what a workplace is and what it is for needs to be reimagined. Organizations must deliberately address the changes wrought by the pandemic and the rapid pace of technological investment to enable remote and flexible work. In particular, organizations must take three key actions.
Embrace the hybrid model. The post-pandemic outcome is clear: a hybrid work model in which part of the workforce works outside of the traditional office for part of the time. The more important question: Which portion of the workforce needs to be present in the office, and when, and for what reason?
Employees are craving clarity about what is coming next in terms of work arrangements. It falls on organizational leaders to chart the path for managers and employees. Transparent and frequent communication, with managers playing a key role, can help ensure that the organization moves in unison.
In a recent survey, we found that organizations that articulated more specific policies and approaches for the future workplace have seen employee well-being and productivity rise . More specifically, organizations that have clearly communicated post-COVID-19 work arrangements have seen a two-fold increase to employee-reported feelings of support, a three-fold increase to feelings of inclusion, and an almost five-fold increase to reported feelings of individual productivity. Attempting to force a one-size-fits all solution can have detrimental effects on the workforce, particularly on women, people of lower socio-economic status, and people in less advanced economies.
Reimagine the physical space. The office of the future requires organizations to consider the altered footprint and layout that will emerge from a hybrid work model. Since in-person work will look substantially different, organizations need to make sure that their physical space is in tune with the objectives of the people within it. Pre-pandemic cubicle setups may be a thing of the past, making way for areas of collaboration, innovation, and community-building.
Real-estate footprints of many organizations will also change significantly. Already, we have seen many companies move to new geographies to tap new talent pools. For example, a large technology company recently announced some roles could remain remote indefinitely, allowing them to leverage talent from around the country. Others, such as a large financial company that is planning on having 60 desks per 100 employees, are rethinking their real-estate spend as they move to hybrid working models.
Manage fundamental human needs. The overnight shift to remote work has been one of the most notable real-time social experiments of recent times. It has shown that remote work does not necessarily come at the cost of productivity. In fact, many companies have reported increased productivity. A McKinsey analysis found that more than 20 percent of the workforce could work remotely three to five days a week as effectively as from an office.
However, remote employees complain that it is difficult to feel connected to colleagues and manage work-life boundaries . Some companies are adamant about the value of remote work while also being concerned about its effect on employee well-being. One online retailer, for example, is addressing these concerns and is acquiring over 900,000 square feet of new office space across six U.S. cities. The gradual return of in-person work alongside the newfound importance of virtual workspaces means organizations need to figure out ways to increase connectivity and a sense of belonging, regardless of where employees are.
The relationship between employees and the workplace has changed in ways that require organizations to invest seriously in helping people navigate through their vision for the hybrid workplace and any changes to the physical workspace. Doing so can help employees balance productivity, well-being, and a sense of connection in the evolving future of work.
This blog post is part of a series on the future of work post-pandemic, exploring three symbiotic elements of work , the workforce , and the workplace .
Learn more about our People & Organizational Performance Practice
Why Do Your Employees Resist New Tech?
by Frank-Jürgen Richter and Gunjan Sinha

Summary .
Due to several barriers, tech adoption at an organizational level is often slow or even nonexistent. Why is true tech adoption so difficult to achieve? Based on the authors’ experience working on these issues, they see five key actions business leaders can take to create a culture that will help drive better, more effective tech adoption: 1) incentivize technology use, 2) invest in infrastructure, 3) make reskilling and learning part of the plan, 4) don’t make it piecemeal, 5) and understand how governments and policy are involved.
While the use and application of technology has become near ubiquitous around the world, the actual adoption of new and emerging technologies across most organizations continues to be less than optimal. Due to several barriers, tech adoption at an organizational level is often slow or even nonexistent. This keeps old legacy systems alive and hinders an organization from achieving its full potential efficiently. This lag in adoption has long been a concern for companies but now, amid a pandemic, it’s a crisis.
Partner Center
Advertisement
Digital technology adaptation and initiatives: a systematic review of teaching and learning during COVID-19
- Open access
- Published: 26 April 2023
Cite this article
You have full access to this open access article

- Xue Zhou ORCID: orcid.org/0000-0002-7242-0958 1 ,
- Christopher James MacBride Smith ORCID: orcid.org/0000-0001-5708-6341 2 &
- Hosam Al-Samarraie ORCID: orcid.org/0000-0002-9861-8989 3
6010 Accesses
7 Citations
1 Altmetric
Explore all metrics
COVID-19 dramatically influenced students’ and staff’s learning and teaching experiences and approaches to learning. While many papers examined individual experiences in the context of higher education, synthesising these papers to determine enabling and hindering influences of digital adaptation was needed to guide the next phase of online learning reforms. This study explored the main dimensions of digital technology adaptation in higher education during the COVID-19 pandemic. The consequences for student and staff experiences and what aspects should be sustained and developed were discussed in this review. A total of 90 articles (published between 1st January 2020 and 30th June 2021) were identified and analysed based on the preferred reporting items for systematic reviews and meta-analyses framework. Four dimensions (with associated sub-factors) were found to influence student and staff experiences: techno-economic; personal and psychological; teaching, learning and assessment; and social. The findings highlighted that an integrated approach, across institutional, technical platforms, and individuals would be required to sustain digital learning initiatives during the crisis time.
Similar content being viewed by others

Digitalisation Transformation in High Schools: Analysis of the COVID-19 Pandemic’s Accelerating Impact

Embracing Digital Teaching and Learning: Innovation Upon COVID-19 in Higher Education

Reimagining Education Systems: How Research on Digital Learning Can Inform Pedagogical Practice
Explore related subjects.
- Digital Education and Educational Technology
Avoid common mistakes on your manuscript.
Introduction
COVID-19 has had a significant impact, whether this has been dealing with bereavement, ill health, or coping with government public health controls and levels of lockdown. While many areas of life were suspended, governments around the world have been in a constant search for ways to keep education going (Müller et al., 2021 ). Universities, their staff and students were forced initially into ‘Emergency Remote Learning’ and then continued with online learning or adjusted to a hybrid approach of on- and off-campus delivery. Consequently, there has been a significant adoption of and adaptation of various digital solutions to support online teaching and learning effectively; adoption and adaptation were recognised as two sequential stages in deployment (Venkatesh & Bala, 2008 ). Technology adoption models, such as Technology adoption model 3(TAM3) (Venkatesh & Bala, 2008 ) and unified theory of acceptance of use of technology (UTAUT) (Venkatesh et al., 2016 ) have validated general factors that influence the use of technology, including psychological, social, facilitating conditions, and system. Moreover, Venkatesh et al. ( 2016 ) developed a multi-level framework for UTAUT, where higher level attributes, such as (physical) environmental, geographical location and organisational, influenced technology acceptance and usage. Bala and Venkatesh ( 2016 )’s adaptation model indicated influencing factors such as experience, training effectiveness, psychological engagement, management support, and reaction to change based on threat or opportunity determination; responses were mediated by either emotional or environment-influencing strategies. In a similar vein, personal awareness, ability, organisational management, and collaboration among the colleagues also been found to impact on the academic staff technology adoption by using concerns-based adoption model (CBAM) (Petherbridge, 2007 ). In recognition that published studies of staff and student experiences detailed adoption of and adaptation of technology due to COVID-19, but did not consistently indicate their use of technology pre-COVID-19, then the term adaptation (as later stage) has been utilised in this research to encompass both adoption and adaptation. Consequently, between the models of technology adoption and acceptance, influencing factors were generalised initially for this research as technology/systems, social, and psychological, including the need to consider higher-order attributes (beyond the individual); these general factors and attributes were used in coding (see methodology section).
Most studies on digital technology adaptations during COVID-19 provided programme, course and institutional level cases that presented a varied situation of acceptance, adaptation, and desire to continue with a blended approach or return to face-to-face learning (Ghazi-Saidi et al., 2020 ; Hattar et al., 2021 ; Sebbani et al., 2021 ). Holistically, these cases were contradictory around experiences of staff and students and do not provide a synthesis of available international empirical cases to examine commonalities across domains (institutions, disciplines, and technologies). The few systematic literature reviews (based on articles published around adaptation in Higher Education in first few months of COVID-19) highlighted that pragmatic approaches by academic and technical teams were taken, which resulted in mixed opinions of quality, efficacy, and efficiency. Such rapid adaptation was met with resistance from some staff and students, in part due to unproductive study spaces and mental wellbeing issues. Additionally, technology challenges created issues in quality of, and access to teaching and learning resources, including in laboratory and practice-based activities (Deng et al., 2021 ; Maddumapatabandi & Gamage, 2020 ; Mseleku, 2020 ). Positively, the changes in response to COVID-19 have driven innovation and exposed staff and students to new forms of teaching, learning and assessment that have potential to improve experience, yet further research was advocated (Talib et al., 2021 ). This systematic review provided an updated, integrated perspective around institutional, technology and individual level adaptations and experiences that would inform future practice. In the context of technology adaptation during COVID-19 (an enforced step-change in practice), then it was important to examine what specific dimensions influenced experiences (coping) across a range of disciplines. Based on these observations, this study aimed at answering two research questions: (1) What are the main dimensions affecting students’ and staff’s learning and teaching experiences during COVID-19? and (2) What are the initiatives required to enhance digital technology adaptation in the post-COVID-19 period? The aim of this systematic review was to explore digital technology adaptation in higher education and its related impact on the experiences of staff and students during the COVID-19 pandemic, and how to use the experiences to form a supporting HE environment to improve the digital technology adaption.
Methodology
The Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines by Liberati et al. ( 2009 ) was applied to guide the review and answer the research questions outlined earlier.
Literature search
This review consisted of previous empirical research on students’ and staffs’ learning and teaching experiences during the COVID-19 pandemic. The search of previous studies was based on predefined database sources: ERIC, Education Database (Proquest), and SCOPUS. Most of the titles identified outside the primary search were not detected by the Web of Science database because they did not contain the set of search terms that we used in this study. Thus, this review used the SCOPUS database because it contains both the ISI and Scopus indexed rank papers (Oakleaf, 2009 ). Google Scholar was also used because some of the publications were not published in scientific journals and their impact cannot be tracked by scientific citation (Ficko et al., 2019 ). Empirical studies (e.g., qualitative, quantitative, and mixed methods) were included that were carried out across different, global university settings. All relevant empirical studies published in peer-reviewed journals, and conference proceedings (for which full-text was available to researchers) were included in this review.
In addition, only English-written articles that were published between January 1st 2020 and June 30th 2021 were retrieved and processed in this review. This start date was chosen because it demarcates the spread of COVID-19 across the globe (in accordance with the declaration of World Health Organization). Search records were retrieved on 12th July 2021. The following keywords were used in the search: (“Covid” OR “Covid-19” OR “pandemic” OR “post Covid”) AND ("digital learning" OR “online learning” OR “blended learning”) AND (“higher education” OR “university” OR “tertiary education”) AND ("interview" OR "questionnaire" OR "survey" OR "focus group" OR "case study") AND ("students" OR "learners" OR "tutor" OR "Faculty" OR "lecturer" OR "teacher") AND "experience". Boolean operators and quotation marks were utilized in the search to identify potential intersection between the keywords and facilitate the retrieval process of variations found in the lexicon related to students’ and staffs’ learning and teaching experiences.
Screening and coding procedures
The initial search result of the literature was 4300 empirical studies (including additional records from cited works). An initial screening of titles and abstracts of these studies was conducted to determine the relevance and value of each study to the current review. Articles were included based on certain inclusion criteria: publication (the article was available in a peer-reviewed, scholarly journal or conference proceeding); language (the article was written in English); content (the article investigated the experiences of students or staff during COVID-19); and context (the sample in the retrieved articles was limited to university students and staff). After applying these criteria on the retrieved articles and excluding of duplicates, 571 studies remained. Other systematic, scoping, and conceptual papers (e.g., ideas and opinions) related to university students’ learning and non-peer-reviewed research were also excluded; there were limited scoping and systematic reviews, and these were used to inform research questions in this study. A total of 481 studies were excluded during the screening of the full article because some studies did not clearly report the impact of COVID-19 on students’ learning experience, or methodologically had small sample sizes (< 50 for quantitative studies to ensure sufficiently representative of capturing representative experiences (Kelley et al., 2003 )) or too few for trustworthiness in qualitative studies (Boddy, 2016 ; Korstjens & Moser, 2018 ). As such, 90 articles remained in the final phase (see Fig. 1 ).
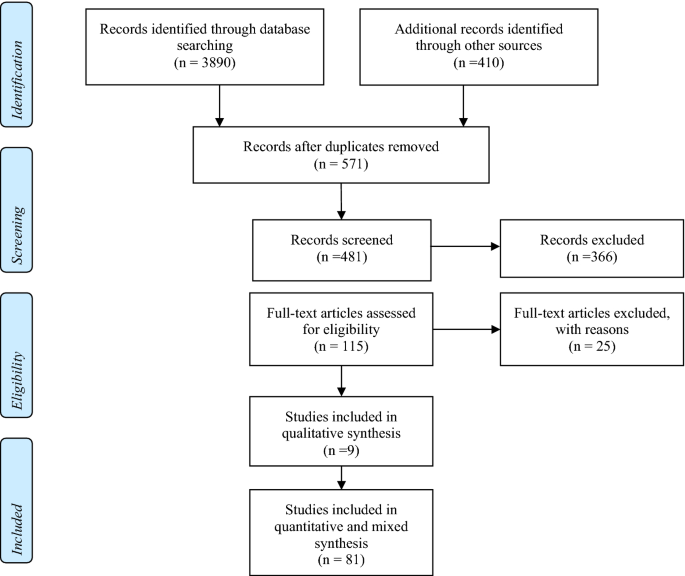
Article searching and selection process based on the PRISMA statement
A literature matrix was created and used to help in the review process of the identified articles. The matrix consisted of multiple columns (study features) and rows (studies). Over and above bibliographic information (citation, article title and journal) in each row, eight study feature groupings were coded for each study in this review: (1) country of study, (2) discipline area(s), (3) methodological characteristics (study design, type, and sample size), (4) technology characteristics, (5) factors, (6) benefits, (7) challenges and (8) recommendations and implications. The first two features were important to determine regional and discipline coverage of included studies. The third grouping ensured the article met the inclusion criteria, whilst the fourth captured details of technology types (where specified). The features in the fifth grouping along with the sixth and seventh groupings recorded how digital innovations influenced learning and teaching (so related to the first research question), with initiatives relative to the second research question captured in the eighth group.
The identified articles were read carefully and evaluated by the first and second authors. These authors independently inductively coded the articles using the general factors identified above—technology/systems, social and psychological—for initial framing. A meeting between first and second authors was set up to compare codes and an iterative process of discussion agreed the naming and content of the codes (sub-factors) relating to students’ and staff’s learning and teaching experiences. Through this coding process additional dimensions (themes) and sub-factors were agreed. As a result, four main dimensions emerged: techno-economic; personal and psychological; teaching, learning and assessment; and social. Intercoder reliability was used to indicate the intercoder agreement for article classification across the authors. The obtained Krippendorff’s alpha for the four themes were above the recommended level of α = 0.8. These dimensions were interpretable in accordance with the technology used by students and staff across different disciplines. These dimensions were used to code students’ and staff’s learning and teaching experiences during COVID-19, as an item-focused coding approach was effective in outlining relevant themes across university disciplines.
Quality check
Three reviewers evaluated independently the final list of articles. The following criteria were used to assess the quality of each article:
Relevance of the study objectives in addressing the research questions.
Appropriateness of the study design for the stated purpose.
Appropriateness of the study type and relevance to the focus of the review (empirical quantitative, qualitative or mixed methods).
Reliability of the results in relation to the focus of this review (trusthworthiness of findings for qualitative findings; reliability/generalisability of findings for quantitative results).
The interrater reliability value was calculated using an item-by-item method, specifically by dividing the tally of agreements by the total number of agreements and disagreements, divided by 100 (Cooper et al., 2007 ). The average value for the interrater agreement was 89%.
Studies’ characteristics
Of the 90 included articles, 63 studies (70%) of the reviewed studies were focused on students’ experiences whereas 12% examined staff experiences and 18% considered both staff and student experiences. Figure 2 shows that 30 studies (32%) were conducted in the Medical and Health discipline, and 16 studies (18%) from Science, Technology, Engineering and Mathematics (STEM), 16 studies (11%) in Business and Management, 16 studies (18%) Arts and Humanities, and 18 studies (20%) that did not clearly specify discipline. Additionally, 65 studies (72%) used a survey method, 16 studies (18%) used interviews, 7 studies (8%) used focus groups, and 2 studies (2%) used mixed methods.
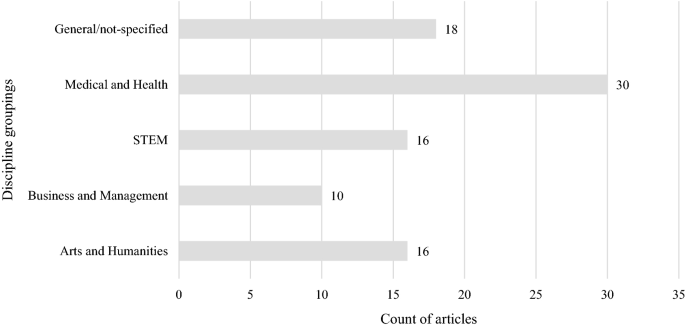
Disciplines covered in studies
A total of 87 studies (97%) examined adaptations to teaching and learning, 23 studies (26%) reported to adaptations to assessment and 2 (2%) around wider support in the response to COVID-19. A range of digital technologies were used and adapted—across synchronous and asynchronous teaching and learning, as well as in assessment (Table 1 ). Some studies focused on particular technologies and adaptations (Nel & Marais, 2021 ), but more commonly research was focused on the overall experiences of adaptation to online learning. The clarity of the level of acceptance and use of specific technologies pre-COVID-19 at each institution was provided in only a few studies, consequently making it challenging to determine the pre- and post-experiential changes in experience in response to adaptation of technology use.
Digital technology adaptation during COVID-19
Our review of the 90 articles revealed several characteristics common among students and staff in relation to adapting digital solutions during the COVID-19 pandemic. We categorized the identified sub-factors into four dimensions: Techno-Economic; Personal and Psychology; Teaching, Learning and Assessment Practice; and Social (see Table I in the supplementary file). Figure 3 outlines the dimensions, their sub-factors and article count.
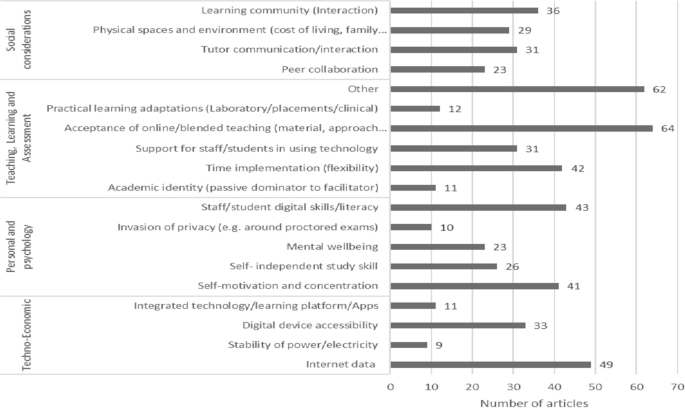
Dimensions and sub-factors affecting digital technology adaptation during COVID-19
Techno-economic
The Techno-Economic dimension encompassed a number of considerations: (1) infrastructure (macro factors that relate to utilities, such as internet and electricity), (2) the platforms and applications used as part of teaching, learning and assessment, as well as (3) more individual factors (such as access to hardware and affordability of access).
This review revealed that access to the internet was as an important influencing factor for both students and staff (N = 49, 54%)—with those with faster and more stable access having a more positive experience. Moreover, the level of access was not typified by country, with studies indicating both sufficient access and access frustrations in the same country; for example, in Germany—acceptance: (Schlenz et al., 2020 ) and frustrations: (Eberle & Hobrecht, 2021 ) were evident. Furthermore, the impact of contrasting levels of ease and quality of access between rural and urban areas was indicated by some studies—Calder et al. ( 2021 ) in New Zealand and Gautam and Gautam ( 2021 ) in Nepal. Additionally, sharing of connection in study places impacted on the quality of access (Costado Dios & Piñero Charlo, 2021 ). It was evident that those countries the existence of clear national policies around online learning (Müller et al., 2021 ) influenced the readiness to transition to online learning. Overall, these bandwidth considerations created an online environment typified by a lack of connection (Blackley et al., 2021 ). Moreover, such stability of access led to student frustrations, feelings of isolation and demotivation about their studies, and potentially to their academic achievement.
Equally, the cost of increased internet usage was highlighted as a barrier and strain on families’ finances, even in countries where the network providers offered a free data bundle for educational sites it was not sufficient (Ogbonnaya et al., 2020 ). This review showed that adaptations made in these more challenging situations saw a move to asynchronous (rather than synchronous) delivery to remove some of these anxieties (Ghazi-Saidi et al., 2020 ), but in the Emergency Remote Teaching phase then this was not always possible.
Additionally, online learning requires greater consumption of electricity and in some studies (N = 9) and countries this was an issue—whether this was that electricity network had capacity issues (e.g., in South Africa and load-shedding) or whether unstable (Bordoloi et al., 2021 ; Laher et al., 2021 ). However, even in some countries with unstable supply, students did not see this as a significant contributing factor (Ogbonnaya et al., 2020 ), perhaps reflecting that they had already developed strategies to manage such issues.
In terms of use of platforms and applications, the results also showed that enhanced efficiency in handling assignments for staff (Chen et al., 2021 ), as well as increased use of online formative and summative tests were evident (Laher et al., 2021 ). The use of different forms of content and complementary apps was evident through the use of tools such as Net.Create and Perusall (Craig et al., 2020 ; Nel & Marais, 2021 ). However, a proliferation of different apps and lack of consistency between different lecturers and courses created challenges for the student experience (Ghazi-Saidi et al., 2020 ; Oliveira et al., 2021 ). Moreover, platforms became unstable due to heavy use, and financial implications for students to access different apps impacted on their teaching and learning experience. Some of these platform challenges were related to Emergency Response Teaching early in the pandemic.
At a more individual level, then access to appropriate devices was required, ranging from smartphones to tablets and to laptops and computers. The level of access to such a device was related to each student’s socio-economic status and influenced their level of satisfaction (Al-Salman & Haider, 2021 ). Some universities provided discounted hardware and software to their students (Ghazi-Saidi et al., 2020 ), but this was not always possible. There were many challenges, particularly in pivoting online, that included i) hardware that was not suitable for online learning, ii) that apps were not compatible with smartphones (that were used heavily), iii) difficulty in maintaining devices (due to lockdown) as well as iv) financial constraints on buying a new device (when incomes had dropped). Such challenges had the potential to exclude students due to a lack of suitable devices, which in turn created anxieties for students about their studies and about graduating.
Personal and psychological
This dimension referred to the personal skills (motivation and independent learning skills), and psychological status (mental health) to cope with online learning. Several studies (N = 41, 46%) demonstrated that students were likely to experience some difficulties in managing their own study (Abou-Khalil et al., 2021 ; Hijazi & Alnatour, 2021 ; Rizvi & Nabi, 2021 ; Ruiz et al., 2021 ). Weak motivation for engaging with online learning and lack of concentration were found to be the significant issues for students adapting to online learning (Al-Tarawneh et al., 2021 ; Lassoued et al., 2020 ). Students were also distracted by their family responsibilities, (e.g., home schooling and caring) and a physically uncomfortable and chaotic home environment (Al-Rasheed, 2021 ; Gonçalves et al., 2020 ). These experiences were also shared by the members of staff, whose productivity was reduced due to the difficulties in concentrating on remote classes and multi-tasking. In addition, some studies (N = 26, 29%) also explored to what extent the students’ learning effectiveness had been affected by the independent study skills, such as self-regulated learning (Ogbonnaya et al., 2020 ), problem-solving skills (Eberle & Hobrecht, 2021 ), self-efficacy (Martha et al., 2021 ), and time management skill (Almazova et al., 2020 ; Ogbonnaya et al., 2020 ). Students with better independent study skills were more active in approaching tutors for support and, as a result, enjoyed the online teaching more (Müller et al., 2021 ).
Additionally, 26% of the studies highlighted the importance of considering mental wellbeing. Online learning reduced interaction between peers and tutors which heightened anxieties and stress, even though chat and communication were still possible for students and staff through various channels. Students reported that they felt stressed and anxious for their academic achievement, employability, health, and work-life balance (Secundo et al., 2021 ; Sugino, 2021 ; Watermeyer et al., 2021 ). Students at master's level experienced more angst than those at undergraduate level, as they took more responsibility for their financial arrangement and were worried the pandemic would delay the process of rebuilding their formal career (Gautam & Gautam, 2021 ). In addition, students pointed to their discomfort with the proctored online exam and the intimidating monitoring systems (Chen et al., 2021 ) that universities had introduced to maintain academic integrity of assessments, particularly examinations. Such systems heightened students’ stress levels, as it might over-stretch the availability of the internet data and violate students’ privacy (Morgan et al., 2021 ).
The findings (N = 43, 48%) showed that students and staff’s digital skills—the ability to work with various apps, software, and search for e-resources contents—improved significantly since the onset of adapted teaching and learning approaches (Händel et al., 2020 ; Khalaf et al., 2020 ). A notable number of students and staff demonstrated their confidence in using digital devices, learning platforms and apps essential for their teaching and learning, especially in those universities that provided sufficient training and support (Casacchia et al., 2021 ; Ghazi-Saidi et al., 2020 ; Stewart & Lowenthal, 2021 ). However, some students were less prepared to use various technologies in the sudden transition (Al-Rasheed, 2021 ; Colfer et al., 2021 ), and more staff over 55 years old also required extra instruction and IT support (Almazova et al., 2020 ).
Teaching, learning, and assessment
This dimension related to the changes to staff’s self-concept when engaged in online learning, as well as the views and outcomes of support in moving online. This dimension also involved the acceptance of online learning and specific technology adaptations in particular discipline areas. Several studies (N = 11, 12%) examined the staff’s motivation and any perceived adaptations to their academic identity. Whilst for some this represented a new ‘intellectual challenge’ and an opportunity to master a different form of teaching, (Almazova et al., 2020 ; Müller et al., 2021 ; Secundo et al., 2021 ), other studies felt that the move challenged the ‘core academic values’ and purpose of a university and inhibited ‘holistic learning’ (Müller et al., 2021 ). Moreover, some staff felt that they had become more like technicians and that teaching and learning have become passive (Hijazi & Alnatour, 2021 ; Müller et al., 2021 ; Watermeyer et al., 2021 ).
The flexibility of online learning was strongly identified (N = 42, 47%) with time and cost-savings being outlined (e.g., lack of commuting), more strongly for working students (Casacchia et al., 2021 ; Costado Dios & Piñero Charlo, 2021 ; Gautam & Gautam, 2021 ). Moreover, online meant that the schedule was no longer dictated by physical spaces on campus, so allowing flexibility with the endpoint of sessions (Toader et al., 2021 ). Additionally, the options to self-pace were both appreciated (Istenič, 2021 ; Kasai et al., 2021 ) and not appreciated (Laher et al., 2021 ). In particular, the ability to replay recorded videos was identified as allowing students the opportunity to master concepts by re-listening and being able to control the speed of playback. However, the resultant balancing of personal and academic time was impacted—with lecturers spending more time on preparing materials and students indicating increased workloads and distractions to their learning at home (Al-Rasheed, 2021 ; Oliveira et al., 2021 ; Stewart et al., 2021 ).
Support for staff and students (N = 31, 34%) was another factor, with positive institutional support being associated with a more positive perception of online learning (Al-Karaki et al., 2021 ; Mouchantaf, 2020 ). This support came in the form of (a)synchronous training, technical support, and peer support (building stronger connections between academic colleagues through necessity). Conversely a lack of support for staff resulted in a perception of teaching preparation taking too long, thereby creating negative views and barriers to acceptance of online learning (Hayat et al., 2021 ; Lassoued et al., 2020 ). Studies identified the greater pastoral role the academic staff had undertaken (Watermeyer et al., 2021 ), in part due to lack of access to student support services (Istenič, 2021 ), which increased staff workload further. Going forward, staff and students need to be supported in how to work in a digital work and learning environment, and doing so would equip both groups with relevant transversal skills (Almazova et al., 2020 ).
Approaches and adaptations associated with clinical and practical work indicated innovative adaptations—in the use simulated electronic health records (Kasai et al., 2021 ), simulated GP clinics (Rasalam & Bandaranaike, 2020 ) and VR simulations (De Ponti et al., 2020 )—but not all disciplines were able to find suitable alternatives. Several papers viewed online learning as being appropriate for the theoretical and written practice elements of a programme, but did not believe that they could replace preparation for practical aspects, such as clinical work, medical interviews, laboratory practice, engineering design, and laboratories (Ahmed et al., 2020 ). These studies reflected discipline differences around acceptance of online learning, with Arts and Humanities having a higher acceptance of online learning in the future, and Sciences, Engineering, Health, Medicine and Languages expressed concerns and barriers about completely online education (Al-Salman & Haider, 2021 ). A mixed mode of online and face-to-face emerged from these studies (with more acceptance of online for theoretical aspects), and opportunities to innovate further with the use of simulation, VR, and other tools. Such modality would align with active forms of instruction that are known to be more engaging.
The acceptance and adaptation to online learning was influenced by the level of study, as studies highlighted students in higher levels of undergraduate and in postgraduate study coped better with the move online, whereas level one and two students found the transition more difficult (Khalil et al., 2020 ; Klein et al., 2021 ; Yu, 2021 ). Such differences potentially reflected a lack of familiarity with systems and culture of the university of newer students, as well as readiness to engage in online instruction.
Adaptations to assessments were identified in 23 papers. Students liked unproctored, open-book examinations that encouraged deeper thinking and considered real-world applications (Chen et al., 2021 ; Morgan et al., 2021 ). Studies recognised the importance of academic integrity (and the need for proctored examinations) thereby creating a conundrum that will need to be addressed to ensure fair outcomes (Müller et al., 2021 ; Reedy et al., 2021 ). In terms of online examinations, particular difficulties were evident in the sciences (Al-Salman & Haider, 2021 ; Elfirdoussi et al., 2020 ; Reedy et al., 2021 ) and academics were not convinced by the integrity of online assessments (Al-Karaki et al., 2021 ).
This dimension consisted of four sub factors, which are (1) peer collaboration (N = 23, 26%), (2) Tutor Communication and interaction (N = 31, 34%), (3) Physical space and environment (N = 29, 32%), and (4) Learning community interaction (N = 36, 40%). Firstly, students acknowledged that staff’s availability to take students’ questions expanded through the adoption of multi-communication channels in online learning environment (Brooks et al. 2021 ; Müller et al., 2021 ; Stewart & Lowenthal, 2021 ), and they could receive a rapid response to their inquiries from their tutor (Al-Balas et al., 2020 ). Student-staff interaction has been enhanced in the synchronised classes, academic staff adopted different teaching techniques such as feedback, online activities apps (e.g., Qualtrics) to enable students to follow the learning easily (Lambert & Rennie, 2021 ). Moreover, students can benefit from these initiatives and gain more opportunities to communicate with their tutors confidently, especially those students who were very shy in the traditional face to face learning environment (Müller et al., 2021 ). On the contrary, some papers highlighted the difficulties in interacting with students online, including inability to check students’ understanding when their cameras are turned off (Toader et al., 2021 ), unwillingness to engage with online chat function due to the anxiety of being judged by peers (Blackley et al., 2021 ), and limited time to interact due to the substantial number of participants in synchronized class (Ahmed et al., 2020 ; Johnson et al., 2020 ). Findings also demonstrated that some of the staff did not adjust their teaching style and were unable to multitask to answer the questions in the chat during the online teaching (Khairi et al., 2021 ), consequently, demotivating students to interact with teachers.
Online learning allows students to choose the place where they would like to conduct their study. Benefits include time- and cost-savings (as mentioned already) and comfort of their chosen learning space (Abou-Khalil et al., 2021 ; Gautam & Gautam, 2021 ), and spending more time with their families, who acted as important part of the coping mechanism to ensure their mental wellness (Louis et al., 2021 ). However, several studies also disclosed the limited and chaotic learning space that hinder students’ motivation and their mental health, especially for those students who lived in small apartments and far away from their families (Gonçalves et al., 2020 ; Martha et al., 2021 ; Tavitiyaman et al., 2021 ). Constant disruption caused by the family dynamics, unstable in-house internet connection, increased chores at home made it extremely difficult for students to concentrate on their study (Gautam & Gautam, 2021 ; Ogbonnaya et al., 2020 ; Rizvi & Nabi, 2021 ).
Finally, studies revealed that students desired to connect and bond with their classmates, as the sense of learning community and solidarity among them can enhance motivation to actively engage in the online activities (Almazova et al., 2020 ; Chen et al., 2021 ; Frolova et al., 2021 ; Sugino, 2021 ). However, twenty-three papers reported that students failed to interact with their peers (Fatani, 2020 ; Gautam & Gautam, 2021 ; Händel et al., 2020 ; Hayat et al., 2021 ), due to the difficulties in agreeing on the meeting time for group work (Al-Rasheed, 2021 ), and uneven contributions among the team members (Lambert & Rennie, 2021 ).
Potential initiatives in the post-COVID 19 period
This study found that 28 articles (31%) had specific and clear considerations and recommendations, which were used (along with implications of key factors from the first research question) to identify key initiatives. These initiatives spanned infrastructure (national and institutional) and available resources, to institution level actions and finally around creating a supportive learning environment with engaged learners. A holistic consideration is presented here, as dimensions and sub-factors interact with each other.
Firstly, infrastructure aspects (whether national or institutional) were identified as influencing experiences of online learning above. Recommendations from studies indicated government-level responses—investment in Intranet and platform infrastructure (Ahmed et al., 2020 ; Al-Salman & Haider, 2021 ) and reduced costs of hardware (Şenol et al., 2021 ). Cross-institutional collaboration in developing approaches to online education (Lassoued et al., 2020 ), the creation and curation of Open Educational Resources (OERs) at national level (Bordoloi et al., 2021 ) to facilitate shared and public courses, and greater use of Open-Source digital learning apps (Elfirdoussi et al., 2020 ) were proposed.
In terms of institutional considerations, a mixture of off- and on-campus learning envisaged in the future would offer greater options to improve programme timetables, as fewer restrictions on availability of physical space would exist (Gautam & Gautam, 2021 ; Hijazi & Alnatour, 2021 ). Physical spaces could still to be used for specific purposes (around clinical, laboratory and development of inter-personal and psychomotor competences) and developing connections, but universities could consider the opportunity presented with any shift to blended learning. Greater provision of IT laboratories (Lassoued et al., 2020 ) and ebooks (Al-Rasheed, 2021 ; Bordoloi et al., 2021 ) is recommended, to address device access issues as well as affording social and study spaces. In the absence of gaining on-campus access, then universities need to consider affordable access to hardware and software (Calder et al., 2021 ; Majda et al., 2021 ), and potentially subsidised hardware and software (Ghazi-Saidi et al., 2020 ).
Enabling social connections should be supported by online learning, for example through break-out rooms (Calder et al., 2021 ), collaborative digital tools (Craig et al., 2020 ; Nel & Marais, 2021 ), and doing so in a creative manner (Rizvi & Nabi, 2021 ). Collaborative group projects (Ariza et al., 2020 ) have such potential, but staff must plan on group formation in team or zoom (Craig et al., 2020 ) reflecting these are new, shared learning spaces. Such new spaces have the potential to be more shared (staff and students) and to be more inclusive of the diversity of learners, such as more introverted learners (Yu, 2021 ). To achieve this, universities may consider adopting innovative pedagogy, collaborative, and engaging technology-enabled learning spaces (Chen et al., 2021 ). Such considerations will best inform what can and should be done synchronously and asynchronously (Martha et al., 2021 ), how to adapt technologies to sustain effective discipline pedagogical practices (Busto et al., 2021 ), how to develop essential computer-aided skills (Ayadat et al., 2021 ), how to support practical and competency-based education, and how to create authentic assessments that maintain the academic integrity of results (Reedy et al., 2021 ).
It is important that staff have been equipped with good level of digital ability to adapt the educational technologies in their teaching (Calder et al., 2021 ). Therefore, institutional policies and practices will need to be reviewed and updated to ensure sufficient staff digital skills development opportunity is provided. There will be also a need for specialised support, such as Instructional Designers (Johnson et al., 2020 ; Lassoued et al., 2020 ), along with ongoing training and support for staff to support adaptation and to help staff see technologies as opportunities to enhance the learning experience and their professional practice.
Equally for students, support is a key initiative that must be taken forward. Developing self-regulated behaviours (SRBs), such as independent study, autonomy, and time management skills (Gonçalves et al., 2020 ; Montano, 2021 ), enhancing resilience and self-efficacy, as well as in digital capabilities will be required (Mok et al., 2021 ). A mixture of pedagogically-aligned synchronous and asynchronous learning opportunities provides an opportunity for these SRBs to grow, as the right mix will balance self-management with scaffolded learning. Adjustment of this balance across distinct levels (or years) of study to support transition and competency enhancement is vitally important. In terms of digital capabilities, the embedding of technology courses (Şenol et al., 2021 ) and use of technology throughout the curricula, as well as training (Rizvi & Nabi, 2021 ), has the potential to build confidence and a more positive perspective around technology-enabled learning. Providing these opportunities to recognise and develop the required meta- and transversal-skills will also underpin a better sense of mental wellbeing and of being in control, which will prevent students from becoming anxious; students then have the potential to develop more positive adaptation strategies with enhanced longer-term outcomes. Moreover, these are important skills in the contemporary workplace.
Innovative adaptations have emerged, some of which have ongoing potential and benefits: use of VR and simulation for medical and engineering courses and in Work-Integrated Learning (Almohammed et al., 2021 ; De Ponti et al., 2020 ; Iipinge et al., 2020 ; Rasalam & Bandaranaike, 2020 ); hybrid teaching (in-class and online) (Busto et al., 2021 ); online assessments (Al-Karaki et al., 2021 ; Oliveira et al., 2021 ; Reedy et al., 2021 ), as well as those mentioned already above. These innovations have offered new ways of achieving positive outcomes (opportunity of mastery through re-play, more time for discussion, efficiency in assignment management, safe environments to practice and learn). However, care must be taken to ensure that adoption and adaptation of any technology are consistent with creating a positive learning environment and do not create unnecessary anxieties and exclude students (Chen et al., 2021 ).
Finally, the pivot to online has also brought to the fore, the key issue of accessibility—access to devices, access to internet, accessibility of provided learning materials and accessibility to fair assessments. At an institutional level, the application of universal design principles and practice (Ghazi-Saidi et al., 2020 ) to create accessible resources (Tavitiyaman et al., 2021 ) has the potential to impact positively on all students and to unleash the potential of online learning to provide universal availability of learning. To do so, universities must consider the socio-economic and geographically related circumstances of their students and staff.
Limitations and future works
Both sets of findings supported a multi-level conceptualisation of adaptation (Venkatesh et al., 2016 ) and demonstrated the impact of macro factors, such as location (associated national infrastructure, policy, and socio-economic conditions), and meso factors such as institutional context (e.g., management support; training availability and efficacy; experience of digital learning technologies), and physical/social environments (e.g., learning and teaching location). These macro and meso-level factors influenced individual factors (such as prior experience of using digital technologies, digital literacy levels, emotional coping skills). The determination of the strength and nature of interactions of these factors, and how they can explain the adaptations seen in response to COVID-19 was not explored in this systematic literature as these are more suited to a meta-analysis methodology. As such, it is recommended that educational policy pay more attention to the emotional-coping mechanisms and problem-focused responses of staff and students as a key to support the ongoing adaptation and learning outcomes.
Despite this, some limitations were identified in this systematic literature review. For example, this review did not compare how digital technology adaptations differentiate between diverse learners. An examination of experiences of learners from different educational levels, age and ethnic background could be conducted in the future. Also, students and staff in certain subjects faced more challenges in online teaching and learning than other subject areas, as not all the pedagogical face to face activities can be transferred to online format. Future research could also examine and compare what digital technologies have been adopted by various disciplines and its related impact. The identified dimensions and sub-factors in this review were based on certain qualitative and quantitative studies that we identified from searching the literature databases, which may skew the results and impact of COVID-19 to specific higher education settings/conditions. Additionally, it was not possible to track adaptations from one wave of lockdown to the next, due to a lack of longitudinal research. This review was also limited to previous empirical studies with sufficient sample sizes to ascertain the factors influencing digital technology adaptation during the COVID-19 pandemic. Therefore, future studies could include different sample sizes and populations. Evaluation of adaptations over the different waves would provide valuable insight into the process of adaptation at a large scale. Finally, papers were not always specific about their level of usage of technologies pre-COVID-19, or always focused on a particular technology and its adaptation in one case. Consequently, targeted studies examining adaptation of impactful technologies from a staff and student perspective across different institutions would enhance the understanding of digital technology adaptation in Higher Education.
This study reviewed 90 articles to identify the main dimensions and initiatives related to the use of digital technologies during the COVID-19 period. Four dimensions were identified in this work (in relation to first research question): techno-economic; personal and psychological; teaching, learning and assessment; and social. Whilst expected dimensions (such as ease of access, connection between students and staff, self-management, and support) were evident in this systematic review, interesting patterns emerged, such as importance of physical space in online learning, balancing standardization of platforms and applications with need for channels to communicate and engage in the learning community, and flexibility in timetabling (as not related to physical classrooms).
Initiatives (as per the second research question) identified covered national, institutional and individual levels. A clear future practical direction at a national level needs educational policies to recognise online-learning as an effective form of education, and the creation of appropriate national digital learning eco-systems and infrastructure for benefits of scale and consistency. Also, investment in national teaching open educational resources and provision of the framework that aligns these resources with available device and network capabilities is required. At institutional level, policies need to support the creation of pedagogically-underpinned teaching, learning and assessment with the appropriate management support and positive culture to enable staff and students to positively engage with online learning. Additionally, universities need to identify and progress innovation adaptations that have the potential for wider and impactful implementation. Also, mechanisms to support the mental wellbeing issues of staff and students are essential. Finally, universities must gain a deeper individualized perspective on how university infrastructure enables learning for students.
In conclusion, the four dimensions and sub-factors identified in this study overlapped with current models of adoption and adaptation, but this review did not establish the interconnection between these factors. However, the extant models can offer some explanatory and planning insight as universities navigate their way through the ongoing pandemic.
Abou-Khalil, V., Helou, S., Khalifé, E., Chen, M. A., Majumdar, R., & Ogata, H. (2021). Emergency online learning in low-resource settings: Effective student engagement strategies. Education Sciences, 11 (1), 1–18. https://doi.org/10.3390/educsci11010024
Article Google Scholar
Ahmed, S. A., Hegazy, N. N., Abdel Malak, H. W., Kayser, W. C., III., Elrafie, N. M., Hassanien, M., Al-Hayani, A. A., El Saadany, S. A., Ai-Youbi, A. O., & Shehata, M. H. (2020). Model for utilizing distance learning post COVID-19 using (PACT)™ a cross sectional qualitative study. BMC Medical Education, 20 , 1–13. https://doi.org/10.1186/s12909-020-02311-1
Al-Balas, M., Al-Balas, H. I., Jaber, H. M., Obeidat, K., Al-Balas, H., Aborajooh, E. A., Al-Taher, R., & Al-Balas, B. (2020). Distance learning in clinical medical education amid COVID-19 pandemic in Jordan: Current situation, challenges, and perspectives. BMC Medical Education, 20 (1), 341. https://doi.org/10.1186/s12909-020-02257-4
Al-Karaki, J. N., Ababneh, N., Hamid, Y., & Gawanmeh, A. (2021). Evaluating the effectiveness of distance learning in higher education during covid-19 global crisis: Uae educators’ perspectives. Contemporary Educational Technology . https://doi.org/10.30935/cedtech/10945
Al-Rasheed, A. (2021). The challenges faced by undergraduate women during the COVID-19 pandemic in Saudi Arabia. Education Research International . https://doi.org/10.1155/2021/8841997
Al-Salman, S., & Haider, A. S. (2021). Jordanian university students’ views on emergency online learning during covid-19. Online Learning Journal, 25 (1), 286–302. https://doi.org/10.24059/olj.v25i1.2470
Al-Tarawneh, L., Al-Nasah, M., & Awwad, F. A. (2021). The Effect of the COVID-19 Pandemic among Undergraduate Engineering Students in Jordanian Universities: Factors Impact Students’ Learning Satisfaction. 2021 Innovation and New Trends in Engineering, Technology and Science Education Conference, IETSEC 2021,
Almazova, N., Krylova, E., Rubtsova, A., & Odinokaya, M. (2020). Challenges and opportunities for Russian higher education amid covid-19: Teachers’ perspective [Article]. Education Sciences, 10 (12), 1–11. https://doi.org/10.3390/educsci10120368
Almohammed, O. A., Alotaibi, L. H., & Ibn Malik, S. A. (2021). Student and educator perspectives on virtual institutional introductory pharmacy practice experience (IPPE). BMC Medical Education . https://doi.org/10.1186/s12909-021-02698-5
Ariza, H. M., Martínez Sarmiento, F. H., & Castillo, H. G. (2020). Connectivity characteristics and level of acceptance linked to online learning by higher education students during the confinement generated by the Covid-19 pandemic. International Journal of Engineering Research and Technology, 13 (8), 1934–1939. https://doi.org/10.37624/ijert/13.8.2020.1934-1939
Ayadat, T., Khasawneh, M. A., Chowdhury, S. R., Nayeemuddin, M., Ahmed, D., & Asiz, A. (2021). Effects of students’ home environment, tools, and technology used on online learning experience in a civil engineering program. International Journal of Information and Education Technology, 11 (8), 356–367. https://doi.org/10.18178/ijiet.2021.11.8.1535
Bala, H., & Venkatesh, V. (2016). Adaptation to information technology: A holistic nomological network from implementation to job outcomes. Management Science, 62 (1), 156–179.
Blackley, S., Wilson, S., Sheffield, R., Murcia, K., Brown, P., Tang, K. S., Cooper, M., & Williams, J. (2021). How have covid-19-related changes to tuition modes impacted face-to-face initial teacher education students? Issues in Educational Research, 31 (2), 421–439.
Google Scholar
Boddy, C. R. (2016). Sample size for qualitative research. Qualitative Market Research: an International Journal, 19 (4), 426–432.
Bordoloi, R., Das, P., & Das, K. (2021). Perception towards online/blended learning at the time of Covid-19 pandemic: An academic analytics in the Indian context. Asian Association of Open Universities Journal, 16 (1), 41–60. https://doi.org/10.1108/AAOUJ-09-2020-0079
Brooks, J. V. C., Glendon, G., Averett, E., & Hughes, D. (2021). Teaching during the COVID- 19 pandemic: MHSA faculty experiences. Journal of Health Administration Education, 38 (1), 265–284.
Busto, S., Dumbser, M., & Gaburro, E. (2021). A simple but efficient concept of blended teaching of mathematics for engineering students during the COVID-19 pandemic. Education Sciences, 11 (2), 56. https://doi.org/10.3390/educsci11020056
Calder, N., Jafri, M., & Guo, L. (2021). mathematics education students’ experiences during lockdown: Managing collaboration in eLearning. Education Sciences, 11 (4), 191. https://doi.org/10.3390/educsci11040191
Casacchia, M., Cifone, M. G., Giusti, L., Fabiani, L., Gatto, R., Lancia, L., Cinque, B., Petrucci, C., Giannoni, M., & Ippoliti, R. (2021). Distance education during COVID 19: An Italian survey on the university teachers’ perspectives and their emotional conditions. BMC Medical Education, 21 (1), 1–17.
Chen, C., Landa, S., Padilla, A., & Yur-Austin, J. (2021). Learners’ experience and needs in online environments: Adopting agility in teaching. Journal of Research in Innovative Teaching & Learning . https://doi.org/10.1108/JRIT-11-2020-0073
Colfer, B. P., Johri, N., & Wagner, S. L. (2021). A case study of MHA faculty and student experiences in adapting learning modality options to hybrid flexible (HyFlex) during the COVID-19 pandemic. Journal of Health Administration Education, 38 (1), 441–466.
Cooper, J. O., Heron, T. E., & Heward, W. L. (2007). Applied behavior analysis (2nd ed.). Pearson/Merrill/Prentice-Hall.
Costado Dios, M. T., & Piñero Charlo, J. C. (2021). Face-to-face vs. E-learning models in the COVID-19 Era: Survey research in a Spanish University. Education Sciences, 11 (6), 293.
Craig, K., Humburg, M., Danish, J. A., Szostalo, M., Hmelo-Silver, C. E., & McCranie, A. (2020). Increasing students’ social engagement during COVID-19 with Net. Create: Collaborative social network analysis to map historical pandemics during a pandemic. Information and Learning Sciences, 121 , 533–547.
De Ponti, R., Marazzato, J., Maresca, A. M., Rovera, F., Carcano, G., & Ferrario, M. M. (2020). Pre-graduation medical training including virtual reality during COVID-19 pandemic: A report on students’ perception. BMC Medical Education, 20 , 1–7. https://doi.org/10.1186/s12909-020-02245-8
Deng, J., Zhou, F., Hou, W., Silver, Z., Wong, C. Y., Chang, O., Drakos, A., Zuo, Q. K., & Huang, E. (2021). The prevalence of depressive symptoms, anxiety symptoms and sleep disturbance in higher education students during the COVID-19 pandemic: A systematic review and meta-analysis. Psychiatry Research, 301 , 113863. https://doi.org/10.1016/j.psychres.2021.113863
Eberle, J., & Hobrecht, J. (2021). The lonely struggle with autonomy: A case study of first-year university students’ experiences during emergency online teaching. Computers in Human Behavior, 121 , 106804. https://doi.org/10.1016/j.chb.2021.106804
Elfirdoussi, S., Lachgar, M., Kabaili, H., Rochdi, A., Goujdami, D., & El Firdoussi, L. (2020). Assessing distance learning in higher education during the COVID-19 pandemic. Education Research International . https://doi.org/10.1155/2020/8890633
Fatani, T. H. (2020). Student satisfaction with videoconferencing teaching quality during the COVID-19 pandemic. BMC Medical Education, 20 (1), 1–8.
Ficko, A., Lidestav, G., Dhubháin, Á. N., Karppinen, H., Zivojinovic, I., & Westin, K. (2019). European private forest owner typologies: A review of methods and use. Forest Policy and Economics, 99 , 21–31.
Frolova, E. V., Rogach, O. V., Tyurikov, A. G., & Razov, P. V. (2021). Online Student Education in a Pandemic: New Challenges and Risks. European Journal of Contemporary Education, 10 (1), 43–52. https://doi.org/10.13187/ejced.2021.1.43
Gautam, D. K., & Gautam, P. K. (2021). Transition to online higher education during COVID-19 pandemic: Turmoil and way forward to developing country of South Asia-Nepal. Journal of Research in Innovative Teaching & Learning, 14 (1), 93–111. https://doi.org/10.1108/JRIT-10-2020-0051
Ghazi-Saidi, L., Criffield, A., Kracl, C. L., McKelvey, M., Obasi, S. N., & Vu, P. (2020). Moving from face-to-face to remote instruction in a higher education institution during a pandemic: Multiple case studies. International Journal of Technology in Education and Science, 4 (4), 370–383.
Gonçalves, S. P., Sousa, M. J., & Pereira, F. S. (2020). Distance learning perceptions from higher education students—the case of Portugal. Education Sciences, 10 (12), 374.
Hattar, S., AlHadidi, A., Sawair, F. A., Alraheam, I. A., El-Ma’aita, A., & Wahab, F. K. (2021). Impact of COVID-19 pandemic on dental education: Online experience and practice expectations among dental students at the University of Jordan. BMC Medical Education, 21 (1), 1–10.
Händel, M., Stephan, M., Gläser-Zikuda, M., Kopp, B., Bedenlier, S., & Ziegler, A. (2020). Digital readiness and its effects on higher education students’ socio-emotional perceptions in the context of the COVID-19 pandemic. Journal of Research on Technology in Education . https://doi.org/10.1080/15391523.2020.1846147
Hayat, A. A., Keshavarzi, M. H., Zare, S., Bazrafcan, L., Rezaee, R., Faghihi, S. A., Amini, M., & Kojuri, J. (2021). Challenges and opportunities from the COVID-19 pandemic in medical education: A qualitative study. BMC Medical Education, 21 (1), 247. https://doi.org/10.1186/s12909-021-02682-z
Hijazi, D., & Alnatour, A. (2021). Online learning challenges affecting students of english in an EFL context during covid-19 pandemic. International Journal of Education and Practice, 9 (2), 379–395. https://doi.org/10.18488/journal.61.2021.92.379.395
Iipinge, S. M., Batholmeus, P. N., & Pop, C. (2020). Using simulations to improve skills needed for work-integrated learning before and during COVID-19 in Namibia. International Journal of Work - Integrated Learning, 21 (5), 531–543.
Istenič, A. (2021). Online learning under COVID-19: Re-examining the prominence of video-based and text-based feedback. Educational Technology Research and Development, 69 (1), 117–121. https://doi.org/10.1007/s11423-021-09955-w
Johnson, N., Veletsianos, G., & Seaman, J. (2020). U.S. faculty and administrators’ experiences and approaches in the early weeks of the COVID-19 pandemic. Online Learning Journal, 24 (2), 6–21. https://doi.org/10.24059/olj.v24i2.2285
Kasai, H., Shikino, K., Saito, G., Tsukamoto, T., Takahashi, Y., Kuriyama, A., Tanaka, K., Onodera, M., Yokoh, H., Tatusmi, K., Yoshino, I., Ikusaka, M., Sakao, S., & Ito, S. (2021). Alternative approaches for clinical clerkship during the COVID-19 pandemic: Online simulated clinical practice for inpatients and outpatients—A mixed method. BMC Medical Education, 21 , 1–13. https://doi.org/10.1186/s12909-021-02586-y
Kelley, K., Clark, B., Brown, V., & Sitzia, J. (2003). Good practice in the conduct and reporting of survey research. International Journal for Quality in Health Care, 15 (3), 261–266. https://doi.org/10.1093/intqhc/mzg031
Khairi, M. A. M., Faridah, I., Norsiah, H., & Zaki, M. A. A. (2021). Preliminary study on readiness to teach online due to covid-19 pandemic among university academician in Malaysia. International Journal of Information and Education Technology, 11 (5), 212–219. https://doi.org/10.18178/ijiet.2021.11.5.1514
Khalaf, K., El-Kishawi, M., Moufti, M. A., & Al Kawas, S. (2020). Introducing a comprehensive high-stake online exam to final-year dental students during the COVID-19 pandemic and evaluation of its effectiveness. Medical Education Online, 25 (1), 1826861. https://doi.org/10.1080/10872981.2020.1826861
Khalil, R., Mansour, A. E., Fadda, W. A., Almisnid, K., Aldamegh, M., Al-Nafeesah, A., Azzam, A., & Al-Wutayd, O. (2020). The sudden transition to synchronized online learning during the COVID-19 pandemic in Saudi Arabia: A qualitative study exploring medical students’ perspectives. BMC Medical Education, 20 , 1–10. https://doi.org/10.1186/s12909-020-02208-z
Klein, P., Ivanjek, L., Dahlkemper, M. N., Jeličić, K., Geyer, M. A., Küchemann, S., & Susac, A. (2021). Studying physics during the COVID-19 pandemic: Student assessments of learning achievement, perceived effectiveness of online recitations, and online laboratories. Physical Review. Physics Education Research . https://doi.org/10.1103/PhysRevPhysEducRes.17.010117
Korstjens, I., & Moser, A. (2018). Series: Practical guidance to qualitative research. Part 4: Trustworthiness and publishing. European Journal of General Practice, 24 (1), 120–124.
Laher, S., Bain, K., Bemath, N., de Andrade, V., & Hassem, T. (2021). Undergraduate psychology student experiences during COVID-19: Challenges encountered and lessons learnt. South African Journal of Psychology, 51 (2), 215–228. https://doi.org/10.1177/0081246321995095
Lambert, C. G., & Rennie, A. E. W. (2021). Experiences from COVID-19 and emergency remote teaching for entrepreneurship education in engineering programmes. Education Sciences . https://doi.org/10.3390/educsci1106028210.3390/educsci11060282
Lassoued, Z., Alhendawi, M., & Bashitialshaaer, R. (2020). An Exploratory study of the obstacles for achieving quality in distance learning during the COVID-19 pandemic. Education Sciences, 10 (9), 232. https://doi.org/10.3390/educsci10090232
Liberati, A., Altman, D. G., Tetzlaff, J., Mulrow, C., Gøtzsche, P. C., Ioannidis, J. P., Clarke, M., Devereaux, P. J., Kleijnen, J., & Moher, D. (2009). The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. Journal of Clinical Epidemiology, 62 (10), e1–e34.
Louis, C. J., Landry, A., Silvera, G., Robbins, J., Shay, P., Lee, H., Felix, J., Cave, S., & Fishman, P. (2021). The COVID-19 impact on health administration education: Understanding student perspectives on the transition from in-person to remote course instruction. Journal of Health Administration Education, 38 (1), 247–264.
Maddumapatabandi, T. D., & Gamage, K. A. (2020). Novel coronavirus (COVID-2019) pandemic: Common challenges and response from higher education providers. Journal of Applied Learning and Teaching, 3 (2), 1–11.
Martha, A. S. D., Junus, K., Santoso, H. B., & Suhartanto, H. (2021). Assessing undergraduate students’ e-learning competencies: A case study of higher education context in Indonesia. Education Sciences, 11 (4), 189. https://doi.org/10.3390/educsci11040189
Mok, K. H., Xiong, W., & Bin Aedy Rahman, H. N. (2021). COVID-19 pandemic’s disruption on university teaching and learning and competence cultivation: Student evaluation of online learning experiences in Hong Kong. International Journal of Chinese Education . https://doi.org/10.1177/22125868211007011
Montano, R. L. T. (2021). Academic engagement predicts flourishing among students in online learning setup: The mediating role of psychological needs. Journal of Psychological and Educational Research, 29 (1), 177–194.
Morgan, K., Adams, E., Elsobky, T., Darr, A., & Brackbill, M. (2021). Moving assessment online: Experiences within a school of pharmacy. Online Learning, 25 (1), 245–252.
Mouchantaf, M. (2020). The covid-19 pandemic: Challenges faced and lessons learned regarding distance learning in Lebanese higher education institutions. Theory and Practice in Language Studies, 10 (10), 1259–1266. https://doi.org/10.17507/tpls.1010.11
Mseleku, Z. (2020). A literature review of E-learning and E-teaching in the era of Covid-19 pandemic. International Journal of Innovative Science and Research Technology, 57 , 588–597.
Müller, A. M., Goh, C., Lim, L. Z., & Gao, X. (2021). Covid-19 emergency elearning and beyond: Experiences and perspectives of university educators. Education Sciences, 11 (1), 1–15. https://doi.org/10.3390/educsci11010019
Nel, C., & Marais, E. (2021). Addressing the wicked problem of feedback during the teaching practicum. Perspectives in Education, 39 (1), 410–426. https://doi.org/10.18820/2519593X/pie.v39.i1.25
Oakleaf, M. (2009). Writing information literacy assessment plans: A guide to best practice.
Ogbonnaya, U. I., Awoniyi, F. C., & Matabane, M. E. (2020). Move to online learning during covid-19 lockdown: Pre-service teachers’ experiences in Ghana. International Journal of Learning, Teaching and Educational Research, 19 (10), 286–303. https://doi.org/10.26803/IJLTER.19.10.16
Oliveira, G., Grenha Teixeira, J., Torres, A., & Morais, C. (2021). An exploratory study on the emergency remote education experience of higher education students and teachers during the COVID-19 pandemic. British Journal of Educational Technology, 52 (4), 1357–1376. https://doi.org/10.1111/bjet.13112
Petherbridge, D. T. (2007). A concerns-based approach to the adoption of web-based learning management systems. Doctoral thesis, North Carolina State University] Raleigh. https://repository.lib.ncsu.edu/bitstream/handle/1840.16/3941/etd.pdf?isAllowed=y&sequence=1
Rasalam, R., & Bandaranaike, S. (2020). Virtual WIL clinics in medicine: Overcoming the COVID-19 challenge. International Journal of Work-Integrated Learning, 21 (5), 573–585.
Reedy, A., Pfitzner, D., Rook, L., & Ellis, L. (2021). Responding to the COVID-19 emergency: Student and academic staff perceptions of academic integrity in the transition to online exams at three Australian universities. International Journal for Educational Integrity, 17 (1), 9. https://doi.org/10.1007/s40979-021-00075-9
Rizvi, Y., & Nabi, A. (2021). Transformation of learning from real to virtual: An exploratory-descriptive analysis of issues and challenges. Journal of Research in Innovative Teaching & Learning . https://doi.org/10.1108/JRIT-10-2020-0052
Ruiz, L. M. S., Moll-López, S., Moraño-Fernández, J. A., & Llobregat-Gómez, N. (2021). B-learning and technology: Enablers for university education resilience. An experience case under COVID-19 in Spain. Sustainability, 13 (6), 3532. https://doi.org/10.3390/su13063532
Sebbani, M., Adarmouch, L., Mansouri, A., Mansoury, O., Michaud, S., ElAdib, A. R., Bouskraoui, M., & Amine, M. (2021). Implementation of online teaching in medical education: Lessons learned from students’ perspectives during the health crisis in Marrakesh, Morocco. Education Research International, 2021 , 1–9. https://doi.org/10.1155/2021/5547821
Schlenz, M. A., Schmidt, A., Wöstmann, B., Krämer, N., & Schulz-Weidner, N. (2020). Students’ and lecturers’ perspective on the implementation of online learning in dental education due to SARS-CoV-2 (COVID-19): A cross-sectional study. BMC Medical Education, 20 , 1–7. https://doi.org/10.1186/s12909-020-02266-3
Secundo, G., Mele, G., Vecchio, P. D., Elia, G., Margherita, A., & Ndou, V. (2021). Threat or opportunity? A case study of digital-enabled redesign of entrepreneurship education in the COVID-19 emergency. Technological Forecasting and Social Change, 166 , 120565. https://doi.org/10.1016/j.techfore.2020.120565
Şenol, H., Lesinger, F. Y., & Çaglar, M. (2021). Evaluation of online education delivered by the universities during pandemic COVID-19: A case of North Cyprus. TOJET: the Turkish Online Journal of Educational Technology, 20 (2), 51–61.
Stewart, B. L., Goodson, C. E., & Miertschin, S. L. (2021). Pandemic online transitions: Student reactions, adaptations, and course feature preferences. Journal of Higher Education Theory and Practice, 21 (1), 38–52.
Stewart, W. H., & Lowenthal, P. R. (2021). Distance education under duress: A case study of exchange students’ experience with online learning during the COVID-19 pandemic in the Republic of Korea. Journal of Research on Technology in Education . https://doi.org/10.1080/15391523.2021.1891996
Sugino, C. (2021). Student perceptions of a synchronous online cooperative learning course in a Japanese women’s university during the COVID-19 pandemic. Education Sciences, 11 (5), 231. https://doi.org/10.3390/educsci11050231
Talib, M. A., Bettayeb, A. M., & Omer, R. I. (2021). Analytical study on the impact of technology in higher education during the age of COVID-19: Systematic literature review. Education and Information Technologies, 26 (6), 6719–6746.
Tavitiyaman, P., Ren, L., & Fung, C. (2021). Hospitality students at the online classes during COVID-19–How personality affects experience? Journal of Hospitality, Leisure Sport & Tourism Education, 28 , 100304.
Toader, T., Safta, M., Titirișcă, C., & Firtescu, B. (2021). Effects of digitalisation on higher education in a sustainable development framework—Online learning challenges during the covid-19 pandemic. Sustainability, 13 (11), 6444. https://doi.org/10.3390/su13116444
Venkatesh, V., & Bala, H. (2008). Technology acceptance model 3 and a research agenda on interventions. Decision Sciences, 39 (2), 273–315.
Venkatesh, V., Thong, J. Y., & Xu, X. (2016). Unified theory of acceptance and use of technology: A synthesis and the road ahead. Journal of the Association for Information Systems, 17 (5), 328–376.
Watermeyer, R., Crick, T., Knight, C., & Goodall, J. (2021). COVID-19 and digital disruption in UK universities: Afflictions and affordances of emergency online migration. Higher Education, 81 (3), 623–641. https://doi.org/10.1007/s10734-020-00561-y
Yu, Z. (2021). The effects of gender, educational level, and personality on online learning outcomes during the COVID-19 pandemic: Revista de Universidad y Sociedad del Conocimiento. International Journal of Educational Technology in Higher Education . https://doi.org/10.1186/s41239-021-00252-3
Download references
Author information
Authors and affiliations.
School of Business and Management, Queen Mary University London, Mile End Rd, Bethnal Green, London, E1 4NS, UK
Institute for University to Business Education, Glasgow Caledonian University, Cowcaddens Rd, Glasgow, G4 0BA, UK
Christopher James MacBride Smith
School of Design, University of Leeds, Woodhouse, Leeds, LS2 9JT, UK
Hosam Al-Samarraie
You can also search for this author in PubMed Google Scholar
Corresponding author
Correspondence to Xue Zhou .
Ethics declarations
Conflict of interest.
The authors declare no conflicts of interest.
Ethical approval
The study did not involve human research participants.
Additional information
Publisher's note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (DOCX 31 KB)
Supplementary file2 (docx 19 kb), rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ .
Reprints and permissions
About this article
Zhou, X., Smith, C.J.M. & Al-Samarraie, H. Digital technology adaptation and initiatives: a systematic review of teaching and learning during COVID-19. J Comput High Educ (2023). https://doi.org/10.1007/s12528-023-09376-z
Download citation
Accepted : 11 April 2023
Published : 26 April 2023
DOI : https://doi.org/10.1007/s12528-023-09376-z
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Digital technology adaptation
- Higher education
- Student and staff experience
- Systematic literature review
- Online/blended learning
- Find a journal
- Publish with us
- Track your research
Free Samples and Examples of Essays, Homeworks and any Papers
- Absolutely free
- Perfect homeworks
- Fast relevant search
- No registration and Anonymous
Adapting to New Technology
Filed Under: Essays Tagged With: Technology
Since teachers know that new technology will mean a lot to students, they do not mind studying how to make the most of it. In many cases, public schools do not have the financial ability to provide new technology to students. Instead, they are stuck using the same old computers, software, and other hardware. Along with this, schools that are struggling financially also find it difficult to pay for system maintenance. There is no rule saying that computer programs are better teaching tools than traditional methods.
If you decide on new technology in your classroom, it is important to monitor students to determine if they are making expected progress. In other words, new technology should lead to a better learning environment and a more efficient classroom. Take this situation for example: when I was a junior high school student, there was a computer lab, shared by all students. At the time, though, we did not have access to new technology as it was yet to be invented. Of course, we were able to learn enough to see where things were headed in the near future.
Another method of adapting to new technology includes taking advantage of mostly advanced technology, including software and computers in all classrooms. This is much better than having a single computer lab for a large number of students to share. The main benefit is more time with the technology for each student, as well as a larger space for working. Students who are used to learning through more traditional means may have a difficult time adapting to new technology. For this reason, expectations for these students will be less than those for future students.
The Development Of A Prevention Dropout For Secondary Student In An Urban High School Setting
The Development of a Prevention Dropout for Secondary Student in an Urban High School Setting According to Noguera and Dimon (2003), the rate of dropout in American urban high schools may be the biggest but least known problem today. Noguera and Dimon estimated that at a great amount of schools 50% and even more of the students who start their ninth grade leave it without graduation. [3]. Many ...
In turn, schools are always challenged with an imbalance as they try to get all students on the same page. Fortunately, the cost of new technology is falling. This means that more schools, regardless of financial means, will be able to implement the latest technology. All schools should research the benefits of new technology, and then do what they can to implement these tools into every classroom. In order to adapt to new technology, we all have to require applying ourselves to fresh challenges. We must be a lifelong learner, because technology advances are inevitable and on-going. We cannot escape them.

Similar Papers
Computer addiction people time internet.
... schools' computer lab. Because it is free and most school provide an e-mail account and have no limit the amount of time for student ... persons that the internet supplies." Computer addiction is emerging. Since the computer technology has to bring new ...
The Lost Tools Of Education
... technology. While schools focus on advancing learning tools, the set back on students had remained hidden behind the walls of digital invasion. Before the computers, school ...
Computers In Classrooms Computer Students Student
... of technology in America's society today, the use of computers in school classrooms has increased tremendously-an action that certainly has become beneficial to students, ...
Using Technology to Motivate Students in the Science Classroom
... Technology to Motivate Students in the Science Classroom Today, a majority of students are either bored, frustrated, or feel like school is a waste of time. ... games versus the traditional lecture format (Greenemeier ... that can be adapted to different ...
Foundations In Education Students School Goals
... students are more diffuse, and academically talented groups. Unquestionably, the goals of education must be relevant to the times. If the schools cannot adapt ... for computer use, and higher-level cognitive skills for the world of work and technology. ...
Technology Students Learning Time
... -6868) Facilitating Collaborative Activity among Students Classrooms of networked computers using software such as Daedalus enable students to spend class time doing group pre-writing ...
- Skip to main content
- Skip to footer
- Explore More ASAE Sites
- ASAE Academy
- Associations Now
- Collaborate
- ASAE Research Foundation
- ASAE Business Solutions
- ASAE 401(k) Retirement Program
- Marketplace
Strategies to Help Staff Adapt to New Technology

Planning to shed your old technology for a hot new product or service? You’ll need to condition your staff to accept and adopt the upgrade. Here’s how to build an agile, multiphase training plan that targets their needs before and after implementation.
For nearly two years, Amy Williams was deeply involved in developing and executing an important communications plan for the American Society of Anesthesiologists. As its director of marketing and communications, Williams made sure that tailored messages were crafted and sent out at carefully chosen times to the many different stakeholders who were depending on ASA for information that would affect their professional lives.
What made this communications plan different from others that Williams had led was the fact that her primary stakeholders were all under ASA’s roof. Her mission: bring full transparency to staff as ASA implemented a new association management system that would affect nearly everyone in the organization.
By keeping staff apprised of every step of the transition, “we really eased their anxiety,” says Williams.
Get Staff on Board
If a full-blown communications plan like ASA’s seems like overkill for what some might see as an IT department project, think again: Major technology adoptions are no longer the sole province of IT. Rather, they are a critical component of an association’s strategic plan and have the potential to improve or even revolutionize what staff can accomplish. With all eyes on the endeavor and often a whole new platform to master, it’s no surprise that staff—particularly those who are less savvy with technology than their peers—may feel disconcerted. This is one reason why “communication on steroids” like Williams coordinated is essential, says Larry Wolff, president and COO of Ouellette & Associates, a consulting firm that specializes in the human side of technology.
The message to employees who will need to be trained in how to use the new system should be, “We’re going to escort you through the change,” Wolff says. Staff should also understand how the new technology will benefit them individually, he says. This creates the all-essential buy-in that can mitigate a chief roadblock to adoption and learning: resistance.
In the Ouellette & Associates book Leading IT Transformation, managers are cautioned that “depending on the severity of the change … people’s natural inclination is to protect themselves, preserve their competence, maintain their comfort zone.” By answering their unspoken question—“What’s in it for me?”—you enable them to start “emotionally accepting” the change, says Wolff.
In addition, today’s highly customizable technology products allow associations to give staff a say in how the new product is configured. Wolff says project leaders should interview people throughout the organization about how they work—ideally before the technology is even purchased—and then invite them to explore the new system and suggest tweaks or additions that will make their work more productive or efficient.
“It doesn’t matter if you have the best technology in the world if you don’t have the ability to align the solution with the actual needs of the end users,” he says.
Optimal Networks, a technology services firm, sought this alignment when the company was transitioning to the communication tool Slack. Founder and CEO Heinan Landa set up a committee of people from every part of the organization and asked them to come up with a capabilities wish list for the app. Then, he formed a pilot group of users, including several remote workers, who spent a month using it among themselves. The collective feedback contributed to a final product that is wildly popular throughout the organization, Landa says.
Genuine employee input not only will allow an association to roll out a more powerful product optimized for each department, but people will also be more enthusiastic about using the new system because they will feel like they were heard and matter to the organization.
Time to Train
Once the new technology tool is selected, whether it’s an AMS, a cloud-based platform like Office 365, or a collaboration tool like Slack, associations can choose from myriad methods and strategies to train staff. Learning products can be purchased online or through the product vendor; contracted for with an association management company, technology services firm, or professional training specialist; or even created in-house.
Just “don’t go into this thinking one size fits all,” says Frank Green, a learning specialist and senior director of global development with the technology services company Alphanumeric. More important, he cautions that training should not be an afterthought to product acquisition.
He knows what’s coming when decision makers say, “‘Let’s launch it and see what bugs there are and what questions we get—then we’ll train,’” Green says. “Now you’ve got something operational, with people continually calling the help desk and asking their friends what to do. This happens with surprising frequency,” even in large organizations, and it “costs money and morale.”
When you are ready to devise a training plan, you can build one that fits your organization’s size and budget and accommodates all kinds of learners.
Guided Learning
Traditional guided or instructor-led training tends to be an organization’s default plan. Most people with several decades on their resumes are probably familiar with the “OK, everyone in the conference room!” approach to training. But it’s easy to go wrong here.
Having an IT manager walk the entire staff through the system start to finish is “penny wise and pound foolish,” says Green. Scheduling several days of this hours-long training only tempts employees to think, “I’m going to be sick that week.” And, customer service staffers who are required to learn a new AMS but who will never need to run a segmented membership report, for example, may think, “I just wasted three hours of my life.”
The better approach: targeted instructor-led training by department role that homes in on what users need. “This is crucial for the successful launch of any application, upgrade, or standalone,” says Green.
During guided sessions, it’s also important to prioritize “fingers on the keyboard,” says Wolff: “For adults, 70 percent of learning is by actually doing.” Keep observation time to a few minutes, he says, and then have staff practice real-life functions the rest of the session.
Pacing can be a drawback to guided training, particularly for staff who don’t grasp technology-related instruction as quickly as others do. Mentoring, including cross-generational pairing, can work well by allowing the more uncertain staff member to set the pace and feel more comfortable asking for a step to be repeated.
Other productive ways to provide guided training include:
- Lunch and learns. Short, low-key sessions can impart bite-size chunks of knowledge that won’t overwhelm. This is also a good format to compare how functions in the old and new systems work. Bonus: Not only do staff learn the system, but they also help IT catch anything they might have missed, allowing the tech team to adjust while still in the conversion process.
- Champions. During deployment, Wolff suggests enlisting champions or “superusers” to walk around for a day or two, physically or virtually, to guide employees through something they may have missed or forgotten. Champions can also help executives and staff with heavy travel schedules who may not be able to attend training classes by teaching them the essentials for their job in an hour or two and then referring them to microlearning tools.
- War room. After bringing in experts to do intense training segmented by department and functions, ASA stationed an employee and a projector in “a war room, if you will,” says Williams, for four hours a day, twice a week, for several weeks leading up to the conversion and for a time afterward. Employees were welcome to drop in and get whatever individualized help they needed.
Solo Learning
Wolff has also found that when training people on new technology, many “will be pretty self-sufficient” and not need much face-to-face instruction. This is especially true among millennials and Gen X staff. Factored in with time and budget constraints, this has led to more self-guided learning methods, including these:
- Playgrounds. Create a development site, as ASA did six months before launch, where employees can safely practice using the system’s features without fear of “messing up the whole database” (a common worry). This is a valuable learning tool for users like Williams, who prefers to dive in and play around to better grasp what she’s read.
- Self-service knowledge base for microlearning tools. Microlearning lets users pick up complicated software functions in manageable portions at their own pace based on when they need the help. Tools can be housed together on the network and can range from purchased lessons and videos to low-tech infographics and cheat sheets.
- Videos. Even a cash-strapped communications or IT shop with just a few staff can tap into the power of video by taking screenshots of step-by-step instructions, or filming a user demonstrating a task, and then posting the video clip to YouTube or the association’s network. As with other microlearning elements, shorter equals better.
By ensuring that all staff members know how they will benefit from the new system, receive clear communication on when and how it will be implemented, and get practical training that meets their specific needs, associations are likely to end up with a success story like Williams experienced at ATA.
Being transparent and supportive “really created camaraderie among staff,” Williams says. “The messages of ‘We’re in this together’ worked.”
[This article was originally published in the Associations Now print edition, titled “Training Camp.”]
IT Strategy & Management
Change management, employee training, maria mihalik.
Maria Mihalik is newsletter and supplements editor of Associations Now in Washington, DC.
Read These Next
- {{article.Title}}
- Back to main content
- Back to header
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
The PMC website is updating on October 15, 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- Int J Environ Res Public Health

Digital Transformation in Healthcare: Technology Acceptance and Its Applications
Angelos i. stoumpos.
1 Healthcare Management Postgraduate Program, Open University Cyprus, P.O. Box 12794, Nicosia 2252, Cyprus
Fotis Kitsios
2 Department of Applied Informatics, University of Macedonia, 156 Egnatia Street, GR54636 Thessaloniki, Greece
Michael A. Talias
Associated data.
Not applicable.
Technological innovation has become an integral aspect of our daily life, such as wearable and information technology, virtual reality and the Internet of Things which have contributed to transforming healthcare business and operations. Patients will now have a broader range and more mindful healthcare choices and experience a new era of healthcare with a patient-centric culture. Digital transformation determines personal and institutional health care. This paper aims to analyse the changes taking place in the field of healthcare due to digital transformation. For this purpose, a systematic bibliographic review is performed, utilising Scopus, Science Direct and PubMed databases from 2008 to 2021. Our methodology is based on the approach by Wester and Watson, which classify the related articles based on a concept-centric method and an ad hoc classification system which identify the categories used to describe areas of literature. The search was made during August 2022 and identified 5847 papers, of which 321 fulfilled the inclusion criteria for further process. Finally, by removing and adding additional studies, we ended with 287 articles grouped into five themes: information technology in health, the educational impact of e-health, the acceptance of e-health, telemedicine and security issues.
1. Introduction
Digital transformation refers to the digital technology changes used to benefit society and the healthcare industry. Healthcare systems need to use digital technology for innovative solutions to improve healthcare delivery and to achieve improvement in medical problems. The digital transformation of healthcare includes changes related to the internet, digital technologies, and their relation to new therapies and best practices for better health management procedures. The quality control of massive data collected can help improve patients’ well-being and reduce the cost of services. Digital technologies will also impact medical education, and experts will deceive new ways to train people. Now in this way, practitioners will face new opportunities.
Digital transformation is an ongoing process that can create opportunities in the health sector, provided the necessary infrastructure and training are available. Under Regulation (EU) 2021/694 of the European Parliament and of the Council of 29 April 2021, establishing the Digital Europe Program and repealing Decision (EU) 2015/2240, digital transformation is defined as the use of digital technologies for the transformation of businesses and services. Some technologies that contribute to digital transformation are the digital platform of the Internet of Things, cloud computing and artificial intelligence. At the same time, the sectors of society that are almost affected are telecommunications, financial services and healthcare.
Digital health can play a role in innovation in health, as it facilitates the participation of patients in the process of providing health care [ 1 ]. The patient can overcome his poor state of health when they are no longer in a state of well-being. In this case, the patient is given the to participate in the decision-making regarding their health care. Searching for information through the patient’s internet or using digital health applications (e.g., via mobile phone) is essential for the patient to make the right decision about their health.
In the coming years, health change is expected to focus primarily on the patient, who will take on the “health service consumer” role as the patient seeks control over their health management. The healthcare industry will be shaped based on the needs and expectations of this new “consumer of health services”, which will require upgraded experiences with the main characteristics of personalisation, comfort, speed and immediacy in the provision of services. Gjellebaek C. et al. argue that new digital technologies will shift healthcare towards digitalisation, bringing significant benefits to patients and healthcare infrastructure [ 2 ]. Some of the benefits listed by Gjellebaek C. are the increase in employee productivity, the improvement of the efficiency and effectiveness of the operation of the health units, and the reduction of their operating costs.
On the other hand, in terms of health infrastructure, a typical example is the United States, where 75% of hospitals use electronic health record systems, according to Rebekah E. et al. [ 3 ]. However, clinicians often report side effects using digital technologies, which can be attributed to their misuse [ 3 ]. In addition, some health professionals oppose using these systems and develop solutions that jeopardise patient care. In some countries, such as the United States, the government provides incentives for the “effective use” of e-health technologies, but their results remain uncertain [ 3 ].
Rebekah E. et al. focus more specifically on U.S. hospitals, observing that the remaining countries are relatively in the early stages of transformation [ 4 ]. The United Kingdom, for example, has recently pursued troubled e-health initiatives, and Australian hospitals have only recently participated in investments in the digitalisation of their hospital services [ 4 ]. At the European Union level, digital health is a critical key strategic priority, in line with the European Strategic Plan 2019–2024 (European Commission).
Today, digital transformation in health is spreading and consolidating rapidly [ 5 ]. The purpose of this paper is to provide an assessment of the current literature on digital health transformation, as well as to identify potential vulnerabilities that make its implementation impossible. The ultimate goal is to see how digital technologies facilitate patients’ participation in health and their health.
Due to the rapid development of e-health and digitalisation, data from previous studies are becoming potentially irrelevant. Most studies evaluating digitalisation have relied heavily on quantitative research-based methods. Although quantitative evaluations are required, some of their effects could be omitted.
According to Gopal G. et al., healthcare has the lowest level of digital innovation compared to other industries, such as media, finance, insurance and retail, contributing to limited labour productivity growth [ 6 ]. With this article, we seek to reverse this picture and contribute to the emergence of digitalisation as a factor of health innovation while optimising patient outcomes and the cost of services provided. However, to achieve this innovation, systemic changes are needed in healthcare finances, the education of healthcare staff and healthcare infrastructure.
The following section analyses the methodology and its steps, which then contributed to the emergence of our results.
2. Material and Methods
2.1. search strategy and bibliography reviews.
Our research approach is based on the methodology of Webster and Watson, who developed a concept-centric method and an ad hoc classification system in which categories are used to describe areas of literature [ 7 ]. Initially, the existing bibliographic reviews were searched to select the databases based on keywords. A retrospective search was then performed to examine the reports of the selected works. Finally, the references of selected works were investigated to increase the search sample through the future search. After selecting the articles, they were grouped according to their content.
Systematic reviews were conducted to place this paper on existing knowledge of digital health, as well as to review prior knowledge in this area and to discuss recognised research questions based on the results of previous studies. A comprehensive review of the published literature was reported by Marques, I. C., & Ferreira, J. J. [ 8 ]. The authors explored the potential of existing digital solutions to improve healthcare quality and analysed the emerging trend in digital medicine to evaluate the research question of how stakeholders apply and manage digital technologies for business purposes [ 9 ]. The main question is: How and what could be done sustainably and inclusively through innovation to achieve sustainable development goals by taking advantage of Information and Communication Technologies? Recently, researchers have expressed concern about secure communication and user authentication within providing information to patients. In contrast with data storage, information exchange, and system integration, new approaches and uses of patient care processes are envisaged with the prospect of monitoring not only diagnostic statistics but also in-depth analysis of signs and symptoms before and after treatment, essential sources for new research. Table 1 presents the previous bibliographic reviews on which our study was based.
Previous Bibliographic Reviews.
| Reference | Keywords | Methodology | Results | |
|---|---|---|---|---|
| 1. | Kraus, S., et al., Digital transformation in healthcare: Analyzing the current state-of-research [ ] | Digital* AND healthcare | 2 Databases (EBSCO)—130 articles (ELSEVIER Science Direct and Springer Link)—340 articles | The article assesses how multiple stakeholders implement digital technologies for management and business purposes. |
| 2. | Marques, Isabel C.P. and Ferreira, Joao J.M. Digital transformation in the area of health: a systematic review of 45 years of evolution. Health and Technology. 2020, 10, pp. 575–586. [ ] | Digital AND Health AND Information System AND Management AND Hospital | 1 Database (Scopus)—749 articles | Explore the potential of existing digital solutions to improve the quality and safety of healthcare and analyse the emerging trend of digital medicine. |
| 3. | Kolasa, K. and G. Kozinski, How to Value Digital Health Interventions? A Systematic Literature Review [ ] | Mhealth Mobile health Telemedicine Health app Wearables | 3 Databases (Pubmed, Scopus and Science Direct)—34 articles | It proposed five recommendations for the generation of evidence to be considered in developing digital health solutions and suggestions for adopting the methodological approach in DHIs’ pricing and reimbursement. |
| 4. | Mehdi Hosseinzadeh, Omed Hassan Ahmed, Ali Ehsani, Aram Mahmood Ahmed, Hawkar kamaran Hama. The impact of knowledge on e-health: a systematic literature review of the advanced systems [ ] | Knowledge health Knowledge e-health | 6 Databases (Google Scholar, Public Libraries, Science Direct, Springer Link, Web of Science and IEEE Xplore)—132 articles | Knowledge is considered one of the important research directions for many purposes in e-health. |
| 5. | Shah Nazir, Yasir Ali, Naeem Ullah and Ivan Garcia—Magarino. Internet of Things for Healthcare Using Effects of Mobile Computing: A Systematic Literature Review, Hindawi, Wireless Communications and Mobile Computing, Volume 2019. [ ] | (Internet of things OR IoT) AND (Smart hospitals) AND (Healthcare) AND (Mobile Computing) OR “Internet of things OR IoT” and “Smart hospitals” and “healthcare” and Mobile computing.” | 5 Databases (Science Direct, Springer, IEEE, Taylor and Francis, Hindawi)—116 articles | Mobile computing extends the functionality of IoT in the healthcare environment by bringing massive support in the form of mobile health (m-health). In this research, a systematic literature review protocol is proposed to study how mobile computing assists IoT applications in healthcare, contributes to the current and future research of IoT in the healthcare system, brings privacy and security to health IoT devices, and affects the IoT in the healthcare system. Furthermore, the paper intends to study the impacts of mobile computing on IoT in the healthcare environment or intelligent hospitals. |
| 6. | Chiranjeev Sanyal, Paul Stolee, Don Husereau. Economic evaluations of eHealth technologies: A systematic review, PLoS ONE [ ] | Assistive technology Socially assistive robots Mobile health Mobile robot Smart home system Telecare Telehealth Telemedicine Wander prevention systems Mobile locator devices Gps Location-based technology Mobile apps Mobile application Cell phone Web-based Internet M-health M-health eHealth e-health older adult elderly seniors older patient cost-effective cost-utility economic evaluation | 5 Databases (MEDLINE, EMBASE, CINAHL, NHS EED, and PsycINFO)—14 articles | E-health technologies can be used to provide resource-efficient patient-oriented care. This review identified the growing use of these technologies in managing chronic diseases in study populations, including older adults. |
| 7. | Kampmeijer, R., et al., The use of e-health and m-health tools in health promotion and primary prevention among older adults: a systematic literature review. [ ] | (“aged”[MeSH Terms] OR “aged”[All Fields] OR “elderly”[All Fields] OR “old”[All Fields] OR “senior”[All Fields] OR “seniors”[All Fields]) AND (“health promotion”[MeSH Terms] OR “health promotion”[All Fields] OR “promotion”[All Fields] OR “primary prevention”[MeSH Terms] OR “primary prevention”[All Fields] OR “prevention”[All Fields]) AND (“telemedicine”[MeSH Terms] OR “telemedicine”[All Fields] OR “telemedicine”[All Fields] OR “telehealth”[All Fields] OR “telehealth”[All Fields] OR “m-health”[All Fields] OR “m-health”[All Fields] OR “e-health”[All Fields] OR “e-health”[All Fields]) | 1 Database (PubMed)—45 articles | E-health and m-health tools are used by older adults in diverse health promotion programmes but also outside formal programmes to monitor and improve their health. |
| 8. | Iyawa, G.E., M. Herselman, and A. Botha, Digital health innovation ecosystems: From a systematic literature review to conceptual framework [ ] | Digital health Innovation Digital ecosystems | 4 Databases (ACM, Science Direct, IEEE Xplore and SpringerLink)—65 articles | The study identified components of digital health, components creation relevant to the healthcare domain, and components of digital ecosystems. |
| 9. | Gagnon, M.-P., et al., m-Health adoption by healthcare professionals: a systematic review. [ ] | m-Health healthcare professionals and adoption | 4 Databases (PubMed, Embase, Cinhal, PsychInfo)—33 articles | The Main perceived adoption factors to m-health at the individual, organisational, and contextual levels were the following: perceived usefulness and ease of use, design and technical concerns, cost, time, privacy and security issues, familiarity with the technology, risk-benefit assessment, and interaction with others (colleagues, patients, and management). |
| 10. | Leslie W., Kim, A. and D. Szeto, The evidence for the economic value of ehealth in the united states today: a systematic review. J Int Soc Telemed EHealth, 2016. [ ] | (telemedicine OR “Mobile Health” OR “Health, Mobile” OR mHealth OR mHealths OR Telehealth OR eHealth) AND (“Cost-Benefit Analysis” OR “Analyses, Cost-Benefit” OR “Analysis, Cost-Benefit” OR “Cost-Benefit Analyses” OR “Cost Benefit Analysis” OR “Analyses, Cost Benefit” OR “Analysis, Cost Benefit” OR “Cost Benefit Analyses” OR “Cost Effectiveness” OR “Effectiveness, Cost” OR “Cost-Benefit Data” OR “Cost Benefit Data” OR “Data, Cost-Benefit” OR “Cost-Utility Analysis” OR “Analyses, Cost-Utility” OR “Analysis, Cost-Utility” OR “Cost Utility Analysis” OR “Cost-Utility Analyses” OR “Economic Evaluation” OR “Economic Evaluations” OR “Evaluation, Economic” OR “Evaluations, Economic” OR “Marginal Analysis” OR “Analyses, Marginal” OR “Analysis, Marginal” OR “Marginal Analyses” OR “Cost Benefit” OR “Costs and Benefits” OR “Benefits and Costs” OR “CostEffectiveness Analysis” OR “Analysis, CostEffectiveness” OR “Cost-Effectiveness Analysis”) Virtual healthcare | 2 Databases (PubMed and The Cochrane Library) -20 articles | The goal of this study is to evaluate the published economic evidence for e-health in the United States, analyse how well it supports the growth of the current e-health environment, and suggest what evidence is needed. |
| 11. | Hu, Y. and G. Bai, A Systematic Literature Review of Cloud Computing in Ehealth. Health Informatics—[ ] | (Cloud) AND (eHealth OR “electronic health” OR e-health) | 5 Databases (ACM Digital Library, IEEE Xplore, Inspec, ISI Web of Science and Springer)—44 articles | With the unique superiority of the cloud in big data storage and processing ability, a hybrid cloud platform with mixed access control and security protection mechanisms will be the main research area for developing a citizen-centred home-based healthcare system. |
| 12. | Boonstra, A., A. Versluis, and J.F.J. Vos, Implementing electronic health records in hospitals: a systematic literature review. BMC Health Services Research, 2014. 14(1): p. 370. [ ] | “Electronic Health Record*” + implement* + hospital* “Electronic Health Record*” + implement* + “healthcare” “Electronic Health Record*” + implement* + clinic* “Electronic Patient Record*” + implment* + hospital* “Electronic Patient Record*” + implement* + “healthcare” “Electronic Patient Record*” + implement* + clinic* “Electronic Medical Record*” + implement* + hospital* “Electronic Medical Record*” + implement* + “healthcare” “Electronic Medical Record*” + implement* + clinic* “Computeri?ed Patient Record*” + implement* + hospital* “Computeri?ed Patient Record*” + implement* + “health care” “Computeri?ed Patient Record*” + implement* + clinic* “Electronic Health Care Record*” + implement* + hospital* “Electronic Health Care Record*” + implement* + “health care” “Electronic Health Care Record*” + implement* + clinic* “Computeri?ed Physician Order Entry” + implement* + hospital* “Computeri?ed Physician Order Entry” + implement* + “health care” “Computeri?ed Physician Order Entry” + implement* + clinic* | 3 Databases (Web of Knowledge, EBSCO and the Cochrane Library)—21 articles | Although EHR systems are anticipated to affect hospitals’ performance positively, their implementation is complex. |
| 13. | Pagliari, C., et al., What Is eHealth (4): A Scoping Exercise to Map the Field. J Med Internet Res, 2005. 7(1) [ ] | “Ehealth OR e-health OR e*health” | 8 Databases (Medline [PubMed], the Cumulative Index of Nursing and Allied Health Literature [CINAHL], the Science Citation Index [SCI], the Social Science Citation Index [SSCI], the Cochrane Library Database (including Dare, Central, NHS Economic Evaluation Database [NHS EED], Health Technology Assessment [HTA] database, NHS EED bibliographic) and Index to Scientific and Technical Proceedings (ISTP, now known as ISI Proceedings)—387 articles | Definitions of e-health vary concerning the functions, stakeholders, contexts, and theoretical issues targeted. |
2.2. Network Analysis
Network analysis is considered a branch of graph theory. Our network analysis is based on the similarity of keywords found in identifying the eligible papers. We used visualisation of similarities (VOS) software, version 1.6.18, to construct graphical networks to understand the clustering of the keywords and their degree of dissimilarity. Our network analysis is based on the similarity of keywords found in identifying the eligible papers.
Initial Search
The search was performed on the following databases: Scopus, Science Direct, and PubMed, using the keywords “digital transformation”, “digitalisation”, “Ehealth or e-health”, “mhealth or m-health”, “healthcare” and “health economics”. We selected publications from the search of international journals and conference proceedings. We collected papers from 2008 until 2021. The documents sought belonged to strategy, management, computer science, medicine, and health professions. Finally, the published works were in English only. The total number of articles collected using the keywords as shown in Table 2 was 5847.
Search Strategy.
| Database | Search within | Keywords | No Sources | |
|---|---|---|---|---|
| 1. | Scopus | Article title, Abstract, Keywords | (Digital transformation or digitalization) AND (Ehealth or e-health or mhealth or m-health or healthcare) AND (health economics) | 408 |
| Article title, Abstract, Keywords | (Digital transformation) AND (health) | 1.152 | ||
| 2. | Science Direct | Article title | (Digital transformation) AND (health) | 2.142 |
| 3. | PubMed | Article title, Abstract | (Digital transformation or digitalization) AND (Ehealth or e-health or mhealth or m-health or healthcare) AND (health economics) | 978 |
| Article title | (Digital transformation) AND (health) | 1.167 | ||
| Total | 5.847 | |||
We systematically checked the total number of papers 5847 by reading their titles, abstracts, and, whenever necessary, the article’s first page to conclude if each document was relevant as a first step as shown in the Figure 1 .

The diagram for the first phase of the selection process.
Then, we looked at the titles of the 378 articles, and after reading their summary, we accepted 321 articles. Further studies were rejected because their full text was not accessible. As a result, there were 255 articles in our last search. Of the selected 255 articles, 32 more were added based on backward and forward research. The investigation was completed by collecting common standards from all databases using different keyword combinations. According to the systematic literature review, we follow the standards of Webster and Watson (2002) to reject an article. Since then, we have collected the critical mass of the relevant publications, as shown in Figure 2 .

The diagram of the article selection process.
3.1. Chronological Development of the Publications
The categorisation of the articles was based on their content and the concepts discussed within them. As a result, we classify articles into the following categories: information technology in health, the educational impact on e-health, the acceptance of e-health, telemedicine, and e-health security.
Although researchers in Information and Communication Technology and digitalisation conducted studies almost two decades ago, most publications have been published in the last eight years. This exciting finding highlights the importance of this field and its continuous development. Figure 3 shows a clear upward trend in recent years. More specifically, the research field of Information and Communication Technology, in combination with digital transformation, appeared in 2008. However, the most significant number of articles was found in 2019, 2020 and 2021. The number of articles decreased to the lowest in 2009–2011 and 2013–2014. Due to the expansion of the field to new technologies, the researchers studied whether the existing technological solutions are sufficient for implementing digital transformation and what problems they may face.

Number of articles and citations per publication by year.
Figure 3 shows a combination of the articles per year and the number of citations per publication per year.
3.2. Document Type
Of the document types, 59.51 per cent of the articles were categorised as “survey”, while a smaller percentage were in: “case study” (32.53%), “literature review” (5.88%) and “report” (2.08%). However, these documents focused on specific concepts: “information technology in health” (45%), “education impact of e-health” (11%), “acceptance of e-health” (19%), “telemedicine” (7%), “security of e-health” (18%).
As we can see from the following Figure 4 , we used network analysis, where the keywords related to digitalisation and digital transformation were identified in the research study. Network analysis, using keywords, came with VOSviewer software to find more breadth and information on healthcare digitalisation and transformation exploration. It was created by analysing the coexistence of keywords author and index. This analysis’s importance lies in the structure of the specific research field is highlighted. In addition, it helped map the intellectual structure of scientific literature. Keywords were obtained from the title and summary of a document. However, there was a limit to the number of individual words. The figure represents a grid focused on reproducing keywords in the literature on the general dimensions of digitalisation. The digitalisation network analysis showed that e-health, telemedicine, telehealth, mobile health, electronic health/medical record, and information systems were the main relevant backgrounds in the literature we perceived. In the healthcare literature, keywords such as “empowerment” and “multicenter study” usually do not lead to a bibliographic search on digitalisation. Figure 4 shows how e-health and telemedicine have gone beyond the essential and most crucial research framework on how they can affect hospitals and the health sector. The potentially small gaps in network analysis can be filled by utilising data in our research study, contributing to future research.

Bibliometric map of the digital transformation and healthcare.
Figure 5 shows the network analysis with the keywords concerning time publication. The yellow colour indicates keywords for most recent years.

Network visualisation of keywords per year.
Figure 6 presents the density visualisation of keywords.

Heat map of keywords.
Figure 7 shows the number of articles per each method (survey, literature review etc.) for each year.

The map of number of articles per method for each year.
It is evident from Figure 7 that the most used method paper is the survey type and that in the year 2021, we have a high number of surveys compared to previous years.
3.3. Summary of the Included Articles
In Figure 2 , we have explained how we collected the critical mass of the 255 relevant publications. We added another 32 articles based on further research with the backward and research methods, which resulted in a total number of 287 articles.
Then, the articles were categorised according to their content. The concepts discussed in the papers are related to information technology in health, the educational impact of e-health, the acceptance of e-health, telemedicine, and e-health security. For this purpose, the following table was created, called the concept matrix table.
4. Concept Matrix
In this section, we provide the Concept matrix table. Academic resources are classified according to if each article belongs or not to any of the five concepts shown in Table 3 .
Concept Matrix Table.
| No. | Author | Year | Method | Sample | Data Analysis | Concepts | ||||
|---|---|---|---|---|---|---|---|---|---|---|
| Information Technology in Health | Education Impact of E-Health | Acceptance of E-Health | Telemedicine | Security of E-Health | ||||||
| 1 | Kesavadev, J, et al., [ ] | 2021 | Case Study | Χ | ||||||
| 2 | Attila, SZ et al., [ ] | 2021 | Survey | Χ | ||||||
| 3 | Malachynska, M et al., [ ] | 2021 | Case Study | Χ | ||||||
| 4 | Lu, WC et al., [ ] | 2021 | Survey | Χ | ||||||
| 5 | Burmann, A et al., [ ] | 2021 | Case Study | Χ | ||||||
| 6 | Bogumil-Ucan, S et al., [ ] | 2021 | Case Study | Χ | ||||||
| 7 | Zanutto, O [ ] | 2021 | Survey | Χ | ||||||
| 8 | Alauddin, MS; et al., [ ] | 2021 | Survey | Χ | ||||||
| 9 | Alterazi, HA [ ] | 2021 | Survey | Χ | ||||||
| 10 | Schmidt-Kaehler, S et al., [ ] | 2021 | Case Study | Χ | ||||||
| 11 | Zhao, Y et al., [ ] | 2021 | Case Study | Χ | Χ | |||||
| 12 | Roth, CB et al., [ ] | 2021 | Systematic Literature Review | Χ | Χ | |||||
| 13 | Ali, NA et al., [ ] | 2021 | Case Study | Χ | ||||||
| 14 | Alimbaev, A et al., [ ] | 2021 | Case Study | Χ | ||||||
| 15 | Dick, H et al., [ ] | 2021 | Systematic Literature Review | Χ | Χ | |||||
| 16 | Alt, R et al., [ ] | 2021 | Survey | a Vice President | - | Χ | ||||
| 17 | Bartosiewicz, A et al., [ ] | 2021 | Survey | Χ | Χ | |||||
| 18 | Mussener, U [ ] | 2021 | Survey | Χ | ||||||
| 19 | Naumann, L et al., [ ] | 2021 | Case Study | 59 qualitative telephone interviews | The findings hinted at five priorities of e-health policy making: strategy, consensus-building, decision-making, implementation and evaluation that emerged from the stakeholders’ perception of the e-health policy. | Χ | ||||
| 20 | Saetra, HS et al., [ ] | 2021 | Case Study | Χ | ||||||
| 21 | Zoltan, V et al., [ ] | 2021 | Survey | Χ | Χ | |||||
| 22 | Hoch, P et al., [ ] | 2021 | Survey | Χ | ||||||
| 23 | De Vos, J [ ] | 2021 | Survey | Χ | ||||||
| 24 | Beaulieu, M et al., [ ] | 2021 | Survey | Χ | ||||||
| 25 | Dang, TH et al., [ ] | 2021 | Survey | Χ | Χ | Χ | ||||
| 26 | Kraus, S et al., [ ] | 2021 | Systematic Literature Review | Χ | Χ | Χ | ||||
| 27 | Gauthier, P et al., [ ] | 2021 | Survey | Χ | ||||||
| 28 | Zhang, JS et al., [ ] | 2021 | Survey | Χ | ||||||
| 29 | Mallmann, CA et al., [ ] | 2021 | Survey | 513 breast cancer patients from 2012 to 2020 | Statistical analysis | Χ | ||||
| 30 | Fons, AQ [ ] | 2021 | Survey | Χ | ||||||
| 31 | Chatterjee, S et al., [ ] | 2021 | Survey | Consumers of different age groups & people working in the healthcare sector (including doctors) | Qualitative analysis | Χ | Χ | |||
| 32 | Wasmann, JWA et al., [ ] | 2021 | Survey | Χ | ||||||
| 33 | Kanungo, RP et al., [ ] | 2021 | Survey | Χ | ||||||
| 34 | Fernandez-Luque, L et al., [ ] | 2021 | Survey | Χ | ||||||
| 35 | Wilson, A et al., [ ] | 2021 | Survey | Χ | ||||||
| 36 | Ziadlou, D [ ] | 2021 | Survey | US health care leaders | Qualitative analysis | Χ | Χ | |||
| 37 | Oh, SS et al., [ ] | 2021 | Survey | Χ | Χ | |||||
| 38 | Knitza, J et al., [ ] | 2021 | Survey | Χ | ||||||
| 39 | Sergi, D et al., [ ] | 2021 | Survey | Χ | ||||||
| 40 | Rosalia, RA et al., [ ] | 2021 | Case Study | Χ | ||||||
| 41 | [Anonymous] [ ] | 2021 | Survey | Χ | ||||||
| 42 | Prisyazhnaya, NV et al., [ ] | 2021 | Survey | Χ | ||||||
| 43 | Odone, A et al. [ ] | 2021 | Case Study | Variety of participants | Qualitative and quantitative analysis | Χ | ||||
| 44 | Balta, M et al., [ ] | 2021 | Case Study | Χ | Χ | |||||
| 45 | Mues, S et al., [ ] | 2021 | Survey | Χ | ||||||
| 46 | Frick, NRJ et al., [ ] | 2021 | Case Study | Physicians (nine female and seven male experts) | Thematic analysis | Χ | ||||
| 47 | Dendere, R et al., [ ] | 2021 | Survey | Χ | ||||||
| 48 | Neumann, M et al., [ ] | 2021 | Survey | The dean or the most senior academic individual responsible for the medical curriculum development | Descriptive statistics in Microsoft Excel (Version 16.38) | Χ | ||||
| 49 | Su, Y et al., [ ] | 2021 | Case Study | Χ | ||||||
| 50 | Masuda, Y et al., [ ] | 2021 | Survey | Χ | ||||||
| 51 | Frennert, S [ ] | 2021 | Survey | Χ | Χ | |||||
| 52 | Hasselgren, A et al., [ ] | 2021 | Survey | Χ | Χ | |||||
| 53 | Kim, HK et al., [ ] | 2021 | Survey | Χ | Χ | |||||
| 54 | Marchant, G et al., [ ] | 2021 | Survey | 569 adults | Statistical analysis | Χ | ||||
| 55 | Malfatti, G et al., [ ] | 2021 | Survey | Χ | ||||||
| 56 | Krasuska, M et al., [ ] | 2021 | Case Study | 628 interviews, observed 190 meetings and analysed 499 documents | Thematical analysis | Χ | ||||
| 57 | Piccialli, F et al., [ ] | 2021 | Survey | Χ | ||||||
| 58 | Kyllingstad, N et al., [ ] | 2021 | Survey | Χ | ||||||
| 59 | Frasquilho, D et al., [ ] | 2021 | Case Study | Χ | ||||||
| 60 | Leone, D et al., [ ] | 2021 | Case Study | Χ | ||||||
| 61 | Kwon, IWG et al., [ ] | 2021 | Report | Χ | ||||||
| 62 | Sim, SS et al., [ ] | 2021 | Systematic Literature Review | Χ | ||||||
| 63 | Christie, HL et al., [ ] | 2021 | Case Study | Experts (n = 483) in the fields of e-health, dementia, and caregiving were contacted via email | Qualitative analysis | Χ | ||||
| 64 | Eberle, C et al., [ ] | 2021 | Survey | 2887 patients | Qualitative analysis | Χ | ||||
| 65 | Popkova, EG et al., [ ] | 2021 | Survey | Χ | ||||||
| 66 | Reich, C et al., [ ] | 2021 | Survey | Χ | ||||||
| 67 | Hanrieder, T et al., [ ] | 2021 | Survey | Χ | ||||||
| 68 | Aleksashina, AA et al., [ ] | 2021 | Survey | Χ | Χ | |||||
| 69 | Haase, CB et al., [ ] | 2021 | Survey | Χ | ||||||
| 70 | Mishra, A et al., [ ] | 2021 | Survey | Χ | ||||||
| 71 | Kokshagina, O [ ] | 2021 | Survey | Χ | ||||||
| 72 | Loch, T et al., [ ] | 2021 | Survey | Χ | ||||||
| 73 | Cajander, A et al., [ ] | 2021 | Survey | 17 interviews with nurses ( = 9) and physicians ( = 8) | Thematical analysis | Χ | Χ | |||
| 74 | Botrugno, C [ ] | 2021 | Survey | Χ | ||||||
| 75 | Jacquemard, T et al., [ ] | 2021 | Survey | Χ | ||||||
| 76 | Behnke, M et al., [ ] | 2021 | Survey | Χ | ||||||
| 77 | Peltoniemi, T et al., [ ] | 2021 | Case Study | Χ | ||||||
| 78 | Glock, H et al., [ ] | 2021 | Survey | Χ | ||||||
| 79 | Weitzel, EC et al., [ ] | 2021 | Survey | Χ | ||||||
| 80 | Sullivan, C et al., [ ] | 2021 | Case Study | Χ | ||||||
| 81 | Luca, MM et al., [ ] | 2021 | Survey | Χ | ||||||
| 82 | Negro-Calduch, E et al., [ ] | 2021 | Systematic Literature Review | Χ | ||||||
| 83 | Werutsky, G et al.,Denninghoff, V et al., [ ] | 2021 | Survey | Χ | ||||||
| 84 | Piasecki, J et al., [ ] | 2021 | Survey | Χ | Χ | |||||
| 85 | Broenneke, JB et al., [ ] | 2021 | Survey | Χ | ||||||
| 86 | Faure, S et al., [ ] | 2021 | Survey | Χ | ||||||
| 87 | Ghaleb, EAA et al., [ ] | 2021 | Survey | Χ | Χ | |||||
| 88 | Verket, M et al., [ ] | 2021 | Survey | Χ | ||||||
| 89 | Lenz, S [ ] | 2021 | Survey | 15 interviews with persons from different areas of digital health care | Theoretical sampling | Χ | ||||
| 90 | De Sutter, E et al., [ ] | 2021 | Survey | 31 healthcare professionals active | Qualitative analysis | Χ | ||||
| 91 | Gevko, V et al., [ ] | 2021 | Survey | Χ | ||||||
| 92 | El Majdoubi, D et al., [ ] | 2021 | Survey | Χ | ||||||
| 93 | Thakur, A et al., [ ] | 2021 | Case Study | Χ | ||||||
| 94 | Persson, J et al., [ ] | 2021 | Survey | Χ | ||||||
| 95 | Zippel-Schultz, B et al., [ ] | 2021 | Survey | 49 patients and 33 of their informal caregivers. | Qualitative analysis | Χ | ||||
| 96 | Lam, K et al., [ ] | 2021 | Survey | Χ | ||||||
| 97 | Manzeschke, A [ ] | 2021 | Survey | Χ | ||||||
| 98 | Dyda, A et al., [ ] | 2021 | Case Study | Χ | Χ | |||||
| 99 | Beckmann, M et al., [ ] | 2021 | Case Study | Variety of participants | Qualitative and quantitative analysis | Χ | ||||
| 100 | Numair, T et al., [ ] | 2021 | Survey | Kenya: Interviewees included nurses, community health workers, and operators hired exclusively for data entry in the WIRE system. Laos: As no operators were hired in Lao PDR, interviewees included nurses, doctors, and midwives who used the WIRE system daily. (20 healthcare workers in Kenya & Laos PDR) | Qualitative and quantitative analysis | Χ | ||||
| 101 | Xiroudaki, S et al., [ ] | 2021 | Case Study | Χ | ||||||
| 102 | Droste, W et al., [ ] | 2021 | Survey | Χ | ||||||
| 103 | Lee, JY et al., [ ] | 2021 | Systematic Literature Review | Χ | ||||||
| 104 | Giovagnoli, et al., [ ] | 2021 | Survey | Χ | ||||||
| 105 | Daguenet, et al., [ ] | 2021 | Survey | Χ | ||||||
| 106 | Hubmann, et al., [ ] | 2021 | Survey | Χ | ||||||
| 107 | Vikhrov, et al., [ ] | 2021 | Survey | Χ | ||||||
| 108 | Jahn, HK et al., [ ] | 2021 | Survey | 198 complete and 45 incomplete survey responses from physicians | Statistical analysis | Χ | ||||
| 109 | Low et al., [ ] | 2021 | Survey | Χ | ||||||
| 110 | Levasluoto, et al., [ ] | 2021 | Case Study | 23 interviews | Thematical analysis | Χ | ||||
| 111 | Verma, et al., [ ] | 2021 | Survey | Χ | ||||||
| 112 | Leung, PPL et al., [ ] | 2021 | Case Study | Χ | ||||||
| 113 | Weber, S et al., [ ] | 2021 | Survey | Χ | ||||||
| 114 | Hogervorst, S et al., [ ] | 2021 | Survey | Patients (11), group HCPs (5 + 6), interviews HCPs (4) | Thematical analysis | Χ | ||||
| 115 | Khan, ich et al., [ ] | 2021 | Systematic Literature Review | Χ | ||||||
| 116 | Cherif, et al., [ ] | 2021 | Survey | Χ | ||||||
| 117 | Bingham, et al., [ ] | 2021 | Survey | 19 registered nurses | Descriptive statistics | Χ | ||||
| 118 | Broich, et al., [ ] | 2021 | Survey | Χ | ||||||
| 119 | Klemme, et al., [ ] | 2021 | Survey | The study consisted of 15 semi-structured interviews with academic staff ( = 7 professors and postdoctoral researchers, three female, four male) in the field of intelligent systems and technology in healthcare and staff at practice partners ( = 8 heads of department, two female, six male) in healthcare technology and economy (a hospital, a digital innovation and engineering company and a manufacturer of household appliances) and social institutions (foundations and aid organisations for people with disabilities). | Qualitative analysis | Χ | Χ | |||
| 120 | Dillenseger, et al., [ ] | 2021 | Survey | Χ | ||||||
| 121 | Wangler, et al., [ ] | 2021 | Survey | Χ | ||||||
| 122 | Kuhn, et al., [ ] | 2021 | Survey | Students (35) | Qualitative analysis | Χ | ||||
| 123 | Aldekhyyel, et al., [ ] | 2021 | Survey | Χ | ||||||
| 124 | Christlein, et al., [ ] | 2021 | Survey | Χ | ||||||
| 125 | Bergier, et al., [ ] | 2021 | Survey | Χ | ||||||
| 126 | Sitges-Macia, et al., [ ] | 2021 | Survey | Χ | ||||||
| 127 | Rani, et al., [ ] | 2021 | Survey | Χ | ||||||
| 128 | Fredriksen, et al., [ ] | 2021 | Case Study | Healthcare employees from a volunteer centre and from municipality healthcare units in three municipalities | Qualitative analysis | Χ | ||||
| 129 | Caixeta, et al., [ ] | 2021 | Survey | Χ | ||||||
| 130 | Gupta, et al., [ ] | 2021 | Survey | Χ | ||||||
| 131 | Dobson, et al., [ ] | 2021 | Survey | Χ | ||||||
| 132 | Choi, K et al., [ ] | 2021 | Survey | Χ | ||||||
| 133 | Muller-Wirtz, et al., [ ] | 2021 | Case Study | Χ | ||||||
| 134 | Sembekov, et al., [ ] | 2021 | Survey | Χ | ||||||
| 135 | Aulenkamp, et al., [ ] | 2021 | Survey | Χ | Χ | |||||
| 136 | Paul, et al., [ ] | 2021 | Survey | 16 key stakeholders | Thematical analysis | Χ | ||||
| 137 | Lemmen, et al., [ ] | 2021 | Survey | 62 citizens and 13 patients | Qualitative analysis | Χ | ||||
| 138 | Golz, et al., [ ] | 2021 | Survey | Χ | ||||||
| 139 | Tarikere, et al., [ ] | 2021 | Survey | Χ | ||||||
| 140 | Li, et al., [ ] | 2021 | Case Study | Χ | ||||||
| 141 | Rouge-Bugat, et al., [ ] | 2021 | Case Study | Χ | ||||||
| 142 | Iodice, et al., [ ] | 2021 | Survey | Χ | ||||||
| 143 | Kulzer, B [ ] | 2021 | Survey | Χ | ||||||
| 144 | Khosla, et al., [ ] | 2021 | Survey | Χ | ||||||
| 145 | Dantas, et al., [ ] | 2021 | Survey | Χ | ||||||
| 146 | Gaur, et al., [ ] | 2021 | Survey | Χ | ||||||
| 147 | Khodadad-Saryazdi, A [ ] | 2021 | Case Study | Χ | Χ | Χ | ||||
| 148 | Bellavista, et al., [ ] | 2021 | Case Study | Χ | ||||||
| 149 | Laukka, et al., [ ] | 2021 | Case Study | Χ | Χ | |||||
| 150 | Singh, et al., [ ] | 2021 | Survey | Χ | ||||||
| 151 | Patalano, et al., [ ] | 2021 | Survey | Χ | ||||||
| 152 | Mantel-Teeuwisse, et al., [ ] | 2021 | Survey | Χ | ||||||
| 153 | Mues, et al., [ ] | 2021 | Survey | Χ | ||||||
| 154 | Bosch-Capblanch, et al., [ ] | 2021 | Survey | Χ | ||||||
| 155 | Jaboyedoff, et al., [ ] | 2021 | Survey | 336 common data elements (CDEs) | Qualitative analysis | Χ | ||||
| 156 | Nadhamuni, et al., [ ] | 2021 | Survey | Χ | ||||||
| 157 | Hertling, et al., [ ] | 2021 | Survey | Χ | ||||||
| 158 | Khan, et al., [ ] | 2021 | Survey | Χ | ||||||
| 159 | Mun, et al., [ ] | 2021 | Survey | Χ | Χ | |||||
| 160 | Xi, et al., [ ] | 2021 | Survey | Χ | ||||||
| 161 | Weichert, et al., M [ ] | 2021 | Survey | Χ | ||||||
| 162 | Liang, et al., [ ] | 2021 | Survey | Χ | ||||||
| 163 | Williams, et al., [ ] | 2021 | Survey | 508 interviews, 163 observed meetings, and analysis of 325 documents. | Qualitative analysis—Sociotechnical principles, combining deductive and inductive methods | Χ | ||||
| 164 | Feroz, et al., [ ] | 2021 | Case Study | Χ | ||||||
| 165 | Huser, et al., [ ] | 2021 | Case Study | Χ | ||||||
| 166 | Apostolos, K [ ] | 2021 | Survey | Χ | ||||||
| 167 | Simsek, et al., [ ] | 2021 | Survey | Χ | Χ | |||||
| 168 | Khamisy-Farah, et al., [ ] | 2021 | Survey | Χ | ||||||
| 169 | Egarter, et al., [ ] | 2021 | Case Study | Χ | ||||||
| 170 | Can, et al., [ ] | 2021 | Survey | Χ | ||||||
| 171 | Sung, et al., [ ] | 2021 | Survey | 278 e-logbook database entries and 379 procedures in the hospital records from 14 users were analysed. Interviews with 12 e-logbook users found overall satisfaction. | Statistical analysis | Χ | Χ | |||
| 172 | Zoellner, et al., [ ] | 2021 | Survey | Χ | ||||||
| 173 | Oliveira, et al., [ ] | 2021 | Case Study | Recipients numbering 151 (21% of the universe) completed the questionnaire: trade (49), industry (41), services (28), health (15), and education (18). | Quantitative analysis | Χ | ||||
| 174 | Goudarzi, et al., [ ] | 2021 | Survey | Χ | ||||||
| 175 | Li, et al., [ ] | 2021 | Survey | Χ | Χ | |||||
| 176 | Klimanov, et al., [ ] | 2021 | Case Study | Χ | ||||||
| 177 | Nadav, et al., [ ] | 2021 | Survey | Eight focus group interviews were conducted with 30 health and social care professionals | Qualitative analysis | Χ | ||||
| 178 | Spanakis, et al., [ ] | 2021 | Survey | Χ | ||||||
| 179 | Polyakov, et al., [ ] | 2021 | Survey | Χ | ||||||
| 180 | Fristedt, et al., [ ] | 2021 | Survey | Intervention group ( = 80) & control group ( = 80) | Data will be coded and manually entered in SPSS | Χ | ||||
| 181 | Mandal, et al., [ ] | 2021 | Survey | Χ | ||||||
| 182 | Ozdemir, V [ ] | 2021 | Survey | Χ | ||||||
| 183 | Eberle, et al., [ ] | 2021 | Survey | Χ | ||||||
| 184 | Iakovleva, et al., [ ] | 2021 | Case Study | Χ | ||||||
| 185 | von Solodkoff, et al., [ ] | 2021 | Survey | In the questionnaire, the participants ( = 217). A total of 27 subjects (mean age 51 years, min: 23 years, max: 86 years) participated in the interviews. | Statistical analysis | Χ | ||||
| 186 | Khuntia, et al., [ ] | 2021 | Survey | Χ | Χ | |||||
| 187 | Ochoa, et al., [ ] | 2021 | Survey | Χ | ||||||
| 188 | Masłoń-Oracz, et al., [ ] | 2021 | Case Study | X | X | |||||
| 189 | Abrahams, et al., [ ] | 2020 | Survey | X | X | |||||
| 190 | Agnihothri, et al., [ ] | 2020 | Survey | X | ||||||
| 191 | Bukowski, et al., [ ] | 2020 | Survey | X | X | |||||
| 192 | Chiang, et al., [ ] | 2020 | Survey | X | X | |||||
| 193 | Cobelli, et al., [ ] | 2020 | Survey | Pharmacists (82) | Qualitative content analysis | X | ||||
| 194 | Crawford, et al., [ ] | 2020 | Survey | X | X | |||||
| 195 | Gjellebæk, et al., [ ] | 2020 | Case Study | Employees and middle managers | Thematic analysis | X | ||||
| 196 | Nascimento, et al., [ ] | 2020 | Case Study | X | ||||||
| 197 | Geiger, et al., [ ] | 2020 | Case Study | Specialist in neurosurery & resident (296) | Statistical Analysis | X | X | |||
| 198 | Eden, et al., [ ] | 2020 | Survey | Medical, nursing, allied health, administrative and executive roles (92) | Analysis of Cohen’s kappa (k) | X | X | |||
| 199 | Gochhait, et al., [ ] | 2020 | Case Study | X | X | |||||
| 200 | Kernebeck, et al., [ ] | 2020 | Case Study | X | ||||||
| 201 | Klinker, et al., [ ] | 2020 | Survey | Staff of health care facilities (14) | Microsoft HoloLens, Vuzix m100 | X | ||||
| 202 | Krasuska, et al., M.; Williams, R.; Sheikh, A.; Franklin, B. D.; Heeney, C.; Lane, W.; Mozaffar, H.; Mason, K.; Eason, et al., [ ] | 2020 | Survey | Staff of health care facilities (113) | Qualitative analysis | X | ||||
| 203 | Leigh, et al., [ ] | 2020 | Survey | X | ||||||
| 204 | Minssen, et al., [ ] | 2020 | Survey | X | ||||||
| 205 | Mueller, et al., [ ] | 2020 | Case Study | Staff of health care facilities (20) | Qualitative analysis | X | X | |||
| 206 | Nadarzynski, et al., [ ] | 2020 | Case Study | Patients (257) | Statistical analysis | X | X | |||
| 207 | Pekkarinen, et al., [ ] | 2020 | Case Study | Variety of participants (24) | The analytical framework is based on Nardi and O’Day’s five components of information ecology: system, diversity, co-evolution, keystone species, and locality. | X | ||||
| 208 | Rajamäki, et al., [ ] | 2020 | Survey | X | ||||||
| 209 | Salamah, et al., [ ] | 2020 | Case Study | X | ||||||
| 210 | Stephanie, et al., [ ] | 2020 | Survey | X | ||||||
| 211 | Sultana, et al., [ ] | 2020 | Survey | X | X | |||||
| 212 | Visconti, et al., [ ] | 2020 | Case Study | X | ||||||
| 213 | Yousaf et al., [ ] | 2020 | Case Study | X | ||||||
| 214 | Asthana, et al., [ ] | 2019 | Survey | X | ||||||
| 215 | Astruc, B. [ ] | 2019 | Case Study | X | X | |||||
| 216 | Baltaxe, et al., [ ] | 2019 | Report | X | ||||||
| 217 | Caumanns, J. [ ] | 2019 | Case Study | X | ||||||
| 218 | Diamantopoulos, et al., [ ] | 2019 | Case Study | X | X | |||||
| 219 | Diviani, et al., [ ] | 2019 | Survey | Variety of participants (165) | Qualitative analysis | X | ||||
| 220 | EYGM [ ] | 2019 | Survey | X | ||||||
| 221 | Hatzivasilis, et al., [ ] | 2019 | Survey | X | ||||||
| 222 | Go Jefferies, et al., [ ] | 2019 | Case Study | X | X | |||||
| 223 | Kivimaa, P., et al., [ ] | 2019 | Systematic Literature Review | X | ||||||
| 224 | Klocek, A., et al., [ ] | 2019 | Case Study | Variety of people (153) | Statistical analysis | X | ||||
| 225 | Kohl, S., et al., [ ] | 2019 | Survey | X | ||||||
| 226 | Kouroubali, et al., [ ] | 2019 | Case Study | X | X | |||||
| 227 | Manard, et al., [ ] | 2019 | Case Study | X | ||||||
| 228 | Mende M. [ ] | 2019 | Survey | X | ||||||
| 229 | Mishra et al., [ ] | 2019 | Systematic Literature Review | X | X | X | ||||
| 230 | Niemelä, et al., [ ] | 2019 | Survey | Health professionals, child patients’ parents, and the healthcare industry | Systematically analysed according to the process structure (pre-, intra-, post-surgery, and home care). | X | ||||
| 231 | Nittas, V., et al. [ ] | 2019 | Survey | X | ||||||
| 232 | Noor, A. [ ] | 2019 | Case Study | Students and Staff in colleges and universities | Qualitative analysis | X | ||||
| 233 | Pape, L., et al. [ ] | 2019 | Case Study | X | ||||||
| 234 | Patrício, et al., [ ] | 2019 | Survey | X | ||||||
| 235 | Russo Spena, T., Cristina, M. [ ] | 2019 | Survey | X | ||||||
| 236 | Rydenfält, C., et al., [ ] | 2019 | Case Study | Variety of people (264) | NVivo 10 (QSR International, Melbourne, Australia) | X | ||||
| 237 | Savikko, et al., [ ] | 2019 | Case Study | X | ||||||
| 238 | Vial, G [ ] | 2019 | Systematic Literature Review | X | ||||||
| 239 | Wangdahl, J.M., et al., [ ] | 2019 | Case Study | Variety of people (600) | Binary logistic regression analysis | X | ||||
| 240 | Watson, et al., [ ] | 2019 | Systematic Literature Review | X | ||||||
| 241 | Weigand, et al., [ ] | 2019 | Survey | X | ||||||
| 242 | Zanutto, A. [ ] | 2019 | Survey | Staff of health care facilities (6836) | Qualitative analysis | X | ||||
| 243 | Eden, et al., [ ] | 2018 | Systematic Literature Review | X | ||||||
| 244 | Goh, W., et al. [ ] | 2018 | Survey | X | ||||||
| 245 | Kayser, L., et al., [ ] | 2018 | Survey | X | ||||||
| 246 | Poss-Doering, R. et al., [ ] | 2018 | Case Study | Patients (11) & Doctors (3) | Statistical analysis | X | X | X | ||
| 247 | Khatoon, et al., [ ] | 2018 | Survey | X | X | |||||
| 248 | Melchiorre, M.G., et al., [ ] | 2018 | Case Study | X | ||||||
| 249 | Ngwenyama, et al., [ ] | 2018 | Survey | X | ||||||
| 250 | Öberg, U.A.-O., et al., [ ] | 2018 | Survey | Primary healthcare nurses (20) | Qualitative analysis | X | ||||
| 251 | Parkin, et al., [ ] | 2018 | Report | X | ||||||
| 252 | Tuzii, J., [ ] | 2018 | Case Study | X | ||||||
| 253 | Brockes, C., et al., [ ] | 2017 | Survey | Students (28) | Mann–Whitney U-Test | X | X | |||
| 254 | Cavusoglu, et al., [ ] | 2017 | Survey | X | ||||||
| 255 | Cerdan, et al., [ ] | 2017 | Case Study | Patients (29) | Qualitative analysis | X | ||||
| 256 | Coppolino, et al., [ ] | 2017 | Survey | X | ||||||
| 257 | Geiger, et al., [ ] | 2017 | Survey | X | ||||||
| 258 | Giacosa, et al., [ ] | 2017 | Survey | X | ||||||
| 259 | Hong, et al., [ ] | 2017 | Survey | X | ||||||
| 260 | Hüsers, J., et al., [ ] | 2017 | Case Study | Nurses (534) | All data were analysed using R (Version 3.2.1) | X | ||||
| 261 | Parviainen, et al., [ ] | 2017 | Survey | X | ||||||
| 262 | Paulin, A. [ ] | 2017 | Survey | X | ||||||
| 263 | Schobel, J., et al. [ ] | 2017 | Survey | X | ||||||
| 264 | Seddon, et al., [ ] | 2017 | Survey | X | ||||||
| 265 | Thorseng, et al., [ ] | 2017 | Survey | Variety of participants | Qualitative analysis | X | ||||
| 266 | Tuzii, J. [ ] | 2017 | Case Study | X | ||||||
| 267 | Amato, F., et al., [ ] | 2016 | Survey | X | ||||||
| 268 | Bongaerts, et al., [ ] | 2016 | Survey | X | ||||||
| 269 | Cucciniello, et al., [ ] | 2016 | Survey | X | ||||||
| 270 | Evans, R.S. [ ] | 2016 | Survey | X | ||||||
| 271 | Faried, et al., [ ] | 2016 | Report | X | ||||||
| 272 | Harjumaa, M., et al., [ ] | 2016 | Survey | Various organisations (12) | Interview data was then analysed thematically. | X | ||||
| 273 | Mattsson, T., [ ] | 2016 | Case Study | X | ||||||
| 274 | Mazor, et al., [ ] | 2016 | Survey | X | ||||||
| 275 | Anwar, et al., [ ] | 2015 | Survey | X | X | |||||
| 276 | Kostkova, P., [ ] | 2015 | Survey | X | ||||||
| 277 | Laur, A., [ ] | 2015 | Survey | X | ||||||
| 278 | Sultan, N., [ ] | 2015 | Survey | X | X | |||||
| 279 | Nudurupati, et al., [ ] | 2015 | Survey | X | ||||||
| 280 | Sanders, K., et al., [ ] | 2015 | Survey | Healthcare professionals (17) | Qualitative analysis | X | ||||
| 281 | Cook, et al., [ ] | 2012 | A Systematic Literature Review | X | ||||||
| 282 | Khan, et al., [ ] | 2012 | Survey | X | ||||||
| 283 | Agarwal, R., et al., [ ] | 2010 | Survey | X | ||||||
| 284 | Thomas, et al., [ ] | 2009 | Case Study | X | ||||||
| 285 | Buccoliero, et al., [ ] | 2008 | Survey | X | ||||||
| 286 | Hikmet, et al., [ ] | 2008 | Case Study | Variety of participants | Quantitive analysis | X | ||||
| 287 | Zdravković, S. [ ] | 2008 | Survey | Χ | X | |||||
5. Analysis of Concepts
From the articles included in the present study between 2008 and 2021, they were grouped into five categories identified: (i) information technology in health, (ii) acceptance of e-health, (iii) telemedicine, (iv) security of e-health, and (v) education impact of e-health.
5.1. Information Technology in Health
Researchers have studied several factors to maximise the effectiveness and success of adopting new technology to benefit patients. Hospitals can benefit from information technology when designing or modifying new service procedures. Health units can use information and communication technology applications to analyse and identify patients’ needs and preferences, enhancing their service innovation processes. Previous findings conclude that technological capability positively influences patient service and innovation in the service process [ 301 ]. These results have significant management implications as managers seek to increase technology resources’ efficiency to achieve patient-centred care as the cornerstone of medical practice [ 207 ].
Informatics facilitates the exchange of knowledge necessary for creating ideas and the development process. The internet supports health organisations in developing and distributing their services more efficiently [ 206 ]. Also, Information Technology improves the quality of services, reduces costs, and helps increase patient satisfaction. As new technologies have created opportunities for companies developing high-tech services, healthcare units can increase customer value, personalise services and adapt to their patient’s needs [ 209 ]. To this end, the “smart hospitals” should represent the latest investment frontiers impacting healthcare. Their technological characteristics are so advanced that the public authorities need know-how for their conception, construction, and operation [ 228 ].
A new example is reshaping global healthcare services in their infancy, emphasising the transition from sporadic acute healthcare to continuous and comprehensive healthcare. This approach is further refined by “anytime and everywhere access to safe eHealth services.” Recent developments in eHealth, digital transformation and remote data interchange, mobile communication, and medical technology are driving this new paradigm. Follow-up and timely intervention, comprehensive care, self-care, and social support are four added features in providing health care anywhere and anytime [ 289 ]. However, the healthcare sector’s already precarious security and privacy conditions are expected to be exacerbated in this new example due to the much greater monitoring, collection, storage, exchange, and retrieval of patient information and the cooperation required between different users, institutions, and systems.
The use of mobile telephony technologies to support health goals contributes to the transformation of healthcare benefits worldwide. The same goes for small and medium-sized healthcare companies, such as pharmacies. A potent combination of factors between companies and customers is the reason for creating new relationships. In particular, mobile technology applications represent new opportunities for integrating mobile health into existing services, facilitating the continued growth of quality service management. Service-based, service-focused strategies have changed distribution patterns and the relationship between resellers and consumers in the healthcare industry, resulting in mobile health and significant pharmacy opportunities. It has been an important research topic in the last decade because it has influenced and changed traditional communication between professionals and patients [ 211 ]. An example of a mobile healthcare platform is “Thymun”, designed and developed by Salamah et al. aiming to create intelligent health communities to improve the health and well-being of autoimmune people in Indonesia [ 225 ].
5.2. Acceptance of E-Health
In a long-term project and a population study (1999–2002), Hsu et al. evaluated e-health usage patterns [ 302 ]. The authors conclude that access to and use of e-health services are rapidly increasing. These services are more significant in people with more medical needs. Fang (2015) shows that scientific techniques can be an essential tool for revealing patterns in medical research that could not be apparent with traditional methods of reviewing the medical literature [ 303 ]. Teleradiology and telediagnosis, electronic health records, and Computer-Aided Diagnosis (CAD) are examples of digital medical technology. France is an example of a country that invests and leads in electronic health records, based on what is written by Manard S. et al. [ 243 ]. However, the impact of technological innovation is reflected in the availability of equipment and new technical services in different or specialised healthcare sectors.
On the other hand, Mariusz Duplaga (2013) argues that the expansion of e-health solutions is related to the growing demand for flexible, integrated and cost-effective models of chronic care [ 304 ]. The scope of applications that can support patients with chronic diseases is broad. In addition to accessing educational resources, patients with chronic diseases can use various electronic diaries and systems for long-term disease monitoring. Depending on the disease and the symptoms, the devices used to assess the patient’s condition vary. However, the need to report symptoms and measurements remains the same. According to Duplaga, the success of treatments depends on the patient’s involvement in monitoring and managing the disease. The emphasis on the role of the patient is parallel to the general tendency of people and patients to participate in decisions made about their health. Involving patients in monitoring their symptoms leads to improved awareness and ability to manage diseases. Duplaga argues that the widespread use of e-health systems depends on several factors, including the acceptance and ability to use information technology tools, combined with an understanding of disease and treatment.
Sumedha Chauhan & Mahadeo Jaiswal (2017) are on the same wavelength. They claim that e-health applications provide tools, processes and communication systems to support e-health practices [ 305 ]. These applications enable the transmission and management of information related to health care and thus contribute to improving patient’s health and physicians’ performance. The human element plays a critical role in the use of e-health, according to the authors. In addition, researchers have studied the acceptance of e-health applications among patients and the general public, as they use services such as home care and search for information online. The meta-analysis they use combines and analyzes quantitative findings of multiple empirical studies providing essential knowledge. However, the reason for their research was the study of Holden and Karsh (2010) [ 306 ].
To provide a comprehensive view of the literature acceptance of e-health applications, Holden and Karsh reviewed 16 studies based on healthcare technology acceptance models [ 306 ]. Findings show them that the use and acceptance of technological medical solutions bring improvements but can be adopted by those involved in the medical field.
5.3. Telemedicine
On the other hand, telemedicine is considered one of the most important innovations in health services, not only from a technological but also from a cultural and social point of view. It benefits the accessibility of healthcare services and organisational efficiency [ 215 ]. Its role is to meet the challenges posed by the socio-economic change in the 21st century (higher demands for health care, ageing population, increased mobility of citizens, need to manage large volumes of information, global competitiveness, and improved health care provision) in an environment with limited budgets and costs. Nevertheless, there are significant obstacles to its standardisation and complete consolidation and expansion [ 300 ].
At present, there are Telemedicine centres that mediate between the patient and the hospital or doctor. However, many factors make this communication impossible [ 300 ]. Such factors include equipment costs, connectivity problems, the patient’s trust or belief in the system or centre that applies telemedicine, and resistance to new and modern diagnostics, especially in rural and island areas. Therefore, telemedicine would make it easier to provide healthcare systems in remote areas than having a specialist in all the country’s remote regions [ 300 ]. Analysing the concept further, one can easily argue that the pros outweigh the disadvantages. Therefore, telemedicine must be adopted in a concerted effort to resolve all the obstacles we are currently facing. Telemedicine centres and services such as teleradiology, teledermatology, teleneurology, and telemonitoring will soon be included. This means that a few years from now, the patient will not have to go to a central hospital and can benefit remotely from the increased quality of health services. This will save valuable time, make good use of available resources, save patient costs, and adequately develop existing and new infrastructure.
In 2007, the World Health Organisation adopted the following broad description of telemedicine: “The delivery of health care services, where distance is a critical factor, by all health care professionals using information and communication technologies for the exchange of valid information for the diagnosis, treatment and prevention of disease and injuries, research and evaluation, and for the continuing education of health care providers, all in the interests of advancing the health of individuals and their communities ” [ 307 ]
According to the Wayback Machine, Canadian Telehealth Forum, other terms similar to telemedicine are telehealth and e-health, which are used as broader concepts of remote medical therapy. It is appropriate to clarify that telemedicine refers to providing clinical services. In contrast, telehealth refers to clinical and non-clinical services, including education, management and research in medical science. On the other hand, the term eHealth, most commonly used in the Americas and Europe, consists of telehealth and other elements of medicine that use information technology, according to the American Telemedicine Association [ 308 ].
The American Telemedicine Association divides telemedicine into three categories: storage-promotion, remote monitoring, and interactive services. The first category includes medical data, such as medical photographs, cardiograms, etc., which are transferred through new technologies to the specialist doctor to assess the patient’s condition and suggest the appropriate medication. Remote monitoring allows remote observation of the patient. This method is used mainly for chronic diseases like heart disease, asthma, diabetes, etc. Its interactive services enable direct communication between the patient and the treating doctor [ 309 ].
Telemedicine is a valuable and efficient tool for people living or working in remote areas. Its usefulness lies in the health access it provides to patients. In addition, it can be used as an educational tool for learning students and medical staff [ 310 ].
Telemedicine is an open and constantly evolving science, as it incorporates new technological developments and responds to and adapts to the necessary health changes within societies.
According to J.J. Moffatt, the most common obstacles to the spread of telemedicine are found in the high cost of equipment, the required technical training of staff and the estimated time of a meeting with the doctor, which can often be longer than the use of a standard doctor [ 311 ]. On the other hand, the World Health Organisation states that telemedicine offers excellent potential for reducing the variability of diagnoses and improving clinical management and the provision of health care services worldwide. The World Health Organisation claims, according to Craig et al. and Heinzelmann PJ, that telemedicine improves access, quality, efficiency and cost-effectiveness [ 312 , 313 ]. In particular, telemedicine can help traditionally under-served communities by overcoming barriers to the distance between healthcare providers and patients [ 314 ]. In addition, Jennett PA et al. highlight significant socio-economic benefits for patients, families, health professionals and the health system, including improved patient-provider communication and educational opportunities [ 315 ].
On the other hand, Wootton R. argues that telemedicine applications have achieved different levels of success. In both industrial and developing countries, telemedicine has yet to be used consistently in the healthcare system, and few pilot projects have been able to be maintained after the end of their initial funding [ 316 ].
However, many challenges are regularly mentioned and responsible for the need for more longevity in many efforts to adopt telemedicine. One such challenge is the complexity of human and cultural factors. Some patients and healthcare workers resist adopting healthcare models that differ from traditional approaches or home practices. In contrast, others need to have the appropriate educational background in Information and Communication Technologies to make effective use of telemedicine approaches [ 314 ]. The need for studies documenting telemedicine applications’ economic benefits and cost-effectiveness is also a challenge. Strong business acumen to persuade policymakers to embrace and invest in telemedicine has contributed to a need for more infrastructure and program funding [ 312 ]. Legal issues are also significant obstacles to the adoption of telemedicine. These include the need for an international legal framework that allows health professionals to provide services in different jurisdictions and countries. Furthermore, the lack of policies governing data confidentiality, authentication and the risk of medical liability for health professionals providing telemedicine services [ 314 ]. In any case, the technological challenges are related to legal issues. In addition, the systems used are complex, and there is a possibility of malfunction, which could cause software or hardware failure. The result is an increase in patient morbidity or mortality as well as the liability of healthcare providers [ 317 ].
According to Stanberry B., to overcome these challenges, telemedicine must be regulated by definitive and comprehensive guidelines, which are ideally and widely applied worldwide [ 318 ]. At the same time, legislation must be enacted governing health confidentiality, data access, and providers’ responsibility [ 314 ].
5.4. Security of eHealth
The possibility of the patients looking at the electronic patient folder in a cloud environment, through mobile devices anytime and anywhere, is significant. On the one hand, the advantages of cloud computing are essential, and on the other hand, a security mechanism is critical to ensure the confidentiality of this environment. Five methods are used to protect data in such environments: (1) users must encrypt the information before storing it; (2) users must transmit information through secure channels; (3) the user ID must be verified before accessing data; (4) the information is divided into small portions for handling and storage, retrieved when necessary; (5) digital signatures are added to verify that a suitable person has created the file to which a user has access. On the other hand, users of these environments will implement self-encryption to protect data and reduce over-reliance on providers [ 210 ].
At the same time, Maliha S. et al. [ 227 ] proposed the blockchain to preserve sensitive medical information. This technology ensures data integrity by maintaining a trace of control over each transaction. At the same time, zero trusts provide that medical data is encrypted and that only certified users and devices interact with the network. In this way, this model solves many vulnerabilities related to data security [ 227 ]. Another alternative approach is the KONFIDO project, which aims at the safe cross-border exchange of health data. A European H2020 project aims to address security issues through a holistic example at the system level. The project combines various cutting-edge technologies in its toolbox (such as blockchain, photonic Physical Unclonable Functions, homomorphic encryption, and trusted execution) [ 234 ]. Finally, Coppolino L. et al. [ 271 ] proposed using a SIEM framework for an e-healthcare portal developed under the Italian National eHealth Net Program. This framework allows real-time monitoring of access to the portal to identify potential threats and anomalies that could cause significant security issues [ 271 ].
5.5. Education Impact of E-Health
But all this would only be feasible with the necessary education of both users and patients [ 11 ]. As the volume and quality of evidence in medical education continue to expand, the need for evidence synthesis will increase [ 295 ]. On the other hand, Brockers C. et al. argued that digitalisation changes jobs and significantly impacts medical work. The quality of medical data provided for support depends on telemedicine’s medical specialisation and knowledge. Adjustments to primary and further education are inevitable because physicians are well trained to support their patients satisfactorily and confidently in the increasingly complex digitalisation of healthcare. The ultimate goal of the educational community is the closest approach of students to the issues of telemedicine and e-health, the creation of a spirit of trust, and the acceptance and transmission of essential knowledge [ 268 ].
Noor also moved in this direction, seeking to discover the gaps in Saudi education for digital transformation in health [ 248 ]. The growing complexity of healthcare systems worldwide and the growing reliance of the medical profession on information technology for precise practices and treatments require specific standardised training in Information Technology (IT) health planning. Accreditation of core Information Technology (IT) is advancing internationally. Noor A. examined the state of Information Technology health programmes in the Kingdom of Saudi Arabia (KSA) to determine (1) how well international standards are met and (2) what further development is required in the light of recent initiatives of the Kingdom of Saudi Arabia on e-health [ 248 ]. Of the 109 institutions that participated in his research, only a few offered programmes specifically in Health Information Technology. As part of Saudi Vision 2030, Saudi digital transformation was deemed an urgent need. This initiative calls for applying internationally accepted Information Technology skills in education programmes and healthcare practices, which can only happen through greater collaboration between medical and technology educators and strategic partnerships with companies, medical centres and government agencies.
Another study by Diviani N. et al. adds to the knowledge of e-health education, demonstrating how online health information affects a person’s overall behaviour and enhances patients’ ability to understand, live and prepare for various health challenges. The increasing digitalisation of communication and healthcare requires further research into the digital divide and patients’ relationships with health professionals. Healthcare professionals must recognise the online information they seek and engage with patients to evaluate online health information and support joint healthcare-making [ 235 ].
6. Discussion
The selected studies comprise a conceptual model based on bibliographic research. Using an open-ended technique, we analyse the selected 287 articles, which are grouped into categories based on their context. This methodology provides readers with a good indication of issues concerning the timeliness of health digitalisation. A limitation of the methodology is that selected criteria of the method might be subjective in terms of the search terms and how the papers are selected. The articles indicate that this field is initial, and further research is needed. Although several articles have created a theoretical basis for corporate sustainability and strategic digital management, only limited studies provided guidelines on the strategic digital transformation process and its health implementation stages. However, studies have also developed sustainable models, software or applications in this area. This is also the reason for creating opportunities for future researchers, who will be closed to investigate this gap and improve the viability of digital health strategies. In addition, any work carried out in case studies provides fruitful results by facilitating researchers through deep penetration into sustainable digitalisation. No generalised frameworks are available to guide the wording and implementation of digital action plans. Thus, the need for quantitative or qualitative research is created, providing conclusions on the impact of internal or external factors in the sustainability process, implementation, adoption, planning, and challenges of digital health solutions in general, as well as the impact of digital transformation. Most existing studies explore the issue of digitalisation in a particular part of a nursing institution or a disease rather than the management strategy perspective. In this way, researchers ignore a debate on obstacles and problems that often face in practice during integration. Such an analysis could lead to more profound knowledge.
7. Conclusions
In conclusion, our research observed a timeless analysis of systematised studies focusing on digital health developments. These studies broaden the researchers’ vision and provide vital information for further investigation. This article focuses on understanding digitalisation in healthcare, including, for the most part, the digitalisation of information and adopting appropriate parameters for further development. To build a more holistic view of digital health transformation, there is a great need for research on the management implications of digitalisation by different stakeholders. Finally, the development of telemedicine, the further enhancement of digital security and the strengthening of technological information systems will contribute to the universal acceptance of the digital health transformation by all involved.
Funding Statement
This research received no external funding.
Author Contributions
Conceptualisation, A.I.S., F.K. and M.A.T.; methodology, F.K. and M.A.T.; software, A.I.S.; validation, A.I.S.; data curation, A.I.S.; writing—original draft preparation, A.I.S. and M.A.T.; writing—review and editing, A.I.S. and M.A.T.; visualisation, A.I.S.; supervision, M.A.T.; project administration, M.A.T. All authors have read and agreed to the published version of the manuscript.
Institutional Review Board Statement
Informed consent statement, data availability statement, conflicts of interest.
The authors declare no conflict of interest.
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content.
- - Google Chrome
Intended for healthcare professionals
- My email alerts
- BMA member login
- Username * Password * Forgot your log in details? Need to activate BMA Member Log In Log in via OpenAthens Log in via your institution

Search form
- Advanced search
- Search responses
- Search blogs
- News & Views
- How the nursing...
How the nursing profession should adapt for a digital future
Read our collection on the future of nursing.
- Related content
- Peer review
- Richard G Booth , associate professor 1 ,
- Gillian Strudwick , scientist 2 ,
- Susan McBride , professor 3 ,
- Siobhán O’Connor , lecturer 4 ,
- Ana Laura Solano López , researcher 5
- 1 Arthur Labatt Family School of Nursing, Western University, London, Canada
- 2 Centre for Addiction and Mental Health, Toronto, Canada
- 3 School of Nursing, Texas Tech University Health Sciences Center, Lubbock, USA
- 4 School of Health in Social Science, University of Edinburgh, Edinburgh, UK
- 5 University of Costa Rica, San José, Costa Rica
- Correspondence to: R Booth rbooth6{at}uwo.ca
Transformation into a digitally enabled profession will maximize the benefits to patient care, write Richard Booth and colleagues
Digital technologies increasingly affect nursing globally. Examples include the growing presence of artificial intelligence (AI) and robotic systems; society’s reliance on mobile, internet, and social media; and increasing dependence on telehealth and other virtual models of care, particularly in response to the covid-19 pandemic.
Despite substantial advances to date, challenges in nursing’s use of digital technology persist. A perennial concern is that nurses have generally not kept pace with rapid changes in digital technologies and their impact on society. This limits the potential benefits they bring to nursing practice and patient care. To respond to these challenges and prepare for the future, nursing must begin immediate transformation into a digitally enabled profession that can respond to the complex global challenges facing health systems and society.
Many exemplars show how digital technologies already bring benefit to nursing practice and education. 1 For instance, telehealth programs where nurses provide daily monitoring, coaching, and triage of patients with several chronic diseases have helped reduce emergency department admissions. 2 Mobile devices, in particular smartphones and health applications, are enabling nurses to offer remote advice on pain management to adolescent patients with cancer 3 4 and supplement aspects of nursing education by providing innovative pedagogical solutions for content delivery and remote learning opportunities. 5
The development and application to nursing of systems based on AI are still in their infancy. But preliminary evidence suggests virtual chatbots could play a part in streamlining communication with patients, and robots could increase the emotional and social support patients receive from nurses, while acknowledging inherent challenges such as data privacy, ethics, and cost effectiveness. 6
Challenges persist
Digital technologies may, however, be viewed as a distraction from, or an unwelcome intrusion into, the hands-on caring role and therapeutic relationships that nurses have with patients and families. 7 This purported incompatibility with traditional nursing ideals, such as compassionate care, may explain some nurses’ reluctance to adopt digital approaches to healthcare. 8 9 In addition, nursing’s history was as structurally subordinate to other healthcare disciplines, 10 and the profession is still cementing its relationship and leadership in health systems.
The specialty of nursing informatics has long advocated for the integration of technology to support the profession, but it has comparatively few practitioners globally. Nursing informaticians are predominantly based in the United States, where the discipline seems to have originated, but many other countries and regions are expanding their digital nursing workforce and involvement with informatics. 11 12
Slow progress in some areas has been due to a lack of leadership and investment that supports nurses to champion and lead digital health initiatives. Globally, uncertainty remains regarding the next steps the nursing profession should take to increase and optimize its use of digital technology. This challenge is exacerbated by the global diversity of the profession, including unequal access to resources such as technological infrastructure maturity and expertise. Huge differences exist among countries and regions of the world in terms of the digitalization of healthcare processes, access to internet connectivity, and transparency of health information processes.
Selected technologies: benefits and challenges
The nursing literature contains many analyses of digital technologies used to support or extend the profession, including practice (eg, hospital information systems, electronic health records, monitoring systems, decision support, telehealth); education (eg, e-Learning, virtual reality, serious games); and, rehabilitative and personalized healthcare approaches (eg, assistive devices sensors, ambient assisted living). 1 T able 1 summarizes the potential benefits, challenges, and implications of emerging innovations to practice.
Benefits, challenges, and implications of selected digital technologies in nursing
- View inline
The table is not exhaustive, but the diversity of topics researched shows the profession recognizes the value and challenges of digital technologies. Given the evidence, for the profession to make further progress we recommend five areas for focused and immediate action. These recommendations should be qualified in light of regional context and professional background owing to global heterogeneity in nursing and the inclusion of digital technologies into healthcare.
Reform nursing education
We must urgently create educational opportunities at undergraduate and graduate levels in informatics, digital health, co-design, implementation science, and data science. 39 These should include opportunities to work with and learn from computing, engineering, and other interdisciplinary colleagues. For instance, nursing will need a critical mass of practitioners who understand how to use data science to inform the creation of nursing knowledge to support practice. 40 These practitioners will also need savviness and courage to lead the development of new models of patient care enabled by digital technologies. 41 42
Determining how, where, and why technology like AI should be used to support practice is of immediate interest and a growing competency requirement in health sciences and informatics education. 43 Nursing education should evolve its competencies and curriculums proactively for the increasing use of digital technologies in all areas of practice 39 while incorporating novel pedagogical approaches—for example, immersive technologies such as virtual and augmented reality—to deliver aspects of simulation based education. 44 45
Recently, the American Association of Colleges of Nursing released core competencies for nursing education, explicitly identifying informatics, social media, and emergent technologies and their impact on decision making and quality as critical to professional practice. 46
Build nursing leadership in digital health
All levels of nursing leadership must advocate more actively for, and invest resources in, a profession that is both complemented and extended by digital technology. The profession needs to evolve its use of digital technology by continuing to champion and support nurses to become knowledgeable in, and generate new scientific knowledge on, data analytics, virtual models of care, and the co-design of digital solutions with patients, differences across contexts and regions permitting.
Advancement of leadership competencies in existing informatics technologies, such as clinical decision support systems, electronic health records, and mobile technologies, is also essential: these kinds of systems will undoubtedly come with increasing levels of AI functionality. Possessing a critical mass of nursing leaders who understand the intended and unintended consequences as well as opportunities of these kinds of technologies is vital to ensure the quality and safety of nursing.
The increasing presence and recognition of the importance of chief nursing informatics officers is a step in the right direction. 47 Further, providing opportunities for nurses of all specialties to contribute to the development and implementation of digital health policies, locally and nationally, could increase future use of digital technologies in nursing.
Investigate artificial intelligence in nursing practice
The influence of AI on human decision making and labor are areas in need of immediate inquiry to support nursing practice for the next decade and beyond. AI technologies could provide the profession with huge benefits in data analytics and advanced clinical decision support.
Although many of the purported potential benefits of AI (eg, improved patient outcomes, streamlined workflow, improved efficiency) have yet to be fully shown in nursing research, 6 it is inevitable that AI technologies will be used more regularly to support and extend nurses’ cognitive, decision making, and potentially labor functions. 15
These opportunities bring new and dynamic practice considerations for nursing and interprofessional expertise. One example relates to the potential automation of inequity and injustice within systems and decision support tools containing AI 48 49 : self-evolving algorithms in systems sometimes unintentionally reinforce systemic inequities found in society.
Increased use of AI also brings novel policy, regulatory, legal, and ethical implications to the fore. The nursing profession must examine its role, processes, and knowledge against emerging ethical frameworks that explore the opportunities and risks that AI and similar innovations bring, while advocating for patient involvement in AI development and application. Floridi and colleagues offer tenets regarding AI development and the ethical considerations in using such innovations in their call to develop AI technology that “secures people’s trust, serves the public interest, and strengthens shared social responsibility.” 50 They also advocate that as guiding principles, AI should be used to enhance human agency, increase societal capacities, cultivate societal cohesion, and enable human self-realization, with an emphasis on instilling and reinforcing human dignity. 50 Further research, funding, and thought leadership in this domain are needed to help support the development of new practice policy, regulatory frameworks, and ethical guidelines to guide nursing practice.
Re-envision nurse-patient relationships
The profession must reframe how nurses interact with and care for patients in a digital world. The sheer variety of “do-it-yourself” health and wellness applications (eg, personalized genetic testing services, virtual mental health support), mobile and social media applications (eg, mHealth, wearables, online communities of practice) and other virtual healthcare (eg, telemedicine, virtual consultations) options available to consumers is impressive.
All this may seem antithetical toward the traditionally espoused nursing role—therapeutic relationships in physical interactions—but patients are increasingly empowered, connected to the internet, and demanding personalized or self-management healthcare models that fit their busy and varied lifestyles.
To maximize its impact on patient care, the profession should continue to develop virtual care modalities that exploit internet and mobile technology, drawing on its experiences with telehealth and remote models of care. 51 These care models might also be extended through virtual or augmented reality technologies or integrated with assisted living or “smart home” systems, 52 and potentially other precision and personalized healthcare solutions that leverage genomic and other biometric data.
Care approaches, interpretations of privacy, and technological interoperability functionalities should be co-designed among the interprofessional healthcare team, patients, and carers 53 and available where patients want them, ideally in both physical and digital realms. Deeper discussions and scientific research regarding access, cost, electronic resource use or wastage, and equity implications of the increasing digitalization of nurse-patient relationships will also need to be thoroughly explored.
Embrace digital practice
The profession requires a cultural shift. Its membership and leadership must demand the evolution of digital systems better to meet contemporary and emerging needs.
Too often, technology to support nursing is poorly configured, resourced, or not upgraded to respond to practice and societal trends. Nurses still commonly use practice systems that are lacking basic usability (eg, contributing to alert fatigue, reinforcing disruptive workflow processes) or generate added documentation burdens because of poor configuration and optimization. 54
There is huge variation globally in access to, integration of, and sustainability of digital technology. 55 56 57 Solutions vary and are context specific. Renewed awareness of digital technology’s use brought about by the covid-19 pandemic offers an impetus for change that nurses should embrace.
Tasks undertaken by nurses that do not add enough value to patient care present opportunities for partial or full divestment, 58 and may be better integrated into future technology enabled processes or delivered by other care providers.
The profession should revisit cultural interpretations of how technology such as drones, robots, and other AI enabled systems can be considered complementary to nursing practice and process, rather than as competition or adversaries. Collaboration with technology developers, providers, and patients will be essential to ensure success.
Although some outdated nursing activities and processes made redundant or less relevant will likely be missed by some in the profession, digital technology provides opportunities to support new models of care and approaches to nursing practice. We must not allow cultural and historical interpretations of nursing to upend or impede progress.
How nursing can stay relevant
Nurses entering the profession today will undoubtedly witness substantive disruption and change from digital technology by the time they are mid-career. 59 Without immediate action, the nursing profession stands to miss a remarkable opportunity to generate new roles, knowledge, and relationships within future health systems and societies saturated by digital technologies.
Nursing will continue to offer value and importance to healthcare systems in the coming decades. However, the profession must consider its role, knowledge, and relationships with technologies and patients to remain relevant in digitally enabled societies and healthcare systems and continue to provide compassionate care in a digital world. Without proactive strategic self-reflection, planning, and action, nursing will fail to control its trajectory across the chasm separating the past, present, and future of practice.
Key recommendations
Nursing must accelerate the transformation to a digitally enabled profession by investing in informatics education, research, and practice
Nurses should upskill in data science and other digital health topics to ensure emerging technologies such as AI are developed appropriately and safe for nursing practice and patient care
Nursing must invest in and lead digital health developments and collaborate with others to develop and deliver digital tools that patients and the public need
Nurses should champion informatics across all areas of professional practice, create leadership opportunities in digital health, and inform health policy in this area
Competing interests: We have read and understood BMJ policy on declaration of interests and have no relevant interests to declare.
Provenance and peer review: Commissioned; not externally peer reviewed.
This article is part of a series commissioned by The BMJ for the World Innovation Summit for Health (WISH). The BMJ peer reviewed, edited, and made the decision to publish. The series, including open access fees, is funded by WISH.
This is an Open Access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/ .
- Domhoff D ,
- Schmidt A ,
- Rothgang H ,
- Wolf-Ostermann K
- van Berkel C ,
- Horsfield D ,
- Duckworth H
- Stevens BJ ,
- Nathan PC ,
- Breakey V ,
- Chuang YH ,
- Buchanan C ,
- Howitt ML ,
- Robichaux C ,
- Sandelowski M
- O’Keefe-McCarthy S
- Fairman J ,
- D’Antonio P
- Bautista JR ,
- Sontag DA ,
- Halpern Y ,
- Jernite Y ,
- Shapiro NI ,
- Nathanson LA
- Chien S-C ,
- Pruinelli L
- Davenport T ,
- Klemets J ,
- Määttälä J ,
- Gjestsen MT ,
- Hoelscher D ,
- McBride S ,
- Hanley MA ,
- Bennett P ,
- Hardiker NR
- Akhu-Zaheya L ,
- Al-Maaitah R ,
- Bany Hani S
- Miyamoto S ,
- Dharmar M ,
- Tang-Feldman Y
- Dodson CH ,
- O’Connor S ,
- Alexander GL ,
- Powell KR ,
- Koivunen M ,
- Kurnat-Thoma E ,
- Starkweather A ,
- Jacelon CS ,
- Jolliffe S ,
- Stanmore E ,
- Renwick L ,
- Gwizdka J ,
- Chieng YJS ,
- Eijlers R ,
- Utens EMWJ ,
- Staals LM ,
- Kothgassner OD ,
- Van Eickels RL ,
- Plener PL ,
- Felnhofer A
- Tyrrell R ,
- Sarig-Bahat H ,
- Williams K ,
- Brennan PF ,
- Pepito JA ,
- McBride SG ,
- ↵ The American Association of Colleges of Nursing. The essentials: Core competencies for professional nursing education. 2021. https://www.aacnnursing.org/Education-Resources/AACN-Essentials
- Gianfrancesco MA ,
- Yazdany J ,
- Obermeyer Z ,
- Mullainathan S
- Floridi L ,
- Beltrametti M ,
- Demiris G ,
- Thompson HJ
- Spiegel B ,
- deBronkart D ,
- Eysenbach G
- Tolbert PH ,
- Konttila J ,
- Strudwick G ,
- McMurray J ,

School of Computer Science and Statistics
View the contact page for more contact and location information
- ADAPT Research Ireland Centre Impact Report reveals over €1 billion contribution to Ireland’s economy and society
ADAPT Research Ireland Centre Impact Report Reveals Over €1 Billion Contribution to Ireland’s Economy and Society
The ADAPT Research Ireland Centre for AI-Driven Digital Content Technology released its latest impact report today, showcasing the Centre’s significant contributions to the Irish economy and society valued at over €1.1 billion. Minister for Finance, Jack Chambers, officially launched the report, praising ADAPT for its groundbreaking research and collaboration across diverse sectors and acknowledged the Centre’s role as a key player in defending democracy in a digital age.
ADAPT has become a key player in addressing societal challenges, fostering innovation, and driving economic growth in Ireland through its multidisciplinary research platform. Leveraging €42 million in Government investment, ADAPT has delivered a 27.5 fold return, translating into over €1.1 billion in economic impact, solidifying its position as a leading global hub for AI research.
Launching the report, Minister for Finance, Jack Chambers TD , said: “This report clearly demonstrates ADAPT’s remarkable impact to the Irish economy and society more generally, in less than a decade. In a time where misinformation spreads rapidly, ADAPT’s work on AI and digital content is vital in combating this challenge. By advancing AI literacy and developing tools to detect deep fakes and misleading content, ADAPT ensures that technology strengthens trust and transparency in society. Their research equips individuals and institutions with the means to critically assess information, making them a key player in defending democracy in a digital world.”
Headquartered at the School of Computer Science and Statistics at Trinity College Dublin, ADAPT is one of Ireland’s flagship research centres funded by the Irish Government through Taighde Éireann – Research Ireland, and formerly funded under Science Foundation Ireland.
Celine Fitzgerald , CEO of Research Ireland, welcomed the report, saying: “In a competitive global landscape, research centres must show their value across a wide range of areas. This internationally peer-reviewed Centre Network has had a transformative economic and societal impact on Ireland. ADAPT exemplifies this by combining world-class research with a strong commitment to societal good, as demonstrated by award winning engaged research and their public engagement programme, which has connected with over 507,000 people.”

ADAPT has made a global impact through collaborations with 260 partners across 38 countries, positioning Ireland as a leader in AI research and innovation. The Centre has hosted 64 international conferences, which attracted nearly 24,000 delegates from around the world to Ireland. These conferences showcased cutting edge AI research and generated €38 million in economic activity through delegate spending on accommodation, dining, transport, and local services.
The Centre employs over 300 highly skilled professionals and has supported the creation of 1039 new research jobs in Ireland. It has nurtured 22 high-potential startups such as MoovAhead, SoapBox Labs, and Biologit, which have collectively generated more than 144 jobs and attracted over €340 million in multinational investment. These companies are boosting Ireland’s tech ecosystem and are at the forefront of fields such as immersive learning, digital mental health support, and voice AI.
Professor John D Kelleher, Professor of Computer Science & Director of the ADAPT Centre at Trinity College Dublin , said: “The potential of generative AI to reshape our world is limitless, but the path it takes depends on the choices we make now. At ADAPT, we’re fortunate to have a diverse community of researchers examining both the opportunities and risks of this technology. By drawing on world-class Irish-based researchers from a range of disciplines such as data science, AI, clinical sciences, and the humanities, our research focuses on how AI will shape critical areas such as work, education, culture, and healthcare.”
Key highlights of the report published today include:
Total Economic Impact : ADAPT’s activities from 2015 to 2023 generated an economic impact of over €1.1 billion, reflecting a 27.5-fold return on the Government’s investment.
Research Funding Success : ADAPT researchers secured over €177 million in competitive funding, including €50 million from EU sources, boosting Ireland’s standing in international research.
Government Investment Leverage : For every €1 invested by the State, ADAPT secured an additional €4.18 of inward investment from external sources such as industry and EU funding, demonstrating efficient leveraging of public funds.
Spin-Out Companies : ADAPT researchers have successfully spun out 22 companies, creating 144 new jobs and attracting over €340 million in foreign investment, which further strengthens Ireland’s economy.
Scientific Excellence: ADAPT researchers have authored more than 2,600 peer reviewed articles since January 2015 with over 60 of these papers earning prestigious best paper or presentation awards.
Talent Development: ADAPT has trained a total of 337 alumni, 40% of whom work in industry, while 49% are employed in academia. ADAPT’S alumni (since 2015) represent 39 different nationalities.
Industry Collaboration : ADAPT has engaged in over 60 collaborative projects with 72 industry partners across 32 countries, driving innovation and enhancing Ireland’s global competitiveness.
Commercialisation: ADAPT inventors have signed 77 licence agreements with companies in both Ireland and internationally.
Foreign Direct Investment (FDI ): ADAPT’s world-class research has influenced the decisions of 19 multinational companies to invest or expand their operations in Ireland, creating 591 new research jobs and bringing €172 million in investment.
International Conferences: Between 2015 and 2023, ADAPT hosted 64 international conferences. These conferences were attended by almost 24,000 delegates. The estimated impact of these conferences on the Irish economy is €38.1m.
AI Literacy and Public Engagement : ADAPT has reached over 507,000 members of the public, helping to build a greater understanding of AI and its influence on our everyday lives, including educating and building AI literacy for over 67,000 citizens through the #DiscussAI campaign.
ADAPT’s initial funding from the Irish Government currently extends through 2026, ensuring continued contributions to Ireland’s economy and the global AI research landscape.
The full Impact Report is available to download .

IMAGES
VIDEO
COMMENTS
Practical example of a quick adaptation from the past is the best answer. Saying that you adapt quickly to changes, or new technologies, without elaborating on it, won't take you far in the interviews. You should say something that demonstrates your ability to do so. For example, you can narrate a story from your last job.
The achievements of humanity over the last century have only been made possible by the development of modern technology. Driven by the need to discover, people have created countless innovations in fields such as electronics, medicine and engineering which have improved the lives of billions. Additionally, many key discoveries throughout ...
Another method of adapting to new technology includes taking advantage of mostly advanced technology, including software and computers in all classrooms. This is much better than having a single computer lab for a large number of students to share. The main benefit is more time with the technology for each student, as well as a.
A crucial part of understanding how technology has created global change and, in turn, how global changes have influenced the development of new technologies is understanding the technologies themselves in all their richness and complexity—how they work, the limits of what they can do, what they were designed to do, how they are actually used.
Introduction. Technological change improves the quality of life; supports the development of new products, industries, opportunities and experiences; increases productivity and leads to increased wages. Last century saw the impact of steam power, electricity, the filament light bulb, radio, television, the telephone, aeroplanes and the telegraph.
Google Classroom: Jordan Mittler, a sophomore at The Ramaz Upper School in New York City and a participant in the Wharton Global Youth Summer Program, is the founder of Mittler Senior Technology, a company that helps senior citizens adapt to the world of technology. In this student essay, Jordan shares the story of how he started his business ...
The advancement of technology ensures that communication is quicker and that more people remain connected. There has been an evolution in interpersonal skills with the advancement of technology, and users should always be keen on adapting to new ways of communication. Technology has continually brought new methods of communication leading to ...
Get a custom essay on New Technology's Influence on the Future---writers online . ... AI has the ability to analyze and understand complex data, make predictions, and adapt to new situations. AI technology is being applied in many industries, from healthcare to finance to transportation, to improve efficiency and decision-making (Costello ...
The onset of the fourth industrial revolution (Industry 4.0) presages far-reaching changes in the nature of work. Footnote 1 New occupations are likely to be concentrated in the nonroutine and cognitive category requiring higher-order cognitive and soft or socio-emotional skills (hereafter, referred to as 'soft skills'). Rising demand for high skills combined with shrinking shelf life of ...
Already, we have seen many companies move to new geographies to tap new talent pools. For example, a large technology company recently announced some roles could remain remote indefinitely, allowing them to leverage talent from around the country. Others, such as a large financial company that is planning on having 60 desks per 100 employees ...
Disruptive changes, understood as changes in a company and its operating environment caused by digitalization, possibly leading to the current business becoming obsolete (Parviainen et al., 2017), trigger DT in different environments due to rapid or disruptive innovations in digital technologies.These changes create high levels of uncertainty, and industries and companies try to adapt to these ...
Why is true tech adoption so difficult to achieve? Based on the authors' experience working on these issues, they see five key actions business leaders can take to create a culture that will ...
COVID-19 dramatically influenced students' and staff's learning and teaching experiences and approaches to learning. While many papers examined individual experiences in the context of higher education, synthesising these papers to determine enabling and hindering influences of digital adaptation was needed to guide the next phase of online learning reforms. This study explored the main ...
Another method of adapting to new technology includes taking advantage of mostly advanced technology, including software and computers in all classrooms. This is much better than having a single computer lab for a large number of students to share. ... essay The Effects of New Technology in Human Lives; essay Internet and New Technology;
Collaboration with technology developers, providers, and patients will be essential to ensure success. Although some outdated nursing activities and processes made redundant or less relevant will likely be missed by some in the profession, digital technology provides opportunities to support new models of care and approaches to nursing practice.
And if your employees thrive, your business will too. This article will outline eight proven strategies to help employees adapt to new technology in the workplace.: 1. Ask employees for their input. Let's start by tackling the first reason workers resist new technology: feeling excluded from the decision-making process.
Staff should also understand how the new technology will benefit them individually, he says. This creates the all-essential buy-in that can mitigate a chief roadblock to adoption and learning: resistance. In the Ouellette & Associates book Leading IT Transformation, managers are cautioned that "depending on the severity of the change ...
Research on the relationship between technology and an ageing society, on the one hand, points out the impact of technologies on older people, such as how older people use assistive technology to remain independent and care for themselves and use communication technology to build interactions (Czaja, 2017); on the other hand, it describes new ...
Also, Information Technology improves the quality of services, reduces costs, and helps increase patient satisfaction. As new technologies have created opportunities for companies developing high-tech services, healthcare units can increase customer value, personalise services and adapt to their patient's needs . To this end, the "smart ...
Transformation into a digitally enabled profession will maximize the benefits to patient care, write Richard Booth and colleagues Digital technologies increasingly affect nursing globally. Examples include the growing presence of artificial intelligence (AI) and robotic systems; society's reliance on mobile, internet, and social media; and increasing dependence on telehealth and other ...
Check out this FREE essay on Adapting to New Technology ️ and use it to write your own unique paper. New York Essays - database with more than 65.000 college essays for A+ grades ... Another method of adapting to new technology includes taking advantage of mostly advanced technology, including software and computers in all classrooms. This is ...
The ADAPT Research Ireland Centre for AI-Driven Digital Content Technology released its latest impact report today, showcasing the Centre's significant contributions to the Irish economy and society valued at over €1.1 billion. Minister for Finance, Jack Chambers, officially launched the report, praising ADAPT for its groundbreaking research and collaboration across diverse sectors and ...