- - Google Chrome
Intended for healthcare professionals
- Access provided by Google Indexer
- My email alerts
- BMA member login
- Username * Password * Forgot your log in details? Need to activate BMA Member Log In Log in via OpenAthens Log in via your institution


Search form
- Advanced search
- Search responses
- Search blogs
- Impact of vaping on...
Impact of vaping on respiratory health
Linked editorial.
Protecting children from harms of vaping
- Related content
- Peer review
- Andrea Jonas , clinical assistant professor
- Division of Pulmonary, Allergy, and Critical Care, Department of Medicine, Stanford University, Stanford, CA, USA
- Correspondence to A Jonas andreajonas{at}stanford.edu
Widespread uptake of vaping has signaled a sea change in the future of nicotine consumption. Vaping has grown in popularity over the past decade, in part propelled by innovations in vape pen design and nicotine flavoring. Teens and young adults have seen the biggest uptake in use of vape pens, which have superseded conventional cigarettes as the preferred modality of nicotine consumption. Relatively little is known, however, about the potential effects of chronic vaping on the respiratory system. Further, the role of vaping as a tool of smoking cessation and tobacco harm reduction remains controversial. The 2019 E-cigarette or Vaping Use-Associated Lung Injury (EVALI) outbreak highlighted the potential harms of vaping, and the consequences of long term use remain unknown. Here, we review the growing body of literature investigating the impacts of vaping on respiratory health. We review the clinical manifestations of vaping related lung injury, including the EVALI outbreak, as well as the effects of chronic vaping on respiratory health and covid-19 outcomes. We conclude that vaping is not without risk, and that further investigation is required to establish clear public policy guidance and regulation.
Abbreviations
BAL bronchoalveolar lavage
CBD cannabidiol
CDC Centers for Disease Control and Prevention
DLCO diffusing capacity of the lung for carbon monoxide
EMR electronic medical record
END electronic nicotine delivery systems
EVALI E-cigarette or Vaping product Use-Associated Lung Injury
LLM lipid laden macrophages
THC tetrahydrocannabinol
V/Q ventilation perfusion
Introduction
The introduction of vape pens to international markets in the mid 2000s signaled a sea change in the future of nicotine consumption. Long the mainstay of nicotine use, conventional cigarette smoking was on the decline for decades in the US, 1 2 largely owing to generational shifts in attitudes toward smoking. 3 With the advent of vape pens, trends in nicotine use have reversed, and the past two decades have seen a steady uptake of vaping among young, never smokers. 4 5 6 Vaping is now the preferred modality of nicotine consumption among young people, 7 and 2020 surveys indicate that one in five US high school students currently vape. 8 These trends are reflected internationally, where the prevalence of vape products has grown in both China and the UK. 9 Relatively little is known, however, regarding the health consequences of chronic vape pen use. 10 11 Although vaping was initially heralded as a safer alternative to cigarette smoking, 12 13 the toxic substances found in vape aerosols have raised new questions about the long term safety of vaping. 14 15 16 17 The 2019 E-cigarette or Vaping product Use-Associated Lung Injury (EVALI) outbreak, ultimately linked to vitamin E acetate in THC vapes, raised further concerns about the health effects of vaping, 18 19 20 and has led to increased scientific interest in the health consequences of chronic vaping. This review summarizes the history and epidemiology of vaping, and the clinical manifestations and proposed pathophysiology of lung injury caused by vaping. The public health consequences of widespread vaping remain to be seen and are compounded by young users of vape pens later transitioning to combustible cigarettes. 4 21 22 Deepened scientific understanding and public awareness of the potential harms of vaping are imperative to confront the challenges posed by a new generation of nicotine users.
Sources and selection criteria
We searched PubMed and Ovid Medline databases for the terms “vape”, “vaping”, “e-cigarette”, “electronic cigarette”, “electronic nicotine delivery”, “electronic nicotine device”, “END”, “EVALI”, “lung injury, diagnosis, management, and treatment” to find articles published between January 2000 and December 2021. We also identified references from the Centers for Disease Control and Prevention (CDC) website, as well as relevant review articles and public policy resources. Prioritization was given to peer reviewed articles written in English in moderate-to-high impact journals, consensus statements, guidelines, and included randomized controlled trials, systematic reviews, meta-analyses, and case series. We excluded publications that had a qualitative research design, or for which a conflict of interest in funding could be identified, as defined by any funding source or consulting fee from nicotine manufacturers or distributors. Search terms were chosen to generate a broad selection of literature that reflected historic and current understanding of the effects of vaping on respiratory health.
The origins of vaping
Vaping achieved widespread popularity over the past decade, but its origins date back almost a century and are summarized in figure 1 . The first known patent for an “electric vaporizer” was granted in 1930, intended for aerosolizing medicinal compounds. 23 Subsequent patents and prototypes never made it to market, 24 and it wasn’t until 1979 that the first vape pen was commercialized. Dubbed the “Favor” cigarette, the device was heralded as a smokeless alternative to cigarettes and led to the term “vaping” being coined to differentiate the “new age” method of nicotine consumption from conventional, combustible cigarettes. 25 “Favor” cigarettes did not achieve widespread appeal, in part because of the bitter taste of the aerosolized freebase nicotine; however, the term vaping persisted and would go on to be used by the myriad products that have since been developed.

Timeline of vape pen invention to widespread use (1970s-2020)
- Download figure
- Open in new tab
- Download powerpoint
The forerunner of the modern vape pen was developed in Beijing in 2003 and later introduced to US markets around 2006. 26 27 Around this time, the future Juul Laboratories founders developed the precursor of the current Juul vape pen while they were students at the Stanford Byers-Center for Biodesign. 28 Their model included disposable cartridges of flavored nicotine solution (pods) that could be inserted into the vape pen, which itself resembled a USB flash drive. Key to their work was the chemical alteration of freebase nicotine to a benzoate nicotine salt. 29 The lower pH of the nicotine salt resulted in an aerosolized nicotine product that lacked a bitter taste, 30 and enabled manufacturers to expand the range of flavored vape products. 31 Juul Laboratories was founded a decade later and quickly rose to dominate the US market, 32 accounting for an estimated 13-59% of the vape products used among teens by 2020. 6 8 Part of the Juul vape pen’s appeal stems from its discreet design, as well as its ability to deliver nicotine with an efficiency matching that of conventional cigarettes. 33 34 Subsequent generations of vape pens have included innovations such as the tank system, which allowed users to select from the wide range of different vape solutions on the market, rather than the relatively limited selection available in traditional pod based systems. Further customizations include the ability to select different vape pen components such as atomizers, heating coils, and fluid wicks, allowing users to calibrate the way in which the vape aerosol is produced. Tobacco companies have taken note of the shifting demographics of nicotine users, as evidenced in 2018 by Altria’s $12.8bn investment in Juul Laboratories. 35
Vaping terminology
At present, vaping serves as an umbrella term that describes multiple modalities of aerosolized nicotine consumption. Vape pens are alternatively called e-cigarettes, electronic nicotine delivery systems (END), e-cigars, and e-hookahs. Additional vernacular terms have emerged to describe both the various vape pen devices (eg, tank, mod, dab pen), vape solution (eg, e-liquid, vape juice), as well as the act of vaping (eg, ripping, juuling, puffing, hitting). 36 A conventional vape pen is a battery operated handheld device that contains a storage chamber for the vape solution and an internal element for generating the characteristic vape aerosol. Multiple generations of vape pens have entered the market, including single use, disposable varieties, as well as reusable models that have either a refillable fluid reservoir or a disposable cartridge for the vape solution. Aerosol generation entails a heating coil that atomizes the vape solution, and it is increasingly popular for devices to include advanced settings that allow users to adjust features of the aerosolized nicotine delivery. 37 38 Various devices allow for coil temperatures ranging from 110 °C to over 1000 °C, creating a wide range of conditions for thermal degradation of the vape solution itself. 39 40
The sheer number of vape solutions on the market poses a challenge in understanding the impact of vaping on respiratory health. The spectrum of vape solutions available encompasses thousands of varieties of flavors, additives, and nicotine concentrations. 41 Most vape solutions contain an active ingredient, commonly nicotine 42 ; however, alternative agents include tetrahydrocannabinol (THC) or cannabidiol (CBD). Vape solutions are typically composed of a combination of a flavorant, nicotine, and a carrier, commonly propylene glycol or vegetable glycerin, that generates the characteristic smoke appearance of vape aerosols. Some 450 brands of vape now offer more than 8000 flavors, 41 a figure that nearly doubled over a three year period. 43 Such tremendous variety does not account for third party sellers who offer users the option to customize a vape solution blend. Addition of marijuana based products such as THC or CBD requires the use of an oil based vape solution carrier to allow for extraction of the psychoactive elements. Despite THC vaping use in nearly 9% of high schoolers, 44 THC vape solutions are subject to minimal market regulation. Finally, a related modality of THC consumption is termed dabbing, and describes the process of inhaling aerosolized THC wax concentrate.
Epidemiology of vaping
Since the early 2000s, vaping has grown in popularity in the US and elsewhere. 8 45 Most of the 68 million vape pen users are concentrated in China, the US, and Europe. 46 Uptake among young people has been particularly pronounced, and in the US vaping has overtaken cigarettes as the most common modality of nicotine consumption among adolescents and young adults. 47 Studies estimate that 20% of US high school students are regular vape pen users, 6 48 in contrast to the 5% of adults who use vape products. 2 Teen uptake of vaping has been driven in part by a perception of vaping as a safer alternative to cigarettes, 49 50 as well as marketing strategies that target adolescents. 33 Teen use of vape pens is further driven by the low financial cost of initiation, with “starter kits” costing less than $25, 51 as well as easy access through peer sales and inconsistent age verification at in-person and online retailers. 52 After sustained growth in use over the 2010s, recent survey data from 2020 suggest that the number of vape pen users has leveled off among teens, perhaps in part owing to increased perceived risk of vaping after the EVALI outbreak. 8 53 The public health implications of teen vaping are compounded by the prevalence of vaping among never smokers (defined as having smoked fewer than 100 lifetime cigarettes), 54 and subsequent uptake of cigarette smoking among vaping teens. 4 55 Similarly, half of adults who currently vape have never used cigarettes, 2 and concern remains that vaping serves as a gateway to conventional cigarette use, 56 57 although these results have been disputed. 58 59 Despite regulation limiting the sale of flavored vape products, 60 a 2020 survey found that high school students were still predominantly using fruit, mint, menthol, and dessert flavored vape solutions. 48 While most data available surround the use of nicotine-containing vape products, a recent meta-analysis showed growing prevalence of adolescents using cannabis-containing products as well. 61
Vaping as harm reduction
Despite facing ongoing questions about safety, vaping has emerged as a potential tool for harm reduction among cigarette smokers. 12 27 An NHS report determined that vaping nicotine is “around 95% less harmful than cigarettes,” 62 leading to the development of programs that promote vaping as a tool of risk reduction among current smokers. A 2020 Cochrane review found that vaping nicotine assisted with smoking cessation over placebo 63 and recent work found increased rates of cigarette abstinence (18% v 9.9%) among those switching to vaping compared with conventional nicotine replacement (eg, gum, patch, lozenge). 64 US CDC guidance suggests that vaping nicotine may benefit current adult smokers who are able to achieve complete cigarette cessation by switching to vaping. 65 66
The public health benefit of vaping for smoking cessation is counterbalanced by vaping uptake among never smokers, 2 54 and questions surrounding the safety of chronic vaping. 10 11 Controversy surrounding the NHS claim of vaping as 95% safer than cigarettes has emerged, 67 68 and multiple leading health organizations have concluded that vaping is harmful. 42 69 Studies have demonstrated airborne particulate matter in the proximity of active vapers, 70 and concern remains that secondhand exposure to vaped aerosols may cause adverse effects, complicating the notion of vaping as a net gain for public health. 71 72 Uncertainty about the potential chronic consequences of vaping combined with vaping uptake among never smokers has complicated attempts to generate clear policy guidance. 73 74 Further, many smokers may exhibit “dual use” of conventional cigarettes and vape pens simultaneously, further complicating efforts to understand the impact of vape exposure on respiratory health, and the role vape use may play in smoking cessation. 12 We are unable to know with certainty the extent of nicotine uptake among young people that would have been seen in the absence of vaping availability, and it remains possible that some young vape pen users may have started on conventional cigarettes regardless. That said, declining nicotine use over the past several decades would argue that many young vape pen users would have never had nicotine uptake had vape pens not been introduced. 1 2 It remains an open question whether public health measures encouraging vaping for nicotine cessation will benefit current smokers enough to offset the impact of vaping uptake among young, never smokers. 75
Vaping lung injury—clinical presentations
Vaping related lung injury: 2012-19.
The potential health effects of vape pen use are varied and centered on injury to the airways and lung parenchyma. Before the 2019 EVALI outbreak, the medical literature detailed case reports of sporadic vaping related acute lung injury. The first known case was reported in 2012, when a patient presented with cough, diffuse ground glass opacities, and lipid laden macrophages (LLM) on bronchoalveolar lavage (BAL) return in the context of vape pen use. 76 Over the following seven years, an additional 15 cases of vaping related acute lung injury were reported in the literature. These cases included a wide range of diffuse parenchymal lung disease without any clear unifying features, and included cases of eosinophilic pneumonia, 77 78 79 hypersensitivity pneumonitis, 80 organizing pneumonia, 81 82 diffuse alveolar hemorrhage, 83 84 and giant cell foreign body reaction. 85 Although parenchymal lung injury predominated the cases reported, additional cases detailed episodes of status asthmaticus 86 and pneumothoraces 87 attributed to vaping. Non-respiratory vape pen injury has also been described, including cases of nicotine toxicity from vape solution ingestion, 88 89 and injuries sustained owing to vape pen device explosions. 90
The 2019 EVALI outbreak
In the summer of 2019 the EVALI outbreak led to 2807 cases of idiopathic acute lung injury in predominantly young, healthy individuals, which resulted in 68 deaths. 19 91 Epidemiological work to uncover the cause of the outbreak identified an association with vaping, particularly the use of THC-containing products, among affected individuals. CDC criteria for EVALI ( box 1 ) included individuals presenting with respiratory symptoms who had pulmonary infiltrates on imaging in the context of having vaped or dabbed within 90 days of symptom onset, without an alternative identifiable cause. 92 93 After peaking in September 2019, EVALI case numbers steadily declined, 91 likely owing to identification of a link with vaping, and subsequent removal of offending agents from circulation. Regardless, sporadic cases continue to be reported, and a high index of suspicion is required to differentiate EVALI from covid-19 pneumonia. 94 95 A strong association emerged between EVALI cases and the presence of vitamin E acetate in the BAL return of affected individuals 96 ; however, no definitive causal link has been established. Interestingly, the EVALI outbreak was nearly entirely contained within the US with the exception of several dozen cases, at least one of which was caused by an imported US product. 97 98 99 The pattern of cases and lung injury is most suggestive of a vape solution contaminant that was introduced into the distribution pipeline in US markets, leading to a geographically contained pattern of lung injury among users. CDC case criteria for EVALI may have obscured a potential link between viral pneumonia and EVALI, and cases may have been under-recognized following the onset of the covid-19 pandemic.
CDC criteria for establishing EVALI diagnosis
Cdc lung injury surveillance, primary case definitions, confirmed case.
Vape use* in 90 days prior to symptom onset; and
Pulmonary infiltrate on chest radiograph or ground glass opacities on chest computed tomography (CT) scan; and
Absence of pulmonary infection on initial investigation†; and
Absence of alternative plausible diagnosis (eg, cardiac, rheumatological, or neoplastic process).
Probable case
Pulmonary infiltrate on chest radiograph or ground glass opacities on chest CT; and
Infection has been identified; however is not thought to represent the sole cause of lung injury OR minimum criteria** to exclude infection have not been performed but infection is not thought to be the sole cause of lung injury
*Use of e-cigarette, vape pen, or dabbing.
†Minimum criteria for absence of pulmonary infection: negative respiratory viral panel, negative influenza testing (if supported by local epidemiological data), and all other clinically indicated infectious respiratory disease testing is negative.
EVALI—clinical, radiographic, and pathologic features
In the right clinical context, diagnosis of EVALI includes identification of characteristic radiographic and pathologic features. EVALI patients largely fit a pattern of diffuse, acute lung injury in the context of vape pen exposure. A systematic review of 200 reported cases of EVALI showed that those affected were predominantly men in their teens to early 30s, and most (80%) had been using THC-containing products. 100 Presentations included predominantly respiratory (95%), constitutional (87%), and gastrointestinal symptoms (73%). Radiological studies mostly featured diffuse ground glass opacities bilaterally. Of 92 cases that underwent BAL, alveolar fluid samples were most commonly neutrophil predominant, and 81% were additionally positive for LLM on Oil Red O staining. Lung biopsy was not required to achieve the diagnosis; however, of 33 cases that underwent tissue biopsy, common features included organizing pneumonia, inflammation, foamy macrophages, and fibrinous exudates.
EVALI—outcomes
Most patients with EVALI recovered, and prognosis was generally favorable. A systematic review of identified cases found that most patients with confirmed disease required admission to hospital (94%), and a quarter were intubated. 100 Mortality among EVALI patients was low, with estimates around 2-3% across multiple studies. 101 102 103 Mortality was associated with age over 35 and underlying asthma, cardiac disease, or mental health conditions. 103 Notably, the cohorts studied only included patients who presented for medical care, and the samples are likely biased toward a more symptomatic population. It is likely that many individuals experiencing mild symptoms of EVALI did not present for medical care, and would have self-discontinued vaping following extensive media coverage of the outbreak at that time. Although most EVALI survivors recovered well, case series of some individuals show persistent radiographic abnormalities 101 and sustained reductions in DLCO. 104 105 Pulmonary function evaluation of EVALI survivors showed normalization in FEV 1 /FVC on spirometry in some, 106 while others had more variable outcomes. 105 107 108
Vaping induced lung injury—pathophysiology
The causes underlying vaping related acute lung injury remain interesting to clinicians, scientists, and public health officials; multiple mechanisms of injury have been proposed and are summarized in figure 2 . 31 109 110 Despite increased scientific interest in vaping related lung injury following the EVALI outbreak, the pool of data from which to draw meaningful conclusions is limited because of small scale human studies and ongoing conflicts due to tobacco industry funding. 111 Further, insufficient time has elapsed since widespread vaping uptake, and available studies reflect the effects of vaping on lung health over a maximum 10-15 year timespan. The longitudinal effects of vaping may take decades to fully manifest and ongoing prospective work is required to better understand the impacts of vaping on respiratory health.

Schematic illustrating pathophysiology of vaping lung injury
Pro-inflammatory vape aerosol effects
While multiple pathophysiological pathways have been proposed for vaping related lung injury, they all center on the vape aerosol itself as the conduit of lung inflammation. Vape aerosols have been found to harbor a number of toxic substances, including thermal degradation products of the various vape solution components. 112 Mass spectrometry analysis of vape aerosols has identified a variety of oxidative and pro-inflammatory substances including benzene, acrolein, volatile organic compounds, and propylene oxide. 16 17 Vaping additionally leads to airway deposition of ultrafine particles, 14 113 as well as the heavy metals manganese and zinc which are emitted from the vaping coils. 15 114 Fourth generation vape pens allow for high wattage aerosol generation, which can cause airway epithelial injury and tissue hypoxia, 115 116 as well as formaldehyde exposure similar to that of cigarette smoke. 117 Common carrier solutions such as propylene glycol have been associated with increased airway hyper-reactivity among vape pen users, 31 118 119 and have been associated with chronic respiratory conditions among theater workers exposed to aerosolized propylene glycol used in the generation of artificial fog. 120 Nicotine salts used in pod based vape pen solutions, including Juul, have been found to penetrate the cell membrane and have cytotoxic effects. 121
The myriad available vape pen flavors correlate with an expansive list of chemical compounds with potential adverse respiratory effects. Flavorants have come under increased scrutiny in recent years and have been found to contribute to the majority of aldehyde production during vape aerosol production. 122 Compounds such as cinnamaldehyde, 123 124 2,5-dimethylpyrazine (chocolate flavoring), 125 and 2,3-pentanedione 126 are common flavor additives and have been found to contribute to airway inflammation and altered immunological responses. The flavorant diacetyl garnered particular attention after it was identified on mass spectrometry in most vape solutions tested. 127 Diacetyl is most widely associated with an outbreak of diacetyl associated bronchiolitis obliterans (“popcorn lung”) among workers at a microwave popcorn plant in 2002. 128 Identification of diacetyl in vape solutions raises the possibility of development of a similar pattern of bronchiolitis obliterans among individuals who have chronic vape aerosol exposure to diacetyl-containing vape solutions. 129
Studies of vape aerosols have suggested multiple pro-inflammatory effects on the respiratory system. This includes increased airway resistance, 130 impaired response to infection, 131 and impaired mucociliary clearance. 132 Vape aerosols have further been found to induce oxidative stress in lung epithelial cells, 133 and to both induce DNA damage and impair DNA repair, consistent with a potential carcinogenic effect. 134 Mice chronically exposed to vape aerosols developed increased airway hyper-reactivity and parenchymal changes consistent with chronic obstructive pulmonary disease. 135 Human studies have been more limited, but reveal increased airway edema and friability among vape pen users, as well as altered gene transcription and decreased innate immunity. 136 137 138 Upregulation of neutrophil elastase and matrix metalloproteases among vape users suggests increased proteolysis, potentially putting those patients at risk of chronic respiratory conditions. 139
THC-containing products
Of particular interest during the 2019 EVALI outbreak was the high prevalence of THC use among EVALI cases, 19 raising questions about a novel mechanism of lung injury specific to THC-containing vape solutions. These solutions differ from conventional nicotine based products because of the need for a carrier capable of emulsifying the lipid based THC component. In this context, additional vape solution ingredients rose to attention as potential culprits—namely, THC itself, which has been found to degrade to methacrolein and benzene, 140 as well as vitamin E acetate which was found to be a common oil based diluent. 141
Vitamin E acetate has garnered increasing attention as a potential culprit in the pathophysiology of the EVALI outbreak. Vitamin E acetate was found in 94% of BAL samples collected from EVALI patients, compared with none identified in unaffected vape pen users. 96 Thermal degradation of vitamin E acetate under conditions similar to those in THC vape pens has shown production of ketene, alkene, and benzene, which may mediate epithelial lung injury when inhaled. 39 Previous work had found that vitamin E acetate impairs pulmonary surfactant function, 142 and subsequent studies have shown a dose dependent adverse effect on lung parenchyma by vitamin E acetate, including toxicity to type II pneumocytes, and increased inflammatory cytokines. 143 Mice exposed to aerosols containing vitamin E acetate developed LLM and increased alveolar protein content, suggesting epithelial injury. 140 143
The pathophysiological insult underlying vaping related lung injury may be multitudinous, including potentially compound effects from multiple ingredients comprising a vape aerosol. The heterogeneity of available vape solutions on the market further complicates efforts to pinpoint particular elements of the vape aerosol that may be pathogenic, as no two users are likely to be exposed to the same combination of vape solution products. Further, vape users may be exposed to vape solutions containing terpenes, medium chain triglycerides, or coconut oil, the effects of which on respiratory epithelium remain under investigation. 144
Lipid laden macrophages
Lipid laden alveolar macrophages have risen to prominence as potential markers of vaping related lung injury. Alveolar macrophages describe a scavenger white blood cell responsible for clearing alveolar spaces of particulate matter and modulating the inflammatory response in the lung parenchyma. 145 LLM describe alveolar macrophages that have phagocytosed fat containing deposits, as seen on Oil Red O staining, and have been described in a wide variety of pulmonary conditions, including aspiration, lipoid pneumonia, organizing pneumonia, and medication induced pneumonitis. 146 147 During the EVALI outbreak, LLM were identified in the alveolar spaces of affected patients, both in the BAL fluid and on both transbronchial and surgical lung biopsies. 148 149 Of 52 EVALI cases reported in the literature who underwent BAL, LLM were identified in over 80%. 19 100 101 148 149 150 151 152 153 Accordingly, attention turned to LLM as not only a potential marker of lung injury in EVALI, but as a possible contributor to lung inflammation itself. This concern was compounded by the frequent reported use of oil based THC vape products among EVALI patients, raising the possibility of lipid deposits in the alveolus resulting from inhalation of THC-containing vape aerosols. 154 The combination of LLM, acute lung injury, and inhalational exposure to an oil based substance raised the concern for exogenous lipoid pneumonia. 152 153 However, further evaluation of the radiographic and histopathologic findings failed to identify cardinal features that would support a diagnosis of exogenous lipoid pneumonia—namely, low attenuation areas on CT imaging and foreign body giant cells on histopathology. 155 156 However, differences in the particle size and distribution between vape aerosol exposure and traditional causes of lipoid pneumonia (ie, aspiration of a large volume of an oil-containing substance), could reasonably lead to differences in radiographic appearance, although this would not account for the lack of characteristic histopathologic features on biopsy that would support a diagnosis of lipoid pneumonia.
Recent work suggests that LLM reflect a non-specific marker of vaping, rather than a marker of lung injury. One study found that LLM were not unique to EVALI and could be identified in healthy vape pen users, as well as conventional cigarette smokers, but not in never smokers. 157 Interestingly, this work showed increased cytokines IL-4 and IL-10 among healthy vape users, suggesting that cigarette and vape pen use are associated with a pro-inflammatory state in the lung. 157 An alternative theory supports LLM presence reflecting macrophage clearance of intra-alveolar cell debris rather than exogenous lipid exposure. 149 150 Such a pattern would be in keeping with the role of alveolar macrophages as modulating the inflammatory response in the lung parenchyma. 158 Taken together, available data would support LLM serving as a non-specific marker of vape product use, rather than playing a direct role in vaping related lung injury pathogenesis. 102
Clinical aspects
A high index of suspicion is required in establishing a diagnosis of vaping related lung injury, and a general approach is summarized in figure 3 . Clinicians may consider the diagnosis when faced with a patient with new respiratory symptoms in the context of vape pen use, without an alternative cause to account for their symptoms. Suspicion should be especially high if respiratory complaints are coupled with constitutional and gastrointestinal symptoms. Patients may present with non-specific markers indicative of an ongoing inflammatory process: fevers, leukocytosis, elevated C reactive protein, or elevated erythrocyte sedimentation rate. 19

Flowchart outlining the procedure for diagnosing a vaping related lung injury
Vaping related lung injury is a diagnosis of exclusion. Chest imaging via radiograph or CT may identify a variety of patterns, although diffuse ground glass opacities remain the most common radiographic finding. Generally, patients with an abnormal chest radiograph should undergo a chest CT for further evaluation of possible vaping related lung injury.
Exclusion of infectious causes is recommended. Testing should include evaluation for bacterial and viral causes of pneumonia, as deemed appropriate by clinical judgment and epidemiological data. Exclusion of common viral causes of pneumonia is imperative, particularly influenza and SARS-CoV-2. Bronchoscopy with BAL should be considered on a case-by-case basis for those with more severe disease and may be helpful to identify patients with vaping mediated eosinophilic lung injury. Further, lung biopsy may be beneficial to exclude alternative causes of lung injury in severe cases. 92
No definitive therapy has been identified for the treatment of vaping related lung injury, and data are limited to case reports and public health guidance on the topic. Management includes supportive care and strong consideration for systemic corticosteroids for severe cases of vaping related lung injury. CDC guidance encourages consideration of systemic corticosteroids for patients requiring admission to hospital, or those with higher risk factors for adverse outcomes, including age over 50, immunosuppressed status, or underlying cardiopulmonary disease. 100 Further, given case reports of vaping mediated acute eosinophilic pneumonia, steroids should be implemented in those patients who have undergone a confirmatory BAL. 77 79
Additional therapeutic options include empiric antibiotics and/or antivirals, depending on the clinical scenario. For patients requiring admission to hospital, prompt subspecialty consultation with a pulmonologist can help guide management. Outpatient follow-up with chest imaging and spirometry is recommended, as well as referral to a pulmonologist. Counseling regarding vaping cessation is also a core component in the post-discharge care for this patient population. Interventions specific to vaping cessation remain under investigation; however, literature supports the use of behavioral counseling and/or pharmacotherapy to support nicotine cessation efforts. 66
Health outcomes among vape pen users
Health outcomes among chronic vape pen users remains an open question. To date, no large scale prospective cohort studies exist that can establish a causal link between vape use and adverse respiratory outcomes. One small scale prospective cohort study did not identify any spirometric or radiographic changes among vape pen users over a 3.5 year period. 159 Given that vaping remains a relatively novel phenomenon, many users will have a less than 10 “pack year” history of vape pen use, arguably too brief an exposure period to reflect the potential harmful nature of chronic vaping. Studies encompassing a longer period of observation of vape pen users have not yet taken place, although advances in electronic medical record (EMR) data collection on vaping habits make such work within reach.
Current understanding of the health effects of vaping is largely limited to case reports of acute lung injury, and health surveys drawing associations between vaping exposure and patient reported outcomes. Within these limitations, however, early work suggests a correlation between vape pen use and poorer cardiopulmonary outcomes. Survey studies of teens who regularly vape found increased frequencies of respiratory symptoms, including productive cough, that were independent of smoking status. 160 161 These findings were corroborated in a survey series identifying more severe asthma symptoms and more days of school missed owing to asthma among vape pen users, regardless of cigarette smoking status. 162 163 164 Studies among adults have shown a similar pattern, with increased prevalence of chronic respiratory conditions (ie, asthma or chronic obstructive pulmonary disease) among vape pen users, 165 166 and higher risk of myocardial infarction and stroke, but lower risk of diabetes. 167
The effects of vaping on lung function as determined by spirometric studies are more varied. Reported studies have assessed lung function after a brief exposure to vape aerosols, varying from 5-60 minutes in duration, and no longer term observational cohort studies exist. While some studies have shown increased airway resistance after vaping exposure, 130 168 169 others have shown no change in lung function. 137 170 171 The cumulative exposure of habitual vape pen users to vape aerosols is much longer than the period evaluated in these studies, and the impact of vaping on longer term respiratory heath remains to be seen. Recent work evaluating ventilation-perfusion matching among chronic vapers compared with healthy controls found increased ventilation-perfusion mismatch, despite normal spirometry in both groups. 172 Such work reinforces the notion that changes in spirometry are a feature of more advanced airways disease, and early studies, although inconsistent, may foreshadow future respiratory impairment in chronic vapers.
Covid-19 and vaping
The covid-19 pandemic brought renewed attention to the potential health impacts of vaping. Studies investigating the role of vaping in covid-19 prevalence and outcomes have been limited by the small size of the populations studied and results have been inconsistent. Early work noted a geographic association in the US between vaping prevalence and covid-19 cases, 173 and a subsequent survey study found that a covid-19 diagnosis was five times more likely among teens who had ever vaped. 174 In contrast, a UK survey study found no association between vaping status and covid-19 infection rates, although captured a much smaller population of vape pen users. 175 Reports of nicotine use upregulating the angiotensin converting enzyme 2 (ACE-2) receptor, 176 which serves as the binding site for SARS-CoV-2 entry, raised the possibility of increased susceptibility to covid-19 among chronic nicotine vape pen users. 177 178 Further, vape use associated with sharing devices and frequent touching of the mouth and face were posited as potential confounders contributing to increased prevalence of covid-19 in this population. 179
Covid-19 outcomes among chronic vape pen users remain an open question. While smoking has been associated with progression to more severe infections, 180 181 no investigation has been performed to date among vaping cohorts. The young average age of chronic vape pen users may prove a protective factor, as risk of severe covid-19 infection has been shown to increase with age. 182 Regardless, a prudent recommendation remains to abstain from vaping to mitigate risk of progression to severe covid-19 infection. 183
Increased awareness of respiratory health brought about by covid-19 and EVALI is galvanizing the changing patterns in vape pen use. 184 Survey studies have consistently shown trends toward decreasing use among adolescents and young adults. 174 185 186 In one study, up to two thirds of participants endorsed decreasing or quitting vaping owing to a combination of factors including difficulty purchasing vape products during the pandemic, concerns about vaping effects on lung health, and difficulty concealing vape use while living with family. 174 Such results are reflected in nationwide trends that show halting growth in vaping use among high school students. 8 These trends are encouraging in that public health interventions countering nicotine use among teens may be meeting some measure of success.
Clinical impact—collecting and recording a vaping history
Vaping history in electronic medical records.
Efforts to prevent, diagnose, and treat vaping related lung injury begin with the ability of our healthcare system to identify vape users. Since vaping related lung injury remains a diagnosis of exclusion, clinicians must have a high index of suspicion when confronted with idiopathic lung injury in a patient with vaping exposure. Unlike cigarette use, vape pen use is not built into most EMR systems, and is not included in meaningful use criteria for EMRs. 187 Retrospective analysis of outpatient visits showed that a vaping history was collected in less than 0.1% of patients in 2015, 188 although this number has been increasing. 189 190 In part augmented by EMR frameworks that prompt collection of data on vaping history, more recent estimates indicate that a vaping history is being collected in up to 6% of patients. 191 Compared with the widespread use of vaping, particularly among adolescent and young adult populations, this number remains low. Considering generational trends in nicotine use, vaping will likely eventually overcome cigarettes as the most common mode of nicotine use, raising the importance of collecting a vaping related history. Further, EMR integration of vaping history is imperative to allow for retrospective, large scale analyses of vape exposure on longitudinal health outcomes at a population level.
Practical considerations—gathering a vaping history
As vaping becomes more common, the clinician’s ability to accurately collect a vaping history and identify patients who may benefit from nicotine cessation programs becomes more important. Reassuringly, gathering a vaping history is not dissimilar to asking about smoking and use of other tobacco products, and is summarized in box 2 . Collecting a vaping history is of particular importance for providers caring for adolescents and young adults who are among the highest risk demographics for vape pen use. Adolescents and young adults may be reluctant to share their vaping history, particularly if they are using THC-containing or CBD-containing vape solutions. Familiarity with vernacular terms to describe vaping, assuming a non-judgmental approach, and asking parents or guardians to step away during history taking will help to break down these barriers. 192
Practical guide to collecting a vaping history
Ask with empathy.
Young adults may be reluctant to share history of vaping use. Familiarity with vaping terminology, asking in a non-judgmental manner, and asking in a confidential space may help.
Ask what they are vaping
Vape products— vape pens commonly contain nicotine or an alternative active ingredient, such as THC or CBD. Providers may also inquire about flavorants, or other vape solution additives, that their patient is consuming, particularly if vaping related lung injury is suspected.
Source— ask where they source their product from. Sources may include commercially available products, third party distributors, or friends or local contacts.
Ask how they are vaping
Device— What style of device are they using?
Frequency— How many times a day do they use their vape pen (with frequent use considered >5 times a day)? Alternatively, providers may inquire how long it takes to deplete a vape solution cartridge (with use of one or more pods a day considered heavy use).
Nicotine concentration— For individuals consuming nicotine-containing products, clinicians may inquire about concentration and frequency of use, as this may allow for development of a nicotine replacement therapy plan.
Ask about other inhaled products
Clinicians should ask patients who vape about use of other inhaled products, particularly cigarettes. Further, clinicians may ask about use of water pipes, heat-not-burn devices, THC-containing products, or dabbing.
The following provides a practical guide on considerations when collecting a vaping history. Of note, collecting a partial history is preferable to no history at all, and simply recording whether a patient is vaping or not adds valuable information to the medical record.
Vape use— age at time of vaping onset and frequency of vape pen use. Vape pen use >5 times a day would be considered frequent. Alternatively, clinicians may inquire how long it takes to deplete a vape solution pod (use of one or more pods a day would be considered heavy use), or how frequently users are refilling their vape pens for refillable models.
Vape products— given significant variation in vape solutions available on the market, and variable risk profiles of the multitude of additives, inquiring as to which products a patient is using may add useful information. Further, clinicians may inquire about use of nicotine versus THC-containing vape solutions, and whether said products are commercially available or are customized by third party sellers.
Concurrent smoking— simultaneous use of multiple inhaled products is common among vape users, including concurrent use of conventional cigarettes, water pipes, heat-not-burn devices, and THC-containing or CBD-containing products. Among those using marijuana products, gathering a history regarding the type of product use, the device, and the modality of aerosol generation may be warranted. Gathering such detailed information may be challenging in the face of rapidly evolving product availability and changing popular terminology. Lastly, clinicians may wish to inquire about “dabbing”—the practice of inhaling heated butane hash oil, a concentrated THC wax—which may also be associated with lung injury. 193
Future directions
Our understanding of the effects of vaping on respiratory health is in its early stages and multiple trials are under way. Future work requires enhanced understanding of the effects of vape aerosols on lung biology, such as ongoing investigations into biomarkers of oxidative stress and inflammation among vape users (clinicaltrials.gov NCT03823885 ). Additional studies seek to elucidate the relation between vape aerosol exposure and cardiopulmonary outcomes among vape pen users ( NCT03863509 , NCT05199480 ), while an ongoing prospective cohort study will allow for longitudinal assessment of airway reactivity and spirometric changes among chronic vape pen users ( NCT04395274 ).
Public health and policy interventions are vital in supporting both our understanding of vaping on respiratory health and curbing the vaping epidemic among teens. Ongoing, large scale randomized controlled studies seek to assess the impact of the FDA’s “The Real Cost” advertisement campaign for vaping prevention ( NCT04836455 ) and another trial is assessing the impact of a vaping prevention curriculum among adolescents ( NCT04843501 ). Current trials are seeking to understand the potential for various therapies as tools for vaping cessation, including nicotine patches ( NCT04974580 ), varenicline ( NCT04602494 ), and text message intervention ( NCT04919590 ).
Finally, evaluation of vaping as a potential tool for harm reduction among current cigarette smokers is undergoing further evaluation ( NCT03235505 ), which will add to the body of work and eventually lead to clear policy guidance.
Several guidelines on the management of vaping related lung injury have been published and are summarized in table 1 . 194 195 196 Given the relatively small number of cases, the fact that vaping related lung injury remains a newer clinical entity, and the lack of clinical trials on the topic, guideline recommendations reflect best practices and expert opinion. Further, published guidelines focus on the diagnosis and management of EVALI, and no guidelines exist to date for the management of vaping related lung injury more generally.
Summary of clinical guidelines
- View inline
Conclusions
Vaping has grown in popularity internationally over the past decade, in part propelled by innovations in vape pen design and nicotine flavoring. Teens and young adults have seen the biggest uptake in use of vape pens, which have superseded conventional cigarettes as the preferred modality of nicotine consumption. Despite their widespread popularity, relatively little is known about the potential effects of chronic vaping on the respiratory system, and a growing body of literature supports the notion that vaping is not without risk. The 2019 EVALI outbreak highlighted the potential harms of vaping, and the consequences of long term use remain unknown.
Discussions regarding the potential harms of vaping are reminiscent of scientific debates about the health effects of cigarette use in the 1940s. Interesting parallels persist, including the fact that only a minority of conventional cigarette users develop acute lung injury, yet the health impact of sustained, longitudinal cigarette use is unquestioned. The true impact of vaping on respiratory health will manifest over the coming decades, but in the interval a prudent and time tested recommendation remains to abstain from consumption of inhaled nicotine and other products.
Questions for future research
How does chronic vape aerosol exposure affect respiratory health?
Does use of vape pens affect respiratory physiology (airway resistance, V/Q matching, etc) in those with underlying lung disease?
What is the role for vape pen use in promoting smoking cessation?
What is the significance of pulmonary alveolar macrophages in the pathophysiology of vaping related lung injury?
Are particular populations more susceptible to vaping related lung injury (ie, by sex, demographic, underlying comorbidity, or age)?
Series explanation: State of the Art Reviews are commissioned on the basis of their relevance to academics and specialists in the US and internationally. For this reason they are written predominantly by US authors
Contributors: AJ conceived of, researched, and wrote the piece. She is the guarantor.
Competing interests: I have read and understood the BMJ policy on declaration of interests and declare the following interests: AJ receives consulting fees from DawnLight, Inc for work unrelated to this piece.
Patient involvement: No patients were directly involved in the creation of this article.
Provenance and peer review: Commissioned; externally peer reviewed.
- ↵ US Department of Health and Human Services. The health consequences of smoking—50 years of progress: a report of the Surgeon General. 2014. doi: 10.1037/e510072014-001 .
- Cornelius ME ,
- Loretan CG ,
- Marshall TR
- Fetterman JL ,
- Benjamin EJ ,
- Barrington-Trimis JL ,
- Leventhal AM ,
- Cullen KA ,
- Gentzke AS ,
- Sawdey MD ,
- ↵ Centers for Disease Control and Prevention. Surgeon General’s Advisory on E-cigarette Use Among Youth. 2018. https://www.cdc.gov/tobacco/basic_information/e-cigarettes/surgeon-general-advisory/index.html
- Leventhal A ,
- Johnston L ,
- O’Malley PM ,
- Patrick ME ,
- Barrington-Trimis J
- ↵ Foundation for a Smoke-Free World https://www.smokefreeworld.org/published_reports/
- Kaisar MA ,
- Calfee CS ,
- Matthay MA ,
- ↵ Royal College of Physicians (London) & Tobacco Advisory Group. Nicotine without smoke: tobacco harm reduction: a report. 2016. https://www.rcplondon.ac.uk/projects/outputs/nicotine-without-smoke-tobacco-harm-reduction
- ↵ National Academies of Sciences, Engineering, and Medicine. Public health consequences of e-cigarettes. 2018. doi: 10.17226/24952 OpenUrl CrossRef
- Manigrasso M ,
- Buonanno G ,
- Stabile L ,
- Agnihotri R
- LeBouf RF ,
- Koutrakis P ,
- Christiani DC
- Perrine CG ,
- Pickens CM ,
- Boehmer TK ,
- Lung Injury Response Epidemiology/Surveillance Group
- Layden JE ,
- Esposito S ,
- Spindle TR ,
- Eissenberg T ,
- Kendler KS ,
- McCabe SE ,
- ↵ Joseph R. Electric vaporizer. 1930.
- ↵ Gilbert HA. Smokeless non-tobacco cigarette. 1965.
- ↵ An Interview With A 1970’s Vaping Pioneer. Ashtray Blog. 2015 . https://www.ecigarettedirect.co.uk/ashtray-blog/2014/06/favor-cigarette-interview-dr-norman-jacobson.html (2014).
- Benowitz N ,
- ↵ National Academies of Sciences, Engineering, and Medicine, Health and Medicine Division, Board on Population Health and Public Health Practice, & Committee on the Review of the Health Effects of Electronic Nicotine Delivery Systems. Public Health Consequences of E-Cigarettes . (National Academies Press (US), 2018).
- ↵ Tolentino J. The Promise of Vaping and the Rise of Juul. The New Yorker . 2018 https://www.newyorker.com/magazine/2018/05/14/the-promise-of-vaping-and-the-rise-of-juul
- ↵ Bowen A, Xing C. Nicotine salt formulations for aerosol devices and methods thereof. 2014.
- Madden DR ,
- McConnell R ,
- Gammon DG ,
- Marynak KL ,
- ↵ Jackler RK, Chau C, Getachew BD, et al. JUUL Advertising Over its First Three Years on the Market. Stanford Research into the Impact of Tobacco Advertising, Stanford University School of Medicine. 2019. https://tobacco-img.stanford.edu/wp-content/uploads/2021/07/21231836/JUUL_Marketing_Stanford.pdf
- Prochaska JJ ,
- ↵ Richtel M, Kaplan S. Juul May Get Billions in Deal With One of World’s Largest Tobacco Companies. The New York Times . 2018.
- ↵ Truth Initiative. Vaping Lingo Dictionary: A guide to popular terms and devices. 2020. https://truthinitiative.org/research-resources/emerging-tobacco-products/vaping-lingo-dictionary
- Williams M ,
- Pepper JK ,
- MacMonegle AJ ,
- Nonnemaker JM
- ↵ The Physics of Vaporization. Jupiter Research. 2020. https://www.jupiterresearch.com/physics-of-vaporization/
- Bonnevie E ,
- ↵ National Center for Chronic Disease Prevention and Health Promotion (US) Office on Smoking and Health. E-Cigarette Use Among Youth and Young Adults: A Report of the Surgeon General. 2016. https://www.ncbi.nlm.nih.gov/books/NBK538680/
- Trivers KF ,
- Phillips E ,
- Stefanac S ,
- Sandner I ,
- Grabovac I ,
- ↵ Knowledge-Action-Change. Burning Issues: The Global State of Tobacco Harm Reduction 2020. 2020. https://gsthr.org/resources/item/burning-issues-global-state-tobacco-harm-reduction-2020
- Creamer MR ,
- Park-Lee E ,
- Gorukanti A ,
- Delucchi K ,
- Fisher-Travis R ,
- Halpern-Felsher B
- Amrock SM ,
- ↵ Buy JUUL Products | Shop All JUULpods, JUUL Devices, and Accessories | JUUL. https://www.juul.com/shop
- Schiff SJ ,
- Kechter A ,
- Simpson KA ,
- Ceasar RC ,
- Braymiller JL ,
- Barrington-Trimis JL
- Moustafa AF ,
- Rodriguez D ,
- Audrain-McGovern J
- Berhane K ,
- Stjepanović D ,
- Hitchman SC ,
- Bakolis I ,
- Plurphanswat N
- Warner KE ,
- Cummings KM ,
- ↵ FDA finalizes enforcement policy on unauthorized flavored cartridge-based e-cigarettes that appeal to children, including fruit and mint. FDA . 2020 . https://www.fda.gov/news-events/press-announcements/fda-finalizes-enforcement-policy-unauthorized-flavored-cartridge-based-e-cigarettes-appeal-children
- ↵ Henderson, E. E-cigarettes: an evidence update. 113.
- Hartmann-Boyce J ,
- McRobbie H ,
- Lindson N ,
- Phillips-Waller A ,
- ↵ Centers for Disease Control and Prevention. Electronic Cigarettes. 2020. https://www.cdc.gov/tobacco/basic_information/e-cigarettes/index.htm l
- Patnode CD ,
- Henderson JT ,
- Thompson JH ,
- Senger CA ,
- Fortmann SP ,
- Whitlock EP
- Kmietowicz Z
- ↵ World Health Organization. E-cigarettes are harmful to health. 2020. https://www.who.int/news/item/05-02-2020-e-cigarettes-are-harmful-to-health
- Lachireddy K ,
- Sleiman M ,
- Montesinos VN ,
- Kalkhoran S ,
- Filion KB ,
- Kimmelman J ,
- Eisenberg MJ
- McCauley L ,
- Aoshiba K ,
- Nakamura H ,
- Wiggins A ,
- Hudspath C ,
- Kisling A ,
- Hostler DC ,
- Sommerfeld CG ,
- Weiner DJ ,
- Mantilla RD ,
- Darnell RT ,
- Khateeb F ,
- Agustin M ,
- Yamamoto M ,
- Cabrera F ,
- ↵ Long. Diffuse Alveolar Hemorrhage Due to Electronic Cigarette Use | A54. CRITICAL CARE CASE REPORTS: ACUTE HYPOXEMIC RESPIRATORY FAILURE/ARDS. https://www.atsjournals.org/doi/abs/10.1164/ajrccm-conference.2016.193.1_MeetingAbstracts.A1862
- Ring Madsen L ,
- Vinther Krarup NH ,
- Bergmann TK ,
- Bradford LE ,
- Rebuli ME ,
- Jaspers I ,
- Clement KC ,
- Loughlin CE
- Bonilla A ,
- Alamro SM ,
- Bassett RA ,
- Osterhoudt K ,
- Slaughter J ,
- ↵ Health CO. on S. and. Smoking and Tobacco Use; Electronic Cigarettes. https://www.cdc.gov/tobacco/basic_information/e-cigarettes/severe-lung-disease.html (2019).
- ↵ For State, Local, Territorial, and Tribal Health Departments | Electronic Cigarettes | Smoking & Tobacco Use | CDC. https://www.cdc.gov/tobacco/basic_information/e-cigarettes/severe-lung-disease/health-departments/index.html (2019).
- ↵ 2019 Lung Injury Surveillance Primary Case Definitions. 2.
- Callahan SJ ,
- Collingridge DS ,
- Armatas C ,
- Heinzerling A ,
- Blount BC ,
- Karwowski MP ,
- Shields PG ,
- Lung Injury Response Laboratory Working Group
- ↵ Government of Canada. Vaping-associated lung illness. 2020. https://www.canada.ca/en/public-health/services/diseases/vaping-pulmonary-illness.html (2020).
- Marlière C ,
- De Greef J ,
- Casanova GS ,
- Blagev DP ,
- Guidry DW ,
- Grissom CK ,
- Werner AK ,
- Koumans EH ,
- Chatham-Stephens K ,
- Lung Injury Response Mortality Working Group
- Tsirilakis K ,
- Yenduri NJS ,
- Guillerman RP ,
- Anderson B ,
- Serajeddini H ,
- Knipping D ,
- Brasky TM ,
- Pisinger C ,
- Godtfredsen N ,
- Jensen RP ,
- Pankow JF ,
- Strongin RM ,
- Lechasseur A ,
- Altmejd S ,
- Turgeon N ,
- Goessler W ,
- Chaumont M ,
- van de Borne P ,
- Bernard A ,
- Kosmider L ,
- Sobczak A ,
- Aldridge K ,
- Afshar-Mohajer N ,
- Koehler K ,
- Varughese S ,
- Teschke K ,
- van Netten C ,
- Beyazcicek O ,
- Onyenwoke RU ,
- Khlystov A ,
- Samburova V
- Lavrich KS ,
- van Heusden CA ,
- Lazarowski ER ,
- Carson JL ,
- Pawlak EA ,
- Lackey JT ,
- Sherwood CL ,
- O’Sullivan M ,
- Vallarino J ,
- Flanigan SS ,
- LeBlanc M ,
- Kullman G ,
- Simoes EJ ,
- Wambui DW ,
- Vardavas CI ,
- Anagnostopoulos N ,
- Kougias M ,
- Evangelopoulou V ,
- Connolly GN ,
- Behrakis PK
- Sussan TE ,
- Gajghate S ,
- Thimmulappa RK ,
- Hossain E ,
- Perveen Z ,
- Lerner CA ,
- Sundar IK ,
- Garcia-Arcos I ,
- Geraghty P ,
- Baumlin N ,
- Coakley RC ,
- Mascenik T ,
- Staudt MR ,
- Hollmann C ,
- Radicioni G ,
- Coakley RD ,
- Kalathil SG ,
- Bogner PN ,
- Goniewicz ML ,
- Thanavala YM
- Massey JB ,
- Matsumoto S ,
- Traber MG ,
- Ranpara A ,
- Stefaniak AB ,
- Williams K ,
- Fernandez E ,
- Basset-Léobon C ,
- Lacoste-Collin L ,
- Courtade-Saïdi M
- Boland JM ,
- Maddock SD ,
- Cirulis MM ,
- Tazelaar HD ,
- Mukhopadhyay S ,
- Dammert P ,
- Kalininskiy A ,
- Davidson K ,
- Brancato A ,
- Heetderks P ,
- Dicpinigaitis PV ,
- Trachuk P ,
- Suhrland MJ
- Khilnani GC
- Simmons A ,
- Freudenheim JL ,
- Hussell T ,
- Cibella F ,
- Caponnetto P ,
- Schweitzer RJ ,
- Williams RJ ,
- Vindhyal MR ,
- Munguti C ,
- Vindhyal S ,
- Lappas AS ,
- Tzortzi AS ,
- Konstantinidi EM ,
- Antoniewicz L ,
- Brynedal A ,
- Lundbäck M ,
- Ferrari M ,
- Boulay MÈ ,
- Boulet LP ,
- Morissette MC
- Kizhakke Puliyakote AS ,
- Elliott AR ,
- Anderson KM ,
- Crotty Alexander LE ,
- Jackson SE ,
- McAlinden KD ,
- McKelvey K ,
- Patanavanich R ,
- NVSS - Provisional Death Counts for COVID-19 - Executive Summary
- Sokolovsky AW ,
- Hertel AW ,
- Micalizzi L ,
- Klemperer EM ,
- Peasley-Miklus C ,
- Villanti AC
- Henricks WH
- Young-Wolff KC ,
- Klebaner D ,
- Mowery DL ,
- Don’t Forget to Ask
- Stephens D ,
- Siegel DA ,
- Jatlaoui TC ,
- Lung Injury Response Clinical Working Group ,
- Ramalingam SS ,
- Schuurmans MM
Featured Topics
Featured series.
A series of random questions answered by Harvard experts.
Explore the Gazette
Read the latest.
Study pinpoints optimal timing for RSV vaccine during pregnancy

Cutting through the fog of long COVID
Warning for younger women: Be vigilant on breast cancer risk

Studies show that about 9 percent of the population and nearly 28 percent of high school students are e-cigarette users.
Diego Cervo/iStock by Getty Images
Restricted airways, scarred lung tissue found among vapers
MGH News and Public Affairs
Small study looks at chronic e-cigarette users, seeing partial improvement once they stop
Chronic use of e-cigarettes, commonly known as vaping, can result in small airway obstruction and asthma-like symptoms, according to researchers at Harvard-affiliated Massachusetts General Hospital.
More like this

Teen vaping rising fast, research says

Survey of oncologists finds knowledge gap on medical marijuana

Chemical flavorings found in e-cigarettes linked to respiratory disease
In the first study to microscopically evaluate the pulmonary tissue of e-cigarette users for chronic disease, the team found in a small sample of patients fibrosis and damage in the small airways, similar to the chemical inhalation damage to the lungs typically seen in soldiers returning from overseas conflicts who had inhaled mustard or similar types of noxious gases. The study was published in New England Journal of Medicine Evidence .
“All four individuals we studied had injury localized to the same anatomic location within the lung, manifesting as small airway-centered fibrosis with constrictive bronchiolitis, which was attributed to vaping after thorough clinical evaluations excluded other possible causes,” says lead author Lida Hariri, an associate professor of pathology at Harvard Medical School and a pathologist and physician investigator at MGH. “We also observed that when patients ceased vaping, they had a partial reversal of the condition over one to four years, though not complete due to residual scarring in the lung tissue.”
A huge increase in vaping, particularly among young adults and adolescents, has occurred in the United States, with studies showing about 9 percent of the population and nearly 28 percent of high school students are e-cigarette users. Unlike cigarette smoking, however, the long-term health risks of chronic vaping are largely unknown.
In order to determine the underlying pathophysiology of vaping-related symptoms, the MGH team examined a cohort of four patients, each with a three- to eight-year history of e-cigarette use and chronic lung disease. All patients underwent detailed clinical evaluation, including pulmonary function tests, high resolution chest imaging, and surgical lung biopsy. Constrictive bronchiolitis, or narrowing of the small airways due to fibrosis within the bronchiolar wall, was observed in each patient. So was significant overexpression of MUC5AC, a gel-forming protein in the mucus layer of the airway that has been seen in airway cell and sputum samples of individuals who vape. In addition, three of the four patients had evidence of mild emphysema consistent with their former combustible cigarette smoking history, though researchers concluded this was distinct from the findings of constrictive bronchiolitis seen in the patient cohort.
Because the same type of lung damage was observed in all patients, as well as partial improvement in symptoms after e-cigarette usage was stopped, researchers concluded that vaping was the most likely cause after thorough evaluation and exclusion of other possible causes. “Our investigation shows that chronic pathological abnormalities can occur in vaping exposure,” says senior author David Christiani, a professor of medicine at HMS and a physician investigator at Mass General Research Institute. “Physicians need to be informed by scientific evidence when advising patients about the potential harm of long-term vaping, and this work adds to a growing body of toxicological evidence that nicotine vaping exposures can harm the lung.”
A hopeful sign from the study was that three of the four patients showed improvements in their pulmonary function tests and high-resolution computed tomography (HRCT) chest imaging after they ceased vaping. “While there is growing evidence to show that vaping is a risky behavior with potential long-term health consequences for users,” says Hariri, “our research also suggests that quitting can be beneficial and help to reverse some of the disease.”
The study was funded by the National Institutes of Health.
Share this article
You might like.
Five weeks before giving birth best transfers maternal antibodies to the fetus, say researchers
Researchers say new AI tool sharpens diagnostic process, may help identify more people needing care

Pathologist explains the latest report from the American Cancer Society
U.S. fertility rates are tumbling, but some families still go big. Why?
It’s partly matter of faith. Economist examines choice to have large families in new book.
Did Trump election signal start of new political era?
Analysts weigh issues, strategies, media decisions at work in contest, suggest class may become dominant factor
Are optimists the realists?
Humanity is doing better than ever yet it often doesn’t seem that way. In podcast, experts make the case for fact-based hope.
- U.S. Department of Health & Human Services

- Virtual Tour
- Staff Directory
- En Español
You are here
News releases.
News Release
Wednesday, October 26, 2022
NIH-funded studies show damaging effects of vaping, smoking on blood vessels
Combining e-cigarettes with regular cigarettes may increase health risks.

Long-term use of electronic cigarettes, or vaping products, can significantly impair the function of the body’s blood vessels, increasing the risk for cardiovascular disease. Additionally, the use of both e-cigarettes and regular cigarettes may cause an even greater risk than the use of either of these products alone. These findings come from two new studies supported by the National Heart, Lung, and Blood Institute (NHLBI), part of the National Institutes of Health (NIH).
The findings, which appear today in the journal Arteriosclerosis, Thrombosis, and Vascular Biology , add to growing evidence that long-term use of e-cigarettes can harm a person’s health. Researchers have known for years that tobacco smoking can cause damage to blood vessels. However, the effects of e-cigarettes on cardiovascular health have been poorly understood. The two new studies – one on humans, the other on rats – aimed to change that.
“In our human study, we found that chronic e-cigarettes users had impaired blood vessel function, which may put them at increased risk for heart disease,” said Matthew L. Springer, Ph.D., a professor of medicine in the Division of Cardiology at the University of California in San Francisco, and leader of both studies. “It indicates that chronic users of e-cigarettes may experience a risk of vascular disease similar to that of chronic smokers.”
In this first study, Springer and his colleagues collected blood samples from a group of 120 volunteers that included those with long-term e-cigarette use, long-term cigarette smoking, and those who didn't use. The researchers defined long-term e-cigarette use as more than five times/week for more than three months and defined long-term cigarette use as smoking more than five cigarettes per day.
They then exposed each of the blood samples to cultured human blood vessel (endothelial) cells in the laboratory and measured the release of nitric oxide, a chemical marker used to evaluate proper functioning of endothelial cells. They also tested cell permeability, the ability of molecules to pass through a layer of cells to the other side. Too much permeability makes vessels leaky, which impairs function and increases the risk for cardiovascular disease.
The researchers found that blood from participants who used e-cigarettes and those who smoked caused a significantly greater decrease in nitric oxide production by the blood vessel cells than the blood of nonusers. Notably, the researchers found that blood from those who used e-cigarettes also caused more permeability in the blood vessel cells than the blood from both those who smoked cigarettes and nonusers. Blood from those that used e-cigarettes also caused a greater release of hydrogen peroxide by the blood vessel cells than the blood of the nonusers. Each of these three factors can contribute to impairment of blood vessel function in people who use e-cigarettes, the researchers said.
In addition, Springer and his team discovered that e-cigarettes had harmful cardiovascular effects in ways that were different from those caused by tobacco smoke. Specifically, they found that blood from people who smoked cigarettes had higher levels of certain circulating biomarkers of cardiovascular risks, and the blood people who used e-cigarettes had elevated levels of other circulating biomarkers of cardiovascular risks.
“These findings suggest that using the two products together, as many people do, could increase their health risks compared to using them individually,” Springer said. “We had not expected to see that.”
In the second study, the researchers tried to find out if there were specific components of cigarette smoke or e-cigarette vapor that were responsible for blood vessel damage. In studies using rats, they exposed the animals to various substances found in tobacco smoke or e-cigarettes. These included nicotine, menthol (a cigarette additive), the gases acrolein and acetaldehyde (two chemicals found in both tobacco smoke and e-cigarette vapors), and inert carbon nanoparticles to represent the particle-like nature of smoke and e-cigarette vapor.
Using special arterial flow measurements, the researchers demonstrated that blood vessel damage does not appear to be caused by a specific component of cigarette smoke or e-cigarette vapor. Instead, they said, it appears to be caused by airway irritation that triggers biological signals in the vagus nerve that somehow leads to blood vessel damage, possibly through an inflammatory process. The vagus is a long nerve extending from the brain that connects the airway to the rest of the nervous system and plays a key role in heart rate, breathing, and other functions. The researchers showed that detaching the nerve in rats prevented blood vessel damage caused by tobacco smoke, demonstrating its key role in this process.
“We were surprised to find that there was not a single component that you could remove to stop the damaging effect of smoke or vapors on the blood vessels,” Springer said. “As long as there’s an irritant in the airway, blood vessel function may be impaired.”
The finding has implications for efforts to regulate tobacco products and e-cigarettes, as it underscores how difficult it is to pinpoint any one ingredient in them that is responsible for blood vessel damage. “What I like to tell people is this: Just breathe clean air and avoid using these products,” Springer said.
Lisa Postow, Ph.D., an NHLBI program officer in NHLBI’s Division of Lung Diseases, agreed that the study results “provide further evidence that exposure to e-cigarettes could lead to harmful cardiovascular health effects.” She added that more data is needed to fully understand the health effects of e-cigarettes. The NIH and others are continuing to explore this area.
Research reported in the e-cigarette study was funded by NHLBI grants U54HL147127, P50HL120163, and R01HL120062 and the U.S. Food and Drug Administration Center for Tobacco Products (FDA CTP); and grant P50CA180890 from the National Cancer Institute at the NIH and FDA CTP. Research reported in the cigarette smoke/-vagal nerve study was supported by NHLBI grants R01HL120062 and U54HL147127 and FDA CTP and grant P50CA180890 from the National Cancer Institute at the NIH and FDA CTP. For additional funding details, please see the full journal articles.
About the National Heart, Lung, and Blood Institute (NHLBI): NHLBI is the global leader in conducting and supporting research in heart, lung, and blood diseases and sleep disorders that advances scientific knowledge, improves public health, and saves lives. For more information, visit www.nhlbi.nih.gov .
About the National Institutes of Health (NIH): NIH, the nation's medical research agency, includes 27 Institutes and Centers and is a component of the U.S. Department of Health and Human Services. NIH is the primary federal agency conducting and supporting basic, clinical, and translational medical research, and is investigating the causes, treatments, and cures for both common and rare diseases. For more information about NIH and its programs, visit www.nih.gov .
NIH…Turning Discovery Into Health ®
Chronic e-cigarette use impairs endothelial function on the physiological and cellular levels. Arteriosclerosis, Thrombosis, and Vascular Biology. DOI: 10.1161/ATVBAHA.121.317749
Impairment of Endothelial Function by Cigarette Smoke is not Caused by a Specific Smoke Constituent, but by Vagal Input from the Airway. Arteriosclerosis, Thrombosis, and Vascular Biology. DOI: 10.1161/ATVBAHA.122.318051
Connect with Us
- More Social Media from NIH
- Open access
- Published: 18 May 2021
An updated overview of e-cigarette impact on human health
- Patrice Marques ORCID: orcid.org/0000-0003-0465-1727 1 , 2 ,
- Laura Piqueras ORCID: orcid.org/0000-0001-8010-5168 1 , 2 , 3 &
- Maria-Jesus Sanz ORCID: orcid.org/0000-0002-8885-294X 1 , 2 , 3
Respiratory Research volume 22 , Article number: 151 ( 2021 ) Cite this article
429k Accesses
184 Citations
390 Altmetric
Metrics details
The electronic cigarette ( e-cigarette ), for many considered as a safe alternative to conventional cigarettes, has revolutionised the tobacco industry in the last decades. In e-cigarettes , tobacco combustion is replaced by e-liquid heating, leading some manufacturers to propose that e-cigarettes have less harmful respiratory effects than tobacco consumption. Other innovative features such as the adjustment of nicotine content and the choice of pleasant flavours have won over many users. Nevertheless, the safety of e-cigarette consumption and its potential as a smoking cessation method remain controversial due to limited evidence. Moreover, it has been reported that the heating process itself can lead to the formation of new decomposition compounds of questionable toxicity. Numerous in vivo and in vitro studies have been performed to better understand the impact of these new inhalable compounds on human health. Results of toxicological analyses suggest that e-cigarettes can be safer than conventional cigarettes, although harmful effects from short-term e-cigarette use have been described. Worryingly, the potential long-term effects of e-cigarette consumption have been scarcely investigated. In this review, we take stock of the main findings in this field and their consequences for human health including coronavirus disease 2019 (COVID-19).
Electronic nicotine dispensing systems (ENDS), commonly known as electronic cigarettes or e-cigarettes , have been popularly considered a less harmful alternative to conventional cigarette smoking since they first appeared on the market more than a decade ago. E-cigarettes are electronic devices, essentially consisting of a cartridge, filled with an e-liquid, a heating element/atomiser necessary to heat the e-liquid to create a vapour that can be inhaled through a mouthpiece, and a rechargeable battery (Fig. 1 ) [ 1 , 2 ]. Both the electronic devices and the different e-liquids are easily available in shops or online stores.
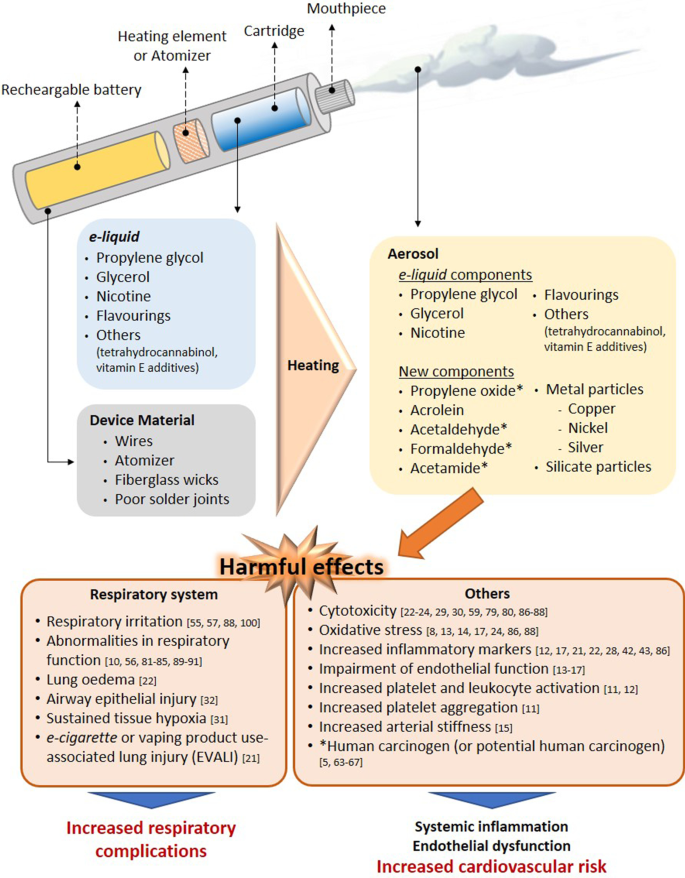
Effect of the heating process on aerosol composition. Main harmful effects documented. Several compounds detected in e-cigarette aerosols are not present in e-liquid s and the device material also seems to contribute to the presence of metal and silicate particles in the aerosols. The heating conditions especially on humectants, flavourings and the low-quality material used have been identified as the generator of the new compounds in aerosols. Some compounds generated from humectants (propylene glycol and glycerol) and flavourings, have been associated with clear airways impact, inflammation, impairment of cardiovascular function and toxicity. In addition, some of them are carcinogens or potential carcinogens
The e-liquid typically contains humectants and flavourings, with or without nicotine; once vapourised by the atomiser, the aerosol (vapour) provides a sensation similar to tobacco smoking, but purportedly without harmful effects [ 3 ]. However, it has been reported that the heating process can lead to the generation of new decomposition compounds that may be hazardous [ 4 , 5 ]. The levels of nicotine, which is the key addictive component of tobacco, can also vary between the commercially available e-liquids, and even nicotine-free options are available. For this particular reason, e-cigarettes are often viewed as a smoking cessation tool, given that those with nicotine can prevent smoking craving, yet this idea has not been fully demonstrated [ 2 , 6 , 7 ].
Because e-cigarettes are combustion-free, and because most of the damaging and well-known effects of tobacco are derived from this reaction, there is a common and widely spread assumption that e-cigarette consumption or “vaping” is safer than conventional cigarette smoking. However, are they risk-free? Is there sufficient toxicological data on all the components employed in e-liquids ? Do we really know the composition of the inhaled vapour during the heating process and its impact on health? Can e-cigarettes be used to curb tobacco use? Do their consumption impact on coronavirus disease 2019 (COVID-19)? In the present review, we have attempted to clarify these questions based on the existing scientific literature, and we have compiled new insights related with the toxicity derived from the use of these devices.

Effect of e-cigarette vapour versus conventional cigarette exposure: in vivo and in vitro effects
Numerous studies have been performed to evaluate the safety/toxicity of e-cigarette use both in vivo and in in vitro cell culture.
One of the first studies in humans involved the analysis of 9 volunteers that consumed e-cigarettes , with or without nicotine, in a ventilated room for 2 h [ 8 ]. Pollutants in indoor air, exhaled nitric oxide (NO) and urinary metabolite profiles were analysed. The results of this acute experiment revealed that e-cigarettes are not emission-free, and ultrafine particles formed from propylene glycol (PG) could be detected in the lungs. The study also suggested that the presence of nicotine in e-cigarettes increased the levels of NO exhaled from consumers and provoked marked airway inflammation; however, no differences were found in the levels of exhaled carbon monoxide (CO), an oxidative stress marker, before and after e-cigarette consumption [ 8 ]. A more recent human study detected significantly higher levels of metabolites of hazardous compounds including benzene, ethylene oxide, acrylonitrile, acrolein and acrylamide in the urine of adolescent dual users ( e-cigarettes and conventional tobacco consumers) than in adolescent e-cigarette -only users (Table 1 ) [ 9 ]. Moreover, the urine levels of metabolites of acrylonitrile, acrolein, propylene oxide, acrylamide and crotonaldehyde, all of which are detrimental for human health, were significantly higher in e-cigarette -only users than in non-smoker controls, reaching up to twice the registered values of those from non-smoker subjects (Table 1 ) [ 9 ]. In line with these observations, dysregulation of lung homeostasis has been documented in non-smokers subjected to acute inhalation of e-cigarette aerosols [ 10 ].
Little is known about the effect of vaping on the immune system. Interestingly, both traditional and e-cigarette consumption by non-smokers was found to provoke short-term effects on platelet function, increasing platelet activation (levels of soluble CD40 ligand and the adhesion molecule P-selectin) and platelet aggregation, although to a lesser extent with e-cigarettes [ 11 ]. As found with platelets, the exposure of neutrophils to e-cigarette aerosol resulted in increased CD11b and CD66b expression being both markers of neutrophil activation [ 12 ]. Additionally, increased oxidative stress, vascular endothelial damage, impaired endothelial function, and changes in vascular tone have all been reported in different human studies on vaping [ 13 , 14 , 15 , 16 , 17 ]. In this context, it is widely accepted that platelet and leukocyte activation as well as endothelial dysfunction are associated with atherogenesis and cardiovascular morbidity [ 18 , 19 ]. In line with these observations the potential association of daily e-cigarettes consumption and the increased risk of myocardial infarction remains controversial but benefits may occur when switching from tobacco to chronic e-cigarette use in blood pressure regulation, endothelial function and vascular stiffness (reviewed in [ 20 ]). Nevertheless, whether or not e-cigarette vaping has cardiovascular consequences requires further investigation.
More recently, in August 2019, the US Centers for Disease Control and Prevention (CDC) declared an outbreak of the e-cigarette or vaping product use-associated lung injury (EVALI) which caused several deaths in young population (reviewed in [ 20 ]). Indeed, computed tomography (CT scan) revealed local inflammation that impaired gas exchange caused by aerosolised oils from e-cigarettes [ 21 ]. However, most of the reported cases of lung injury were associated with use of e-cigarettes for tetrahydrocannabinol (THC) consumption as well as vitamin E additives [ 20 ] and not necessarily attributable to other e-cigarette components.
On the other hand, in a comparative study of mice subjected to either lab air, e-cigarette aerosol or cigarette smoke (CS) for 3 days (6 h-exposure per day), those exposed to e-cigarette aerosols showed significant increases in interleukin (IL)-6 but normal lung parenchyma with no evidence of apoptotic activity or elevations in IL-1β or tumour necrosis factor-α (TNFα) [ 22 ]. By contrast, animals exposed to CS showed lung inflammatory cell infiltration and elevations in inflammatory marker expression such as IL-6, IL-1β and TNFα [ 22 ]. Beyond airway disease, exposure to aerosols from e-liquids with or without nicotine has also been also associated with neurotoxicity in an early-life murine model [ 23 ].
Results from in vitro studies are in general agreement with the limited number of in vivo studies. For example, in an analysis using primary human umbilical vein endothelial cells (HUVEC) exposed to 11 commercially-available vapours, 5 were found to be acutely cytotoxic, and only 3 of those contained nicotine [ 24 ]. In addition, 5 of the 11 vapours tested (including 4 that were cytotoxic) reduced HUVEC proliferation and one of them increased the production of intracellular reactive oxygen species (ROS) [ 24 ]. Three of the most cytotoxic vapours—with effects similar to those of conventional high-nicotine CS extracts—also caused comparable morphological changes [ 24 ]. Endothelial cell migration is an important mechanism of vascular repair than can be disrupted in smokers due to endothelial dysfunction [ 25 , 26 ]. In a comparative study of CS and e-cigarette aerosols, Taylor et al . found that exposure of HUVEC to e-cigarette aqueous extracts for 20 h did not affect migration in a scratch wound assay [ 27 ], whereas equivalent cells exposed to CS extract showed a significant inhibition in migration that was concentration dependent [ 27 ].
In cultured human airway epithelial cells, both e-cigarette aerosol and CS extract induced IL-8/CXCL8 (neutrophil chemoattractant) release [ 28 ]. In contrast, while CS extract reduced epithelial barrier integrity (determined by the translocation of dextran from the apical to the basolateral side of the cell layer), e-cigarette aerosol did not, suggesting that only CS extract negatively affected host defence [ 28 ]. Moreover, Higham et al . also found that e-cigarette aerosol caused IL-8/CXCL8 and matrix metallopeptidase 9 (MMP-9) release together with enhanced activity of elastase from neutrophils [ 12 ] which might facilitate neutrophil migration to the site of inflammation [ 12 ].
In a comparative study, repeated exposure of human gingival fibroblasts to CS condensate or to nicotine-rich or nicotine-free e-vapour condensates led to alterations in morphology, suppression of proliferation and induction of apoptosis, with changes in all three parameters greater in cells exposed to CS condensate [ 29 ]. Likewise, both e-cigarette aerosol and CS extract increased cell death in adenocarcinomic human alveolar basal epithelial cells (A549 cells), and again the effect was more damaging with CS extract than with e-cigarette aerosol (detrimental effects found at 2 mg/mL of CS extract vs. 64 mg/mL of e-cigarette extract) [ 22 ], which is in agreement with another study examining battery output voltage and cytotoxicity [ 30 ].
All this evidence would suggest that e-cigarettes are potentially less harmful than conventional cigarettes (Fig. 2 ) [ 11 , 14 , 22 , 24 , 27 , 28 , 29 ]. Importantly, however, most of these studies have investigated only short-term effects [ 10 , 14 , 15 , 22 , 27 , 28 , 29 , 31 , 32 ], and the long-term effects of e-cigarette consumption on human health are still unclear and require further study.
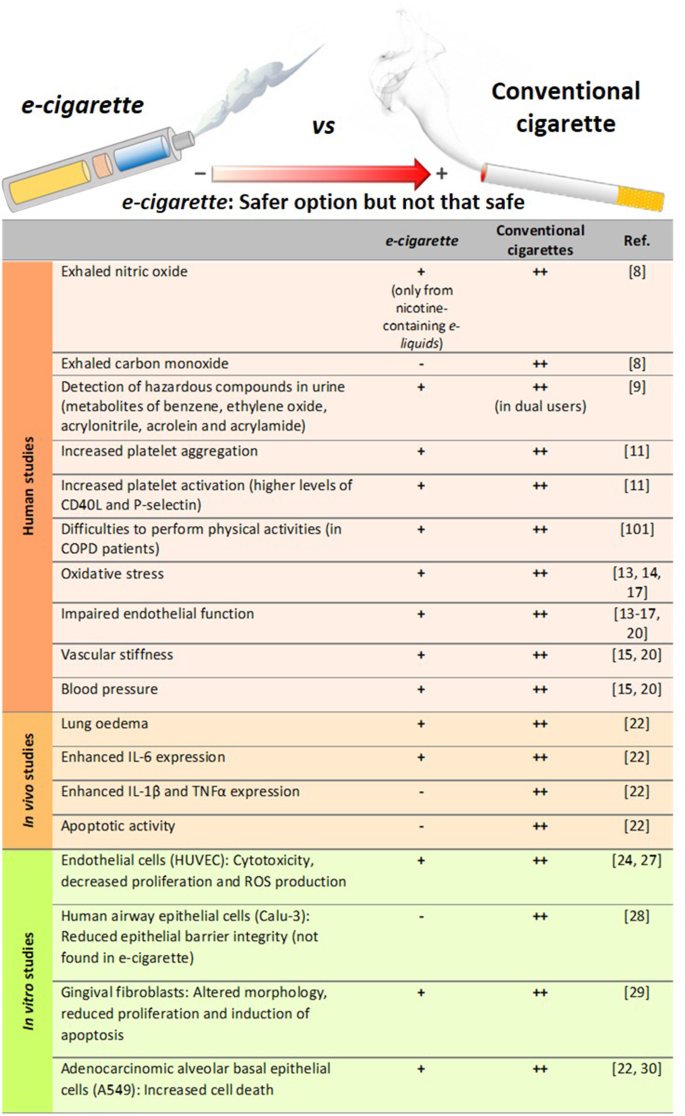
Comparison of the degree of harmful effects documented from e-cigarette and conventional cigarette consumption. Human studies, in vivo mice exposure and in vitro studies. All of these effects from e-cigarettes were documented to be lower than those exerted by conventional cigarettes, which may suggest that e-cigarette consumption could be a safer option than conventional tobacco smoking but not a clear safe choice
Consequences of nicotine content
Beyond flavour, one of the major issues in the e-liquid market is the range of nicotine content available. Depending on the manufacturer, the concentration of this alkaloid can be presented as low , medium or high , or expressed as mg/mL or as a percentage (% v/v). The concentrations range from 0 (0%, nicotine-free option) to 20 mg/mL (2.0%)—the maximum nicotine threshold according to directive 2014/40/EU of the European Parliament and the European Union Council [ 33 , 34 ]. Despite this normative, however, some commercial e-liquids have nicotine concentrations close to 54 mg/mL [ 35 ], much higher than the limits established by the European Union.
The mislabelling of nicotine content in e-liquids has been previously addressed [ 8 , 34 ]. For instance, gas chromatography with a flame ionisation detector (GC-FID) revealed inconsistencies in the nicotine content with respect to the manufacturer´s declaration (average of 22 ± 0.8 mg/mL vs. 18 mg/mL) [ 8 ], which equates to a content ~ 22% higher than that indicated in the product label. Of note, several studies have detected nicotine in those e-liquids labelled as nicotine-free [ 5 , 35 , 36 ]. One study detected the presence of nicotine (0.11–6.90 mg/mL) in 5 of 23 nicotine-free labelled e-liquids by nuclear magnetic resonance spectroscopy [ 35 ], and another study found nicotine (average 8.9 mg/mL) in 13.6% (17/125) of the nicotine-free e-liquids as analysed by high performance liquid chromatography (HPLC) [ 36 ]. Among the 17 samples tested in this latter study 14 were identified to be counterfeit or suspected counterfeit. A third study detected nicotine in 7 of 10 nicotine-free refills, although the concentrations were lower than those identified in the previous analyses (0.1–15 µg/mL) [ 5 ]. Not only is there evidence of mislabelling of nicotine content among refills labelled as nicotine-free, but there also seems to be a history of poor labelling accuracy in nicotine-containing e-liquids [ 37 , 38 ].
A comparison of the serum levels of nicotine from e-cigarette or conventional cigarette consumption has been recently reported [ 39 ]. Participants took one vape from an e-cigarette , with at least 12 mg/mL of nicotine, or inhaled a conventional cigarette, every 20 s for 10 min. Blood samples were collected 1, 2, 4, 6, 8, 10, 12 and 15 min after the first puff, and nicotine serum levels were measured by liquid chromatography-mass spectrometry (LC–MS). The results revealed higher serum levels of nicotine in the conventional CS group than in the e-cigarette group (25.9 ± 16.7 ng/mL vs. 11.5 ± 9.8 ng/mL). However, e-cigarettes containing 20 mg/mL of nicotine are more equivalent to normal cigarettes, based on the delivery of approximately 1 mg of nicotine every 5 min [ 40 ].
In this line, a study compared the acute impact of CS vs. e-cigarette vaping with equivalent nicotine content in healthy smokers and non-smokers. Both increased markers of oxidative stress and decreased NO bioavailability, flow-mediated dilation, and vitamin E levels showing no significant differences between tobacco and e-cigarette exposure (reviewed in [ 20 ]). Inasmuch, short-term e-cigarette use in healthy smokers resulted in marked impairment of endothelial function and an increase in arterial stiffness (reviewed in [ 20 ]). Similar effects on endothelial dysfunction and arterial stiffness were found in animals when they were exposed to e-cigarette vapor either for several days or chronically (reviewed in [ 20 ]). In contrast, other studies found acute microvascular endothelial dysfunction, increased oxidative stress and arterial stiffness in smokers after exposure to e-cigarettes with nicotine, but not after e-cigarettes without nicotine (reviewed in [ 20 ]). In women smokers, a study found a significant difference in stiffness after smoking just one tobacco cigarette, but not after use of e-cigarettes (reviewed in [ 20 ]).
It is well known that nicotine is extremely addictive and has a multitude of harmful effects. Nicotine has significant biologic activity and adversely affects several physiological systems including the cardiovascular, respiratory, immunological and reproductive systems, and can also compromise lung and kidney function [ 41 ]. Recently, a sub-chronic whole-body exposure of e-liquid (2 h/day, 5 days/week, 30 days) containing PG alone or PG with nicotine (25 mg/mL) to wild type (WT) animals or knockout (KO) mice in α7 nicotinic acetylcholine receptor (nAChRα7-KO) revealed a partly nAChRα7-dependent lung inflammation [ 42 ]. While sub-chronic exposure to PG/nicotine promote nAChRα7-dependent increased levels of different cytokines and chemokines in the bronchoalveolar lavage fluid (BALF) such as IL-1α, IL-2, IL-9, interferon γ (IFNγ), granulocyte-macrophage colony-stimulating factor (GM-CSF), monocyte chemoattractant protein-1 (MCP-1/CCL2) and regulated on activation, normal T cell expressed and secreted (RANTES/CCL5), the enhanced levels of IL-1β, IL-5 and TNFα were nAChRα7 independent. In general, most of the cytokines detected in BALF were significantly increased in WT mice exposed to PG with nicotine compared to PG alone or air control [ 42 ]. Some of these effects were found to be through nicotine activation of NF-κB signalling albeit in females but not in males. In addition, PG with nicotine caused increased macrophage and CD4 + /CD8 + T-lymphocytes cell counts in BALF compared to air control, but these effects were ameliorated when animals were sub-chronically exposed to PG alone [ 42 ].
Of note, another study indicated that although RANTES/CCL5 and CCR1 mRNA were upregulated in flavour/nicotine-containing e-cigarette users, vaping flavour and nicotine-less e-cigarettes did not significantly dysregulate cytokine and inflammasome activation [ 43 ].
In addition to its toxicological effects on foetus development, nicotine can disrupt brain development in adolescents and young adults [ 44 , 45 , 46 ]. Several studies have also suggested that nicotine is potentially carcinogenic (reviewed in [ 41 ]), but more work is needed to prove its carcinogenicity independently of the combustion products of tobacco [ 47 ]. In this latter regard, no differences were encountered in the frequency of tumour appearance in rats subjected to long-term (2 years) inhalation of nicotine when compared with control rats [ 48 ]. Despite the lack of carcinogenicity evidence, it has been reported that nicotine promotes tumour cell survival by decreasing apoptosis and increasing proliferation [ 49 ], indicating that it may work as a “tumour enhancer”. In a very recent study, chronic administration of nicotine to mice (1 mg/kg every 3 days for a 60-day period) enhanced brain metastasis by skewing the polarity of M2 microglia, which increases metastatic tumour growth [ 50 ]. Assuming that a conventional cigarette contains 0.172–1.702 mg of nicotine [ 51 ], the daily nicotine dose administered to these animals corresponds to 40–400 cigarettes for a 70 kg-adult, which is a dose of an extremely heavy smoker. We would argue that further studies with chronic administration of low doses of nicotine are required to clearly evaluate its impact on carcinogenicity.
In the aforementioned study exposing human gingival fibroblasts to CS condensate or to nicotine-rich or nicotine-free e-vapour condensates [ 29 ], the detrimental effects were greater in cells exposed to nicotine-rich condensate than to nicotine-free condensate, suggesting that the possible injurious effects of nicotine should be considered when purchasing e-refills . It is also noteworthy that among the 3 most cytotoxic vapours for HUVEC evaluated in the Putzhammer et al . study, 2 were nicotine-free, which suggests that nicotine is not the only hazardous component in e-cigarettes [ 24 ] .
The lethal dose of nicotine for an adult is estimated at 30–60 mg [ 52 ]. Given that nicotine easily diffuses from the dermis to the bloodstream, acute nicotine exposure by e-liquid spilling (5 mL of a 20 mg/mL nicotine-containing refill is equivalent to 100 mg of nicotine) can easily be toxic or even deadly [ 8 ]. Thus, devices with rechargeable refills are another issue of concern with e-cigarettes , especially when e-liquids are not sold in child-safe containers, increasing the risk of spilling, swallowing or breathing.
These data overall indicate that the harmful effects of nicotine should not be underestimated. Despite the established regulations, some inaccuracies in nicotine content labelling remain in different brands of e-liquids . Consequently, stricter regulation and a higher quality control in the e-liquid industry are required.
Effect of humectants and their heating-related products
In this particular aspect, again the composition of the e-liquid varies significantly among different commercial brands [ 4 , 35 ]. The most common and major components of e-liquids are PG or 1,2-propanediol, and glycerol or glycerine (propane-1,2,3-triol). Both types of compounds are used as humectants to prevent the e-liquid from drying out [ 2 , 53 ] and are classified by the Food and Drug Administration (FDA) as “Generally Recognised as Safe” [ 54 ]. In fact, they are widely used as alimentary and pharmaceutical products [ 2 ]. In an analysis of 54 commercially available e-liquids , PG and glycerol were detected in almost all samples at concentrations ranging from 0.4% to 98% (average 57%) and from 0.3% to 95% (average 37%), respectively [ 35 ].
With regards to toxicity, little is known about the effects of humectants when they are heated and chronically inhaled. Studies have indicated that PG can induce respiratory irritation and increase the probability of asthma development [ 55 , 56 ], and both PG and glycerol from e-cigarettes might reach concentrations sufficiently high to potentially cause irritation of the airways [ 57 ]. Indeed, the latter study established that one e-cigarette puff results in a PG exposure of 430–603 mg/m 3 , which is higher than the levels reported to cause airway irritation (average 309 mg/m 3 ) based on a human study [ 55 ]. The same study established that one e-cigarette puff results in a glycerol exposure of 348–495 mg/m 3 [ 57 ], which is close to the levels reported to cause airway irritation in rats (662 mg/m 3 ) [ 58 ].
Airway epithelial injury induced by acute vaping of PG and glycerol aerosols (50:50 vol/vol), with or without nicotine, has been reported in two randomised clinical trials in young tobacco smokers [ 32 ]. In vitro, aerosols from glycerol only-containing refills showed cytotoxicity in A549 and human embryonic stem cells, even at a low battery output voltage [ 59 ]. PG was also found to affect early neurodevelopment in a zebrafish model [ 60 ]. Another important issue is that, under heating conditions PG can produce acetaldehyde or formaldehyde (119.2 or 143.7 ng/puff at 20 W, respectively, on average), while glycerol can also generate acrolein (53.0, 1000.0 or 5.9 ng/puff at 20 W, respectively, on average), all carbonyls with a well-documented toxicity [ 61 ]. Although, assuming 15 puffs per e-cigarette unit, carbonyls produced by PG or glycerol heating would be below the maximum levels found in a conventional cigarette combustion (Table 2 ) [ 51 , 62 ]. Nevertheless, further studies are required to properly test the deleterious effects of all these compounds at physiological doses resembling those to which individuals are chronically exposed.
Although PG and glycerol are the major components of e-liquids other components have been detected. When the aerosols of 4 commercially available e-liquids chosen from a top 10 list of “ Best E-Cigarettes of 2014” , were analysed by gas chromatography-mass spectrometry (GC–MS) after heating, numerous compounds were detected, with nearly half of them not previously identified [ 4 ], thus suggesting that the heating process per se generates new compounds of unknown consequence. Of note, the analysis identified formaldehyde, acetaldehyde and acrolein [ 4 ], 3 carbonyl compounds with known high toxicity [ 63 , 64 , 65 , 66 , 67 ]. While no information was given regarding formaldehyde and acetaldehyde concentrations, the authors calculated that one puff could result in an acrolein exposure of 0.003–0.015 μg/mL [ 4 ]. Assuming 40 mL per puff and 15 puffs per e-cigarette unit (according to several manufacturers) [ 4 ], each e-cigarette unit would generate approximately 1.8–9 μg of acrolein, which is less than the levels of acrolein emitted by a conventional tobacco cigarette (18.3–98.2 μg) [ 51 ]. However, given that e-cigarette units of vaping are not well established, users may puff intermittently throughout the whole day. Thus, assuming 400 to 500 puffs per cartridge, users could be exposed to up to 300 μg of acrolein.
In a similar study, acrolein was found in 11 of 12 aerosols tested, with a similar content range (approximately 0.07–4.19 μg per e-cigarette unit) [ 68 ]. In the same study, both formaldehyde and acetaldehyde were detected in all of the aerosols tested, with contents of 0.2–5.61 μg and 0.11–1.36 μg, respectively, per e-cigarette unit [ 68 ]. It is important to point out that the levels of these toxic products in e-cigarette aerosols are significantly lower than those found in CS: 9 times lower for formaldehyde, 450 times lower for acetaldehyde and 15 times lower for acrolein (Table 2 ) [ 62 , 68 ].
Other compounds that have been detected in aerosols include acetamide, a potential human carcinogen [ 5 ], and some aldehydes [ 69 ], although their levels were minimal. Interestingly, the existence of harmful concentrations of diethylene glycol, a known cytotoxic agent, in e-liquid aerosols is contentious with some studies detecting its presence [ 4 , 68 , 70 , 71 , 72 ], and others finding low subtoxic concentrations [ 73 , 74 ]. Similar observations were reported for the content ethylene glycol. In this regard, either it was detected at concentrations that did not exceed the authorised limit [ 73 ], or it was absent from the aerosols produced [ 4 , 71 , 72 ]. Only one study revealed its presence at high concentration in a very low number of samples [ 5 ]. Nevertheless, its presence above 1 mg/g is not allowed by the FDA [ 73 ]. Figure 1 lists the main compounds detected in aerosols derived from humectant heating and their potential damaging effects. It would seem that future studies should analyse the possible toxic effects of humectants and related products at concentrations similar to those that e-cigarette vapers are exposed to reach conclusive results.
Impact of flavouring compounds
The range of e-liquid flavours available to consumers is extensive and is used to attract both current smokers and new e-cigarette users, which is a growing public health concern [ 6 ]. In fact, over 5 million middle- and high-school students were current users of e-cigarettes in 2019 [ 75 ], and appealing flavours have been identified as the primary reason for e-cigarette consumption in 81% of young users [ 76 ]. Since 2016, the FDA regulates the flavours used in the e-cigarette market and has recently published an enforcement policy on unauthorised flavours, including fruit and mint flavours, which are more appealing to young users [ 77 ]. However, the long-term effects of all flavour chemicals used by this industry (which are more than 15,000) remain unknown and they are not usually included in the product label [ 78 ]. Furthermore, there is no safety guarantee since they may harbour potential toxic or irritating properties [ 5 ].
With regards to the multitude of available flavours, some have demonstrated cytotoxicity [ 59 , 79 ]. Bahl et al. evaluated the toxicity of 36 different e-liquids and 29 different flavours on human embryonic stem cells, mouse neural stem cells and human pulmonary fibroblasts using a metabolic activity assay. In general, those e-liquids that were bubblegum-, butterscotch- and caramel-flavoured did not show any overt cytotoxicity even at the highest dose tested. By contrast, those e-liquids with Freedom Smoke Menthol Arctic and Global Smoke Caramel flavours had marked cytotoxic effects on pulmonary fibroblasts and those with Cinnamon Ceylon flavour were the most cytotoxic in all cell lines [ 79 ]. A further study from the same group [ 80 ] revealed that high cytotoxicity is a recurrent feature of cinnamon-flavoured e-liquids. In this line, results from GC–MS and HPLC analyses indicated that cinnamaldehyde (CAD) and 2-methoxycinnamaldehyde, but not dipropylene glycol or vanillin, were mainly responsible for the high cytotoxicity of cinnamon-flavoured e-liquids [ 80 ]. Other flavouring-related compounds that are associated with respiratory complications [ 81 , 82 , 83 ], such as diacetyl, 2,3-pentanedione or acetoin, were found in 47 out of 51 aerosols of flavoured e-liquids tested [ 84 ] . Allen et al . calculated an average of 239 μg of diacetyl per cartridge [ 84 ]. Assuming again 400 puffs per cartridge and 40 mL per puff, is it is possible to estimate an average of 0.015 ppm of diacetyl per puff, which could compromise normal lung function in the long-term [ 85 ].
The cytotoxic and pro-inflammatory effects of different e-cigarette flavouring chemicals were also tested on two human monocytic cell lines—mono mac 6 (MM6) and U937 [ 86 ]. Among the flavouring chemicals tested, CAD was found to be the most toxic and O-vanillin and pentanedione also showed significant cytotoxicity; by contrast, acetoin, diacetyl, maltol, and coumarin did not show any toxicity at the concentrations assayed (10–1000 µM). Of interest, a higher toxicity was evident when combinations of different flavours or mixed equal proportions of e-liquids from 10 differently flavoured e-liquids were tested, suggesting that vaping a single flavour is less toxic than inhaling mixed flavours [ 86 ]. Also, all the tested flavours produced significant levels of ROS in a cell-free ROS production assay. Finally, diacetyl, pentanedione, O-vanillin, maltol, coumarin, and CAD induced significant IL-8 secretion from MM6 and U937 monocytes [ 86 ]. It should be borne in mind, however, that the concentrations assayed were in the supra-physiological range and it is likely that, once inhaled, these concentrations are not reached in the airway space. Indeed, one of the limitations of the study was that human cells are not exposed to e-liquids per se, but rather to the aerosols where the concentrations are lower [ 86 ]. In this line, the maximum concentration tested (1000 µM) would correspond to approximately 80 to 150 ppm, which is far higher than the levels found in aerosols of some of these compounds [ 84 ]. Moreover, on a day-to-day basis, lungs of e-cigarette users are not constantly exposed to these chemicals for 24 h at these concentrations. Similar limitations were found when five of seven flavourings were found to cause cytotoxicity in human bronchial epithelial cells [ 87 ].
Recently, a commonly commercialized crème brûlée -flavoured aerosol was found to contain high concentrations of benzoic acid (86.9 μg/puff), a well-established respiratory irritant [ 88 ]. When human lung epithelial cells (BEAS-2B and H292) were exposed to this aerosol for 1 h, a marked cytotoxicity was observed in BEAS-2B but not in H292 cells, 24 h later. However, increased ROS production was registered in H292 cells [ 88 ].
Therefore, to fully understand the effects of these compounds, it is relevant the cell cultures selected for performing these assays, as well as the use of in vivo models that mimic the real-life situation of chronic e-cigarette vapers to clarify their impact on human health.
The e-cigarette device
While the bulk of studies related to the impact of e-cigarette use on human health has focused on the e-liquid components and the resulting aerosols produced after heating, a few studies have addressed the material of the electronic device and its potential consequences—specifically, the potential presence of metals such as copper, nickel or silver particles in e-liquids and aerosols originating from the filaments and wires and the atomiser [ 89 , 90 , 91 ].
Other important components in the aerosols include silicate particles from the fiberglass wicks or silicone [ 89 , 90 , 91 ]. Many of these products are known to cause abnormalities in respiratory function and respiratory diseases [ 89 , 90 , 91 ], but more in-depth studies are required. Interestingly, the battery output voltage also seems to have an impact on the cytotoxicity of the aerosol vapours, with e-liquids from a higher battery output voltage showing more toxicity to A549 cells [ 30 ].
A recent study compared the acute effects of e-cigarette vapor (with PG/vegetable glycerine plus tobacco flavouring but without nicotine) generated from stainless‐steel atomizer (SS) heating element or from a nickel‐chromium alloy (NC) [ 92 ]. Some rats received a single e-cigarette exposure for 2 h from a NC heating element (60 or 70 W); other rats received a similar exposure of e-cigarette vapor using a SS heating element for the same period of time (60 or 70 W) and, a final group of animals were exposed for 2 h to air. Neither the air‐exposed rats nor those exposed to e-cigarette vapor using SS heating elements developed respiratory distress. In contrast, 80% of the rats exposed to e-cigarette vapor using NC heating units developed clinical acute respiratory distress when a 70‐W power setting was employed. Thus, suggesting that operating units at higher than recommended settings can cause adverse effects. Nevertheless, there is no doubt that the deleterious effects of battery output voltage are not comparable to those exerted by CS extracts [ 30 ] (Figs. 1 and 2 ).
E-cigarettes as a smoking cessation tool
CS contains a large number of substances—about 7000 different constituents in total, with sizes ranging from atoms to particulate matter, and with many hundreds likely responsible for the harmful effects of this habit [ 93 ]. Given that tobacco is being substituted in great part by e-cigarettes with different chemical compositions, manufacturers claim that e -cigarette will not cause lung diseases such as lung cancer, chronic obstructive pulmonary disease, or cardiovascular disorders often associated with conventional cigarette consumption [ 3 , 94 ]. However, the World Health Organisation suggests that e-cigarettes cannot be considered as a viable method to quit smoking, due to a lack of evidence [ 7 , 95 ]. Indeed, the results of studies addressing the use of e-cigarettes as a smoking cessation tool remain controversial [ 96 , 97 , 98 , 99 , 100 ]. Moreover, both FDA and CDC are actively investigating the incidence of severe respiratory symptoms associated with the use of vaping products [ 77 ]. Because many e-liquids contain nicotine, which is well known for its powerful addictive properties [ 41 ], e-cigarette users can easily switch to conventional cigarette smoking, avoiding smoking cessation. Nevertheless, the possibility of vaping nicotine-free e-cigarettes has led to the branding of these devices as smoking cessation tools [ 2 , 6 , 7 ].
In a recently published randomised trial of 886 subjects who were willing to quit smoking [ 100 ], the abstinence rate was found to be twice as high in the e-cigarette group than in the nicotine-replacement group (18.0% vs. 9.9%) after 1 year. Of note, the abstinence rate found in the nicotine-replacement group was lower than what is usually expected with this therapy. Nevertheless, the incidence of throat and mouth irritation was higher in the e-cigarette group than in the nicotine-replacement group (65.3% vs. 51.2%, respectively). Also, the participant adherence to the treatment after 1-year abstinence was significantly higher in the e-cigarette group (80%) than in nicotine-replacement products group (9%) [ 100 ].
On the other hand, it is estimated that COPD could become the third leading cause of death in 2030 [ 101 ]. Given that COPD is generally associated with smoking habits (approximately 15 to 20% of smokers develop COPD) [ 101 ], smoking cessation is imperative among COPD smokers. Published data revealed a clear reduction of conventional cigarette consumption in COPD smokers that switched to e-cigarettes [ 101 ]. Indeed, a significant reduction in exacerbations was observed and, consequently, the ability to perform physical activities was improved when data was compared with those non-vapers COPD smokers. Nevertheless, a longer follow-up of these COPD patients is required to find out whether they have quitted conventional smoking or even vaping, since the final goal under these circumstances is to quit both habits.
Based on the current literature, it seems that several factors have led to the success of e-cigarette use as a smoking cessation tool. First, some e-cigarette flavours positively affect smoking cessation outcomes among smokers [ 102 ]. Second, e-cigarettes have been described to improve smoking cessation rate only among highly-dependent smokers and not among conventional smokers, suggesting that the individual degree of nicotine dependence plays an important role in this process [ 97 ]. Third, the general belief of their relative harmfulness to consumers' health compared with conventional combustible tobacco [ 103 ]. And finally, the exposure to point-of-sale marketing of e-cigarette has also been identified to affect the smoking cessation success [ 96 ].
Implication of e-cigarette consumption in COVID-19 time
Different reports have pointed out that smokers and vapers are more vulnerable to SARS-CoV-2 (Severe Acute Respiratory Syndrome Coronavirus 2) infections or more prone to adverse outcomes if they suffer COVID-19 [ 104 ]. However, while a systematic review indicated that cigarette smoking is probably associated with enhanced damage from COVID-19, a meta-analysis did not, yet the latter had several limitations due to the small sample sizes [ 105 ].
Interestingly, most of these reports linking COVID-19 harmful effects with smoking or vaping, are based on their capability of increasing the expression of angiotensin-converting enzyme 2 (ACE2) in the lung. It is well known that ACE2 is the gate for SARS-CoV-2 entrance to the airways [ 106 ] and it is mainly expressed in type 2 alveolar epithelial cells and alveolar macrophages [ 107 ]. To date, most of the studies in this field indicate that current smokers have higher expression of ACE2 in the airways (reviewed by [ 108 ]) than healthy non-smokers [ 109 , 110 ]. However, while a recent report indicated that e-cigarette vaping also caused nicotine-dependent ACE2 up-regulation [ 42 ], others have revealed that neither acute inhalation of e-cigarette vapour nor e-cigarette users had increased lung ACE2 expression regardless nicotine presence in the e-liquid [ 43 , 110 ].
In regard to these contentions, current knowledge suggests that increased ACE2 expression is not necessarily linked to enhanced susceptibility to SARS-CoV-2 infection and adverse outcome. Indeed, elderly population express lower levels of ACE2 than young people and SARS-CoV-2/ACE2 interaction further decreases ACE2 expression. In fact, most of the deaths provoked by COVID-19 took place in people over 60 years old of age [ 111 ]. Therefore, it is plausible that the increased susceptibility to disease progression and the subsequent fatal outcome in this population is related to poor angiotensin 1-7 (Ang-1-7) generation, the main peptide generated by ACE2, and probably to their inaccessibility to its anti-inflammatory effects. Furthermore, it seems that all the efforts towards increasing ACE2 expression may result in a better resolution of the pneumonic process associated to this pandemic disease.
Nevertheless, additional complications associated to COVID-19 are increased thrombotic events and cytokine storm. In the lungs, e-cigarette consumption has been correlated to toxicity, oxidative stress, and inflammatory response [ 32 , 112 ]. More recently, a study revealed that while the use of nicotine/flavour-containing e-cigarettes led to significant cytokine dysregulation and potential inflammasome activation, none of these effects were detected in non-flavoured and non-nicotine-containing e-cigarettes [ 43 ]. Therefore, taken together these observations, e-cigarette use may still be a potent risk factor for severe COVID-19 development depending on the flavour and nicotine content.
In summary, it seems that either smoking or nicotine vaping may adversely impact on COVID-19 outcome. However, additional follow up studies are required in COVID-19 pandemic to clarify the effect of e-cigarette use on lung and cardiovascular complications derived from SARS-CoV-2 infection.
Conclusions
The harmful effects of CS and their deleterious consequences are both well recognised and widely investigated. However, and based on the studies carried out so far, it seems that e-cigarette consumption is less toxic than tobacco smoking. This does not necessarily mean, however, that e-cigarettes are free from hazardous effects. Indeed, studies investigating their long-term effects on human health are urgently required. In this regard, the main additional studies needed in this field are summarized in Table 3 .
The composition of e-liquids requires stricter regulation, as they can be easily bought online and many incidences of mislabelling have been detected, which can seriously affect consumers’ health. Beyond their unknown long-term effects on human health, the extended list of appealing flavours available seems to attract new “never-smokers”, which is especially worrying among young users. Additionally, there is still a lack of evidence of e-cigarette consumption as a smoking cessation method. Indeed, e-cigarettes containing nicotine may relieve the craving for smoking, but not the conventional cigarette smoking habit.
Interestingly, there is a strong difference of opinion on e-cigarettes between countries. Whereas countries such as Brazil, Uruguay and India have banned the sale of e-cigarettes , others such as the United Kingdom support this device to quit smoking. The increasing number of adolescent users and reported deaths in the United States prompted the government to ban the sale of flavoured e-cigarettes in 2020. The difference in opinion worldwide may be due to different restrictions imposed. For example, while no more than 20 ng/mL of nicotine is allowed in the EU, e-liquids with 59 mg/dL are currently available in the United States. Nevertheless, despite the national restrictions, users can easily access foreign or even counterfeit products online.
In regard to COVID-19 pandemic, the actual literature suggests that nicotine vaping may display adverse outcomes. Therefore, follow up studies are necessary to clarify the impact of e-cigarette consumption on human health in SARS-CoV-2 infection.
In conclusion, e-cigarettes could be a good alternative to conventional tobacco cigarettes, with less side effects; however, a stricter sale control, a proper regulation of the industry including flavour restriction, as well as further toxicological studies, including their chronic effects, are warranted.
Availability of data and materials
Not applicable.
Abbreviations
Angiotensin-converting enzyme 2
Angiotensin 1-7
Bronchoalveolar lavage fluid
Cinnamaldehyde
US Centers for Disease Control and Prevention
Carbon monoxide
Chronic obstructive pulmonary disease
Coronavirus disease 2019
Cigarette smoke
Electronic nicotine dispensing systems
e-cigarette or vaping product use-associated lung injury
Food and Drug Administration
Gas chromatography with a flame ionisation detector
Gas chromatography-mass spectrometry
Granulocyte–macrophage colony-stimulating factor
High performance liquid chromatography
Human umbilical vein endothelial cells
Interleukin
Interferon γ
Liquid chromatography-mass spectrometry
Monocyte chemoattractant protein-1
Matrix metallopeptidase 9
α7 Nicotinic acetylcholine receptor
Nickel‐chromium alloy
Nitric oxide
Propylene glycol
Regulated on activation, normal T cell expressed and secreted
Reactive oxygen species
Severe acute respiratory syndrome coronavirus 2
Stainless‐steel atomizer
Tetrahydrocannabinol
Tumour necrosis factor-α
Hiemstra PS, Bals R. Basic science of electronic cigarettes: assessment in cell culture and in vivo models. Respir Res. 2016;17(1):127.
Article PubMed PubMed Central CAS Google Scholar
Bertholon JF, Becquemin MH, Annesi-Maesano I, Dautzenberg B. Electronic cigarettes: a short review. Respiration. 2013;86(5):433–8.
Article CAS PubMed Google Scholar
Rowell TR, Tarran R. Will chronic e-cigarette use cause lung disease? Am J Physiol Lung Cell Mol Physiol. 2015;309(12):L1398–409.
Article CAS PubMed PubMed Central Google Scholar
Herrington JS, Myers C. Electronic cigarette solutions and resultant aerosol profiles. J Chromatogr A. 2015;1418:192–9.
Hutzler C, Paschke M, Kruschinski S, Henkler F, Hahn J, Luch A. Chemical hazards present in liquids and vapors of electronic cigarettes. Arch Toxicol. 2014;88(7):1295–308.
Pokhrel P, Herzog TA, Muranaka N, Fagan P. Young adult e-cigarette users’ reasons for liking and not liking e-cigarettes: a qualitative study. Psychol Health. 2015;30(12):1450–69.
Article PubMed PubMed Central Google Scholar
Harrell PT, Simmons VN, Correa JB, Padhya TA, Brandon TH. Electronic nicotine delivery systems (“e-cigarettes”): review of safety and smoking cessation efficacy. Otolaryngol Head Neck Surg. 2014;151(3):381–93.
Schober W, Szendrei K, Matzen W, Osiander-Fuchs H, Heitmann D, Schettgen T, et al. Use of electronic cigarettes (e-cigarettes) impairs indoor air quality and increases FeNO levels of e-cigarette consumers. Int J Hyg Environ Health. 2014;217(6):628–37.
Rubinstein ML, Delucchi K, Benowitz NL, Ramo DE. Adolescent exposure to toxic volatile organic chemicals from E-cigarettes. Pediatrics. 2018;141(4):e20173557.
Article PubMed Google Scholar
Staudt MR, Salit J, Kaner RJ, Hollmann C, Crystal RG. Altered lung biology of healthy never smokers following acute inhalation of E-cigarettes. Respir Res. 2018;19(1):78.
Nocella C, Biondi-Zoccai G, Sciarretta S, Peruzzi M, Pagano F, Loffredo L, et al. Impact of tobacco versus electronic cigarette smoking on platelet function. Am J Cardiol. 2018;122(9):1477–81.
Higham A, Rattray NJW, Dewhurst JA, Trivedi DK, Fowler SJ, Goodacre R, et al. Electronic cigarette exposure triggers neutrophil inflammatory responses. Respir Res. 2016;17(1):56.
Antoniewicz L, Bosson JA, Kuhl J, Abdel-Halim SM, Kiessling A, Mobarrez F, et al. Electronic cigarettes increase endothelial progenitor cells in the blood of healthy volunteers. Atherosclerosis. 2016;255:179–85.
Carnevale R, Sciarretta S, Violi F, Nocella C, Loffredo L, Perri L, et al. Acute impact of tobacco vs electronic cigarette smoking on oxidative stress and vascular function. Chest. 2016;150(3):606–12.
Vlachopoulos C, Ioakeimidis N, Abdelrasoul M, Terentes-Printzios D, Georgakopoulos C, Pietri P, et al. Electronic cigarette smoking increases aortic stiffness and blood pressure in young smokers. J Am Coll Cardiol. 2016;67(23):2802–3.
Franzen KF, Willig J, Cayo Talavera S, Meusel M, Sayk F, Reppel M, et al. E-cigarettes and cigarettes worsen peripheral and central hemodynamics as well as arterial stiffness: a randomized, double-blinded pilot study. Vasc Med. 2018;23(5):419–25.
Caporale A, Langham MC, Guo W, Johncola A, Chatterjee S, Wehrli FW. Acute effects of electronic cigarette aerosol inhalation on vascular function detected at quantitative MRI. Radiology. 2019;293(1):97–106.
von Hundelshausen P, Schmitt MM. Platelets and their chemokines in atherosclerosis-clinical applications. Front Physiol. 2014;5:294.
Google Scholar
Landmesser U, Hornig B, Drexler H. Endothelial function: a critical determinant in atherosclerosis? Circulation. 2004;109(21 Suppl 1):Ii27-33.
PubMed Google Scholar
Münzel T, Hahad O, Kuntic M, Keaney JF, Deanfield JE, Daiber A. Effects of tobacco cigarettes, e-cigarettes, and waterpipe smoking on endothelial function and clinical outcomes. Eur Heart J. 2020;41:4057–70.
Javelle E. Electronic cigarette and vaping should be discouraged during the new coronavirus SARS-CoV-2 pandemic. Arch Toxicol. 2020;94(6):2261–2.
Husari A, Shihadeh A, Talih S, Hashem Y, El Sabban M, Zaatari G. Acute exposure to electronic and combustible cigarette aerosols: effects in an animal model and in human alveolar cells. Nicotine Tob Res. 2016;18(5):613–9.
Zelikoff JT, Parmalee NL, Corbett K, Gordon T, Klein CB, Aschner M. Microglia activation and gene expression alteration of neurotrophins in the hippocampus following early-life exposure to E-cigarette aerosols in a murine model. Toxicol Sci. 2018;162(1):276–86.
Putzhammer R, Doppler C, Jakschitz T, Heinz K, Forste J, Danzl K, et al. Vapours of US and EU market leader electronic cigarette brands and liquids are cytotoxic for human vascular endothelial cells. PLoS One. 2016;11(6):e0157337.
Bernhard D, Pfister G, Huck CW, Kind M, Salvenmoser W, Bonn GK, et al. Disruption of vascular endothelial homeostasis by tobacco smoke: impact on atherosclerosis. Faseb J. 2003;17(15):2302–4.
Newby DE, Wright RA, Labinjoh C, Ludlam CA, Fox KA, Boon NA, et al. Endothelial dysfunction, impaired endogenous fibrinolysis, and cigarette smoking: a mechanism for arterial thrombosis and myocardial infarction. Circulation. 1999;99(11):1411–5.
Taylor M, Jaunky T, Hewitt K, Breheny D, Lowe F, Fearon IM, et al. A comparative assessment of e-cigarette aerosols and cigarette smoke on in vitro endothelial cell migration. Toxicol Lett. 2017;277:123–8.
Herr C, Tsitouras K, Niederstraßer J, Backes C, Beisswenger C, Dong L, et al. Cigarette smoke and electronic cigarettes differentially activate bronchial epithelial cells. Respir Res. 2020;21(1):67.
Alanazi H, Park HJ, Chakir J, Semlali A, Rouabhia M. Comparative study of the effects of cigarette smoke and electronic cigarettes on human gingival fibroblast proliferation, migration and apoptosis. Food Chem Toxicol. 2018;118:390–8.
Otreba M, Kosmider L. E-cigarettes: voltage- and concentration-dependent loss in human lung adenocarcinoma viability. J Appl Toxicol. 2018;38(8):1135–43.
Chaumont M, Bernard A, Pochet S, Melot C, El Khattabi C, Reye F, et al. High-wattage E-cigarettes induce tissue hypoxia and lower airway injury: a randomized clinical trial. Am J Respir Crit Care Med. 2018;198(1):123–6.
Chaumont M, van de Borne P, Bernard A, Van Muylem A, Deprez G, Ullmo J, et al. Fourth generation e-cigarette vaping induces transient lung inflammation and gas exchange disturbances: results from two randomized clinical trials. Am J Physiol Lung Cell Mol Physiol. 2019;316(5):L705–19.
European Parliament and the council of the European Union. Directive 2014/40/EU. 2014 (updated April 29, 2014). https://ec.europa.eu/health//sites/health/files/tobacco/docs/dir_201440_en.pdf . Accessed 17 April 2020.
Cameron JM, Howell DN, White JR, Andrenyak DM, Layton ME, Roll JM. Variable and potentially fatal amounts of nicotine in e-cigarette nicotine solutions. Tob Control. 2014;23(1):77–8.
Hahn J, Monakhova YB, Hengen J, Kohl-Himmelseher M, Schussler J, Hahn H, et al. Electronic cigarettes: overview of chemical composition and exposure estimation. Tob Induc Dis. 2014;12(1):23.
Omaiye EE, Cordova I, Davis B, Talbot P. Counterfeit electronic cigarette products with mislabeled nicotine concentrations. Tob Regul Sci. 2017;3(3):347–57.
Buettner-Schmidt K, Miller DR, Balasubramanian N. Electronic cigarette refill liquids: child-resistant packaging, nicotine content, and sales to minors. J Pediatr Nurs. 2016;31(4):373–9.
Jackson R, Huskey M, Brown S. Labelling accuracy in low nicotine e-cigarette liquids from a sampling of US manufacturers. Int J Pharm Pract. 2019;28(3):290–4.
Yingst JM, Foulds J, Veldheer S, Hrabovsky S, Trushin N, Eissenberg TT, et al. Nicotine absorption during electronic cigarette use among regular users. PLoS One. 2019;14(7):e0220300.
Farsalinos KE, Romagna G, Tsiapras D, Kyrzopoulos S, Voudris V. Evaluation of electronic cigarette use (vaping) topography and estimation of liquid consumption: implications for research protocol standards definition and for public health authorities’ regulation. Int J Environ Res Public Health. 2013;10(6):2500–14.
Mishra A, Chaturvedi P, Datta S, Sinukumar S, Joshi P, Garg A. Harmful effects of nicotine. Indian J Med Paediatr Oncol. 2015;36(1):24–31.
Wang Q, Sundar IK, Li D, Lucas JH, Muthumalage T, McDonough SR, et al. E-cigarette-induced pulmonary inflammation and dysregulated repair are mediated by nAChR α7 receptor: role of nAChR α7 in SARS-CoV-2 Covid-19 ACE2 receptor regulation. Respir Res. 2020;21(1):154.
Lee AC, Chakladar J, Li WT, Chen C, Chang EY, Wang-Rodriguez J, et al. Tobacco, but not nicotine and flavor-less electronic cigarettes, induces ACE2 and immune dysregulation. Int J Mol Sci. 2020;21(15):5513.
Article CAS PubMed Central Google Scholar
England LJ, Bunnell RE, Pechacek TF, Tong VT, McAfee TA. Nicotine and the developing human: a neglected element in the electronic cigarette debate. Am J Prev Med. 2015;49(2):286–93.
Yuan M, Cross SJ, Loughlin SE, Leslie FM. Nicotine and the adolescent brain. J Physiol. 2015;593(16):3397–412.
Holbrook BD. The effects of nicotine on human fetal development. Birth Defects Res C Embryo Today. 2016;108(2):181–92.
Sanner T, Grimsrud TK. Nicotine: carcinogenicity and effects on response to cancer treatment—a review. Front Oncol. 2015;5:196.
Waldum HL, Nilsen OG, Nilsen T, Rørvik H, Syversen V, Sanvik AK, et al. Long-term effects of inhaled nicotine. Life Sci. 1996;58(16):1339–46.
Cucina A, Dinicola S, Coluccia P, Proietti S, D’Anselmi F, Pasqualato A, et al. Nicotine stimulates proliferation and inhibits apoptosis in colon cancer cell lines through activation of survival pathways. J Surg Res. 2012;178(1):233–41.
Wu SY, Xing F, Sharma S, Wu K, Tyagi A, Liu Y, et al. Nicotine promotes brain metastasis by polarizing microglia and suppressing innate immune function. J Exp Med. 2020;217(8):e20191131.
Roemer E, Stabbert R, Rustemeier K, Veltel DJ, Meisgen TJ, Reininghaus W, et al. Chemical composition, cytotoxicity and mutagenicity of smoke from US commercial and reference cigarettes smoked under two sets of machine smoking conditions. Toxicology. 2004;195(1):31–52.
Mayer B. How much nicotine kills a human? Tracing back the generally accepted lethal dose to dubious self-experiments in the nineteenth century. Arch Toxicol. 2014;88(1):5–7.
Brown CJ, Cheng JM. Electronic cigarettes: product characterisation and design considerations. Tob Control. 2014;23(Suppl 2):ii4-10.
Food and Drug Administration. SCOGS (Select Committee on GRAS Substances). 2019 (updated April 29, 2019). https://www.accessdata.fda.gov/scripts/fdcc/index.cfm?set=SCOGS&sort=Sortsubstance&order=ASC&startrow=251&type=basic&search= . Accessed 14 April 2020.
Wieslander G, Norback D, Lindgren T. Experimental exposure to propylene glycol mist in aviation emergency training: acute ocular and respiratory effects. Occup Environ Med. 2001;58(10):649–55.
Choi H, Schmidbauer N, Sundell J, Hasselgren M, Spengler J, Bornehag CG. Common household chemicals and the allergy risks in pre-school age children. PLoS One. 2010;5(10):e13423.
Kienhuis AS, Soeteman-Hernandez LG, Bos PMJ, Cremers HWJM, Klerx WN, Talhout R. Potential harmful health effects of inhaling nicotine-free shisha-pen vapor: a chemical risk assessment of the main components propylene glycol and glycerol. Tob Induc Dis. 2015;13(1):15.
Renne RA, Wehner AP, Greenspan BJ, Deford HS, Ragan HA, Westerberg RB, et al. 2-Week and 13-week inhalation studies of aerosolized glycerol in rats. Inhal Toxicol. 1992;4(2):95–111.
Article CAS Google Scholar
Behar R, Wang Y, Talbot P. Comparing the cytotoxicity of electronic cigarette fluids, aerosols and solvents. Tob Control. 2018;27(3):325.
Massarsky A, Abdel A, Glazer L, Levin ED, Di Giulio RT. Neurobehavioral effects of 1,2-propanediol in zebrafish (Danio rerio). Neurotoxicology. 2018;65:111–24.
Geiss O, Bianchi I, Barrero-Moreno J. Correlation of volatile carbonyl yields emitted by e-cigarettes with the temperature of the heating coil and the perceived sensorial quality of the generated vapours. Int J Hyg Environ Health. 2016;219(3):268–77.
Counts ME, Morton MJ, Laffoon SW, Cox RH, Lipowicz PJ. Smoke composition and predicting relationships for international commercial cigarettes smoked with three machine-smoking conditions. Regul Toxicol Pharmacol. 2005;41(3):185–227.
Agency for Toxic Substances & Disease Registry. Toxicological Profile for Formaldehyde. 2019 (updated September 26, 2019). https://www.atsdr.cdc.gov/ToxProfiles/tp.asp?id=220&tid=39 . Accessed 9 April 2020.
Agency for Toxic Substances & Disease Registry. Toxicological Profile for Acrolein. 2019 (updated September 26, 2019). https://www.atsdr.cdc.gov/toxprofiles/TP.asp?id=557&tid=102 . Accessed 9 April 2020
Moghe A, Ghare S, Lamoreau B, Mohammad M, Barve S, McClain C, et al. Molecular mechanisms of acrolein toxicity: relevance to human disease. Toxicol Sci. 2015;143(2):242–55.
Seitz HK, Stickel F. Acetaldehyde as an underestimated risk factor for cancer development: role of genetics in ethanol metabolism. Genes Nutr. 2010;5(2):121–8.
Faroon O, Roney N, Taylor J, Ashizawa A, Lumpkin MH, Plewak DJ. Acrolein health effects. Toxicol Ind Health. 2008;24(7):447–90.
Goniewicz ML, Knysak J, Gawron M, Kosmider L, Sobczak A, Kurek J, et al. Levels of selected carcinogens and toxicants in vapour from electronic cigarettes. Tob Control. 2014;23(2):133–9.
Farsalinos KE, Voudris V. Do flavouring compounds contribute to aldehyde emissions in e-cigarettes? Food Chem Toxicol. 2018;115:212–7.
Kavvalakis MP, Stivaktakis PD, Tzatzarakis MN, Kouretas D, Liesivuori J, Alegakis AK, et al. Multicomponent analysis of replacement liquids of electronic cigarettes using chromatographic techniques. J Anal Toxicol. 2015;39(4):262–9.
Etter JF, Zather E, Svensson S. Analysis of refill liquids for electronic cigarettes. Addiction. 2013;108(9):1671–9.
Etter JF, Bugey A. E-cigarette liquids: constancy of content across batches and accuracy of labeling. Addict Behav. 2017;73:137–43.
Varlet V, Farsalinos K, Augsburger M, Thomas A, Etter JF. Toxicity assessment of refill liquids for electronic cigarettes. Int J Environ Res Public Health. 2015;12(5):4796–815.
McAuley TR, Hopke PK, Zhao J, Babaian S. Comparison of the effects of e-cigarette vapor and cigarette smoke on indoor air quality. Inhal Toxicol. 2012;24(12):850–7.
Cullen KA, Gentzke AS, Sawdey MD, Chang JT, Anic GM, Wang TW, et al. e-Cigarette use among youth in the United States, 2019. JAMA. 2019;322(21):2095–103.
Villanti AC, Johnson AL, Ambrose BK, Cummings KM, Stanton CA, Rose SW, et al. Flavored tobacco product use in youth and adults: findings from the first wave of the PATH Study (2013–2014). Am J Prev Med. 2017;53(2):139–51.
Food and Drug Administration. Vaporizers, E-Cigarettes, and other Electronic Nicotine Delivery Systems (ENDS) 2020 (updated April 13, 2020). https://www.fda.gov/tobacco-products/products-ingredients-components/vaporizers-e-cigarettes-and-other-electronic-nicotine-delivery-systems-ends . Accessed 15 April 2020
Omaiye EE, McWhirter KJ, Luo W, Tierney PA, Pankow JF, Talbot P. High concentrations of flavor chemicals are present in electronic cigarette refill fluids. Sci Rep. 2019;9(1):2468.
Bahl V, Lin S, Xu N, Davis B, Wang YH, Talbot P. Comparison of electronic cigarette refill fluid cytotoxicity using embryonic and adult models. Reprod Toxicol. 2012;34(4):529–37.
Behar R, Davis B, Wang Y, Bahl V, Lin S, Talbot P. Identification of toxicants in cinnamon-flavored electronic cigarette refill fluids. Toxicol In Vitro. 2014;28(2):198–208.
Morgan DL, Flake GP, Kirby PJ, Palmer SM. Respiratory toxicity of diacetyl in C57BL/6 mice. Toxicol Sci. 2008;103(1):169–80.
Hubbs AF, Cumpston AM, Goldsmith WT, Battelli LA, Kashon ML, Jackson MC, et al. Respiratory and olfactory cytotoxicity of inhaled 2,3-pentanedione in Sprague-Dawley rats. Am J Pathol. 2012;181(3):829–44.
Vas CA, Porter A, Mcadam K. Acetoin is a precursor to diacetyl in e-cigarette liquids. Food Chem Toxicol. 2019;133:110727.
Allen JG, Flanigan SS, LeBlanc M, Vallarino J, MacNaughton P, Stewart JH, et al. Flavoring chemicals in E-cigarettes: diacetyl, 2,3-pentanedione, and acetoin in a sample of 51 products, including fruit-, candy-, and cocktail-flavored E-cigarettes. Environ Health Perspect. 2016;124(6):733–9.
Park RM, Gilbert SJ. Pulmonary impairment and risk assessment in a diacetyl-exposed population: microwave popcorn workers. J Occup Environ Med. 2018;60(6):496–506.
Muthumalage T, Prinz M, Ansah KO, Gerloff J, Sundar IK, Rahman I. Inflammatory and oxidative responses induced by exposure to commonly used e-cigarette flavoring chemicals and flavored e-liquids without nicotine. Front Physiol. 2017;8:1130.
Sherwood CL, Boitano S. Airway epithelial cell exposure to distinct e-cigarette liquid flavorings reveals toxicity thresholds and activation of CFTR by the chocolate flavoring 2,5-dimethypyrazine. Respir Res. 2016;17(1):57.
Pinkston R, Zaman H, Hossain E, Penn AL, Noël A. Cell-specific toxicity of short-term JUUL aerosol exposure to human bronchial epithelial cells and murine macrophages exposed at the air–liquid interface. Respir Res. 2020;21(1):269.
Williams M, Villarreal A, Bozhilov K, Lin S, Talbot P. Metal and silicate particles including nanoparticles are present in electronic cigarette cartomizer fluid and aerosol. PLoS One. 2013;8(3):e57987.
Mikheev VB, Brinkman MC, Granville CA, Gordon SM, Clark PI. Real-time measurement of electronic cigarette aerosol size distribution and metals content analysis. Nicotine Tob Res. 2016;18(9):1895–902.
Williams M, Bozhilov K, Ghai S, Talbot P. Elements including metals in the atomizer and aerosol of disposable electronic cigarettes and electronic hookahs. PLoS One. 2017;12(4):e0175430.
Kleinman MT, Arechavala RJ, Herman D, Shi J, Hasen I, Ting A, et al. E-cigarette or vaping product use-associated lung injury produced in an animal model from electronic cigarette vapor exposure without tetrahydrocannabinol or vitamin E oil. J Am Heart Assoc. 2020;9(18):e017368.
Patnode CD, Henderson JT, Thompson JH, Senger CA, Fortmann SP, Whitlock EP. Behavioral counseling and pharmacotherapy interventions for tobacco cessation in adults, including pregnant women: a review of reviews for the U.S. preventive services task force. Ann Intern Med. 2015;163(8):608–21.
Messner B, Bernhard D. Smoking and cardiovascular disease: mechanisms of endothelial dysfunction and early atherogenesis. Arterioscler Thromb Vasc Biol. 2014;34(3):509–15.
Bansal V, Kim K-H. Review on quantitation methods for hazardous pollutants released by e-cigarette (EC) smoking. Trends Analyt Chem. 2016;78:120–33.
Mantey DS, Pasch KE, Loukas A, Perry CL. Exposure to point-of-sale marketing of cigarettes and E-cigarettes as predictors of smoking cessation behaviors. Nicotine Tob Res. 2019;21(2):212–9.
Selya AS, Dierker L, Rose JS, Hedeker D, Mermelstein RJ. The role of nicotine dependence in E-cigarettes’ potential for smoking reduction. Nicotine Tob Res. 2018;20(10):1272–7.
Kalkhoran S, Glantz SA. E-cigarettes and smoking cessation in real-world and clinical settings: a systematic review and meta-analysis. Lancet Respir Med. 2016;4(2):116–28.
Levy DT, Yuan Z, Luo Y, Abrams DB. The relationship of e-cigarette use to cigarette quit attempts and cessation: insights from a large, nationally representative U.S. survey. Nicotine Tob Res. 2017;20(8):931–9.
Article PubMed Central Google Scholar
Hajek P, Phillips-Waller A, Przulj D, Pesola F, Myers Smith K, Bisal N, et al. A randomized trial of E-cigarettes versus nicotine-replacement therapy. N Engl J Med. 2019;380(7):629–37.
Polosa R, Morjaria JB, Caponnetto P, Prosperini U, Russo C, Pennisi A, et al. Evidence for harm reduction in COPD smokers who switch to electronic cigarettes. Respir Res. 2016;17(1):166.
Litt MD, Duffy V, Oncken C. Cigarette smoking and electronic cigarette vaping patterns as a function of e-cigarette flavourings. Tob Control. 2016;25(Suppl 2):ii67–72.
Palmer AM, Brandon TH. How do electronic cigarettes affect cravings to smoke or vape? Parsing the influences of nicotine and expectancies using the balanced-placebo design. J Consult Clin Psychol. 2018;86(5):486–91.
Majmundar A, Allem JP, Cruz TB, Unger JB. Public health concerns and unsubstantiated claims at the intersection of vaping and COVID-19. Nicotine Tob Res. 2020;22(9):1667–8.
Berlin I, Thomas D, Le Faou A-L, Cornuz J. COVID-19 and smoking. Nicotine Tob Res. 2020;22(9):1650–2.
Wrapp D, Wang N, Corbett KS, Goldsmith JA, Hsieh C-L, Abiona O, et al. Cryo-EM structure of the 2019-nCoV spike in the prefusion conformation. Science. 2020;367(6483):1260–3.
Wang K, Gheblawi M, Oudit GY. Angiotensin Converting Enzyme 2: A Double-Edged Sword. Circulation. 2020;142(5):426–8.
Sharma P, Zeki AA. Does vaping increase susceptibility to COVID-19? Am J Respir Crit Care Med. 2020;202(7):1055–6.
Brake SJ, Barnsley K, Lu W, McAlinden KD, Eapen MS, Sohal SS. Smoking upregulates angiotensin-converting enzyme-2 receptor: a potential adhesion site for novel coronavirus SARS-CoV-2 (Covid-19). J Clin Med. 2020;9(3):841.
Zhang H, Rostamim MR, Leopold PL, Mezey JG, O’Beirne SL, Strulovici-Barel Y, et al. Reply to sharma and zeki: does vaping increase susceptibility to COVID-19? Am J Respir Crit Care Med. 2020;202(7):1056–7.
Cheng H, Wang Y, Wang GQ. Organ-protective effect of angiotensin-converting enzyme 2 and its effect on the prognosis of COVID-19. J Med Virol. 2020;92(7):726–30.
Lerner CA, Sundar IK, Yao H, Gerloff J, Ossip DJ, McIntosh S, et al. Vapors produced by electronic cigarettes and e-juices with flavorings induce toxicity, oxidative stress, and inflammatory response in lung epithelial cells and in mouse lung. PLoS ONE. 2015;10(2):e0116732.
Download references
Acknowledgements
The authors gratefully acknowledge Dr. Cruz González, Pulmonologist at University Clinic Hospital of Valencia (Valencia, Spain) for her thoughtful suggestions and support.
This work was supported by the Spanish Ministry of Science and Innovation [Grant Number SAF2017-89714-R]; Carlos III Health Institute [Grant Numbers PIE15/00013, PI18/00209]; Generalitat Valenciana [Grant Number PROMETEO/2019/032, Gent T CDEI-04/20-A and AICO/2019/250], and the European Regional Development Fund.
Author information
Authors and affiliations.
Department of Pharmacology, Faculty of Medicine, University of Valencia, Avda. Blasco Ibañez 15, 46010, Valencia, Spain
Patrice Marques, Laura Piqueras & Maria-Jesus Sanz
Institute of Health Research INCLIVA, University Clinic Hospital of Valencia, Valencia, Spain
CIBERDEM-Spanish Biomedical Research Centre in Diabetes and Associated Metabolic Disorders, ISCIII, Av. Monforte de Lemos 3-5, 28029, Madrid, Spain
Laura Piqueras & Maria-Jesus Sanz
You can also search for this author in PubMed Google Scholar
Contributions
All authors discussed and agreed to the scope of the manuscript and contributed to the development of the manuscript at all stages. All authors read and approved the final manuscript.
Corresponding author
Correspondence to Maria-Jesus Sanz .
Ethics declarations
Ethics approval and consent to participate, consent for publication, competing interests.
The authors of the manuscript declare no conflicts of interest and take sole responsibility for the writing and content of the manuscript. None of the authors have been involved in legal or regulatory matters related to the contents of this paper.
Additional information
Publisher's note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Reprints and permissions
About this article
Cite this article.
Marques, P., Piqueras, L. & Sanz, MJ. An updated overview of e-cigarette impact on human health. Respir Res 22 , 151 (2021). https://doi.org/10.1186/s12931-021-01737-5
Download citation
Received : 22 October 2020
Accepted : 03 May 2021
Published : 18 May 2021
DOI : https://doi.org/10.1186/s12931-021-01737-5
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Electronic cigarette
- E-cigarette
- Flavourings
- Smoking cessation tool
Respiratory Research
ISSN: 1465-993X
- General enquiries: [email protected]

An official website of the United States government
Here’s how you know
Official websites use .gov A .gov website belongs to an official government organization in the United States.
Secure .gov websites use HTTPS A lock ( A locked padlock ) or https:// means you’ve safely connected to the .gov website. Share sensitive information only on official, secure websites.
- Heart-Healthy Living
- High Blood Pressure
- Sickle Cell Disease
- Sleep Apnea
- Information & Resources on COVID-19
- The Heart Truth®
- Learn More Breathe Better®
- Blood Diseases & Disorders Education Program
- Publications and Resources
- Clinical Trials and Studies
- Blood Disorders and Blood Safety
- Sleep Science and Sleep Disorders
- Lung Diseases
- Health Disparities and Inequities
- Heart and Vascular Diseases
- Precision Medicine Activities
- Obesity, Nutrition, and Physical Activity
- Population and Epidemiology Studies
- Women’s Health
- Research Topics
- All Science A-Z
- Grants and Training Home
- Policies and Guidelines
- Funding Opportunities and Contacts
- Training and Career Development
- Email Alerts
- NHLBI in the Press
- Research Features
- Ask a Scientist
- Past Events
- Upcoming Events
- Mission and Strategic Vision
- Divisions, Offices and Centers
- Advisory Committees
- Budget and Legislative Information
- Jobs and Working at the NHLBI
- Contact and FAQs
- NIH Sleep Research Plan
- News and Events
- < Back To All News
NIH-funded studies show damaging effects of vaping, smoking on blood vessels

Combining e-cigarettes with regular cigarettes may increase health risks
Long-term use of electronic cigarettes, or vaping products, can significantly impair the function of the body’s blood vessels, increasing the risk for cardiovascular disease. Additionally, the use of both e-cigarettes and regular cigarettes may cause an even greater risk than the use of either of these products alone. These findings come from two new studies supported by the National Heart, Lung, and Blood Institute (NHLBI), part of the National Institutes of Health (NIH).
The findings, which appear today in the journal Arteriosclerosis, Thrombosis, and Vascular Biology , add to growing evidence that long-term use of e-cigarettes can harm a person’s health. Researchers have known for years that tobacco smoking can cause damage to blood vessels. However, the effects of e-cigarettes on cardiovascular health have been poorly understood. The two new studies – one on humans, the other on rats – aimed to change that.
“In our human study, we found that chronic e-cigarettes users had impaired blood vessel function, which may put them at increased risk for heart disease,” said Matthew L. Springer, Ph.D., a professor of medicine in the Division of Cardiology at the University of California in San Francisco, and leader of both studies. “It indicates that chronic users of e-cigarettes may experience a risk of vascular disease similar to that of chronic smokers.”
In this first study, Springer and his colleagues collected blood samples from a group of 120 volunteers that included those with long-term e-cigarette use, long-term cigarette smoking, and those who didn't use. The researchers defined long-term e-cigarette use as more than five times/week for more than three months and defined long-term cigarette use as smoking more than five cigarettes per day.
They then exposed each of the blood samples to cultured human blood vessel (endothelial) cells in the laboratory and measured the release of nitric oxide, a chemical marker used to evaluate proper functioning of endothelial cells. They also tested cell permeability, the ability of molecules to pass through a layer of cells to the other side. Too much permeability makes vessels leaky, which impairs function and increases the risk for cardiovascular disease.
The researchers found that blood from participants who used e-cigarettes and those who smoked caused a significantly greater decrease in nitric oxide production by the blood vessel cells than the blood of nonusers. Notably, the researchers found that blood from those who used e-cigarettes also caused more permeability in the blood vessel cells than the blood from both those who smoked cigarettes and nonusers. Blood from those that used e-cigarettes also caused a greater release of hydrogen peroxide by the blood vessel cells than the blood of the nonusers. Each of these three factors can contribute to impairment of blood vessel function in people who use e-cigarettes, the researchers said.
In addition, Springer and his team discovered that e-cigarettes had harmful cardiovascular effects in ways that were different from those caused by tobacco smoke. Specifically, they found that blood from people who smoked cigarettes had higher levels of certain circulating biomarkers of cardiovascular risks, and the blood people who used e-cigarettes had elevated levels of other circulating biomarkers of cardiovascular risks.
“These findings suggest that using the two products together, as many people do, could increase their health risks compared to using them individually,” Springer said. “We had not expected to see that.”
In the second study, the researchers tried to find out if there were specific components of cigarette smoke or e-cigarette vapor that were responsible for blood vessel damage. In studies using rats, they exposed the animals to various substances found in tobacco smoke or e-cigarettes. These included nicotine, menthol (a cigarette additive), the gases acrolein and acetaldehyde (two chemicals found in both tobacco smoke and e-cigarette vapors), and inert carbon nanoparticles to represent the particle-like nature of smoke and e-cigarette vapor.
Using special arterial flow measurements, the researchers demonstrated that blood vessel damage does not appear to be caused by a specific component of cigarette smoke or e-cigarette vapor. Instead, they said, it appears to be caused by airway irritation that triggers biological signals in the vagus nerve that somehow leads to blood vessel damage, possibly through an inflammatory process. The vagus is a long nerve extending from the brain that connects the airway to the rest of the nervous system and plays a key role in heart rate, breathing, and other functions. The researchers showed that detaching the nerve in rats prevented blood vessel damage caused by tobacco smoke, demonstrating its key role in this process.
“We were surprised to find that there was not a single component that you could remove to stop the damaging effect of smoke or vapors on the blood vessels,” Springer said. “As long as there’s an irritant in the airway, blood vessel function may be impaired.”
The finding has implications for efforts to regulate tobacco products and e-cigarettes, as it underscores how difficult it is to pinpoint any one ingredient in them that is responsible for blood vessel damage. “What I like to tell people is this: Just breathe clean air and avoid using these products,” Springer said.
Lisa Postow, Ph.D., an NHLBI program officer in NHLBI’s Division of Lung Diseases, agreed that the study results “provide further evidence that exposure to e-cigarettes could lead to harmful cardiovascular health effects.” She added that more data is needed to fully understand the health effects of e-cigarettes. The NIH and others are continuing to explore this area.
Research reported in the e-cigarette study was funded by NHLBI grants U54HL147127, P50HL120163, and R01HL120062 and the U.S. Food and Drug Administration Center for Tobacco Products (FDA CTP); and grant P50CA180890 from the National Cancer Institute at the NIH and FDA CTP. Research reported in the cigarette smoke/-vagal nerve study was supported by NHLBI grants R01HL120062 and U54HL147127 and FDA CTP and grant P50CA180890 from the National Cancer Institute at the NIH and FDA CTP. For additional funding details, please see the full journal articles.
Study: Chronic e-cigarette use impairs endothelial function on the physiological and cellular levels. Arteriosclerosis, Thrombosis, and Vascular Biology. DOI: 10.1161/ATVBAHA.121.317749
Study: Impairment of Endothelial Function by Cigarette Smoke is not Caused by a Specific Smoke Constituent, but by Vagal Input from the Airway. Arteriosclerosis, Thrombosis, and Vascular Biology. DOI: 10.1161/ATVBAHA.122.318051
About the National Heart, Lung, and Blood Institute (NHLBI): NHLBI is the global leader in conducting and supporting research in heart, lung, and blood diseases and sleep disorders that advances scientific knowledge, improves public health, and saves lives. For more information, visit www.nhlbi.nih.gov .
About the National Institutes of Health (NIH): NIH, the nation's medical research agency, includes 27 Institutes and Centers and is a component of the U.S. Department of Health and Human Services. NIH is the primary federal agency conducting and supporting basic, clinical, and translational medical research, and is investigating the causes, treatments, and cures for both common and rare diseases. For more information about NIH and its programs, visit www.nih.gov .
More Information
Related health topics, health education.
Thank you for visiting nature.com. You are using a browser version with limited support for CSS. To obtain the best experience, we recommend you use a more up to date browser (or turn off compatibility mode in Internet Explorer). In the meantime, to ensure continued support, we are displaying the site without styles and JavaScript.
- View all journals
- My Account Login
- Explore content
- About the journal
- Publish with us
- Sign up for alerts
- Open access
- Published: 22 October 2022
A systematic review of the effects of e-cigarette use on lung function
- Lucy Honeycutt 1 ,
- Katherine Huerne 1 , 2 ,
- Alanna Miller 1 ,
- Erica Wennberg 1 ,
- Kristian B. Filion 1 , 3 ,
- Roland Grad 1 , 4 ,
- Andrea S. Gershon 5 ,
- Carolyn Ells ORCID: orcid.org/0000-0002-4593-454X 1 , 2 , 4 ,
- Genevieve Gore 6 ,
- Andrea Benedetti 3 , 7 ,
- Brett Thombs 1 , 3 , 8 &
- Mark J. Eisenberg ORCID: orcid.org/0000-0002-1296-0661 1 , 3 , 9
npj Primary Care Respiratory Medicine volume 32 , Article number: 45 ( 2022 ) Cite this article
21k Accesses
12 Citations
40 Altmetric
Metrics details
- Epidemiology
Given the increasing use of e-cigarettes and uncertainty surrounding their safety, we conducted a systematic review to determine the effects of e-cigarettes on measures of lung function. We systematically searched EMBASE, MEDLINE, and PsycINFO databases via Ovid, the Cochrane CENTRAL database, and the Web of Science Core from 2004 until July 2021, identifying 8856 potentially eligible studies. A total of eight studies (seven studying immediate effects and one long-term effects, 273 total participants) were included. The risk of bias was assessed using the Risk of Bias in Non-randomized Studies—of Interventions (ROBINS-I) and Cochrane risk of bias tools. These studies suggest that vaping increases airway resistance but does not appear to impact forced expiratory volume in one second (FEV 1) , forced vital capacity (FVC), or FEV 1 /FVC ratio. However, given the limited size and follow-up duration of these studies, larger, long-term studies are required to further determine the effects of e-cigarettes on lung function.
Similar content being viewed by others
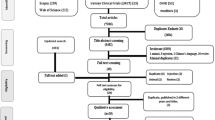
Efficacy and safety of inhaled heparin in asthmatic and chronic obstructive pulmonary disease patients: a systematic review and a meta-analysis
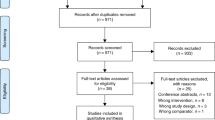
Are COPD self-management mobile applications effective? A systematic review and meta-analysis
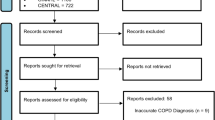
Wearable technology interventions in patients with chronic obstructive pulmonary disease: a systematic review and meta-analysis
Introduction.
The first electronic cigarette (e-cigarette) was patented and marketed in 2004 1 . Since then, e-cigarette use (or “vaping”) has grown exponentially across the globe 2 . As the use of vaping devices evolves with policy, the consequences of vaping on health are becoming an increasingly important public health issue. E-cigarettes are being studied for harm reduction in individuals who use cigarettes and as a smoking cessation aid, as they are believed to be less harmful to health than smoking 3 . However, there is increasing evidence demonstrating adverse respiratory effects of vaping compared to vaping abstinence. In particular, an outbreak of E-Cigarette and Vaping-Associated Lung Illness (EVALI) brought the short-term respiratory consequences of vaping into question, especially if cannabis or THC-containing products are used 4 . Other short-term respiratory changes that have been linked to vaping include increased airway resistance 5 , breathing difficulty 6 , and transient lung inflammation 7 . Vaping has also been associated with chronic respiratory conditions such as asthma 8 and chronic bronchitis 9 . Despite these reports, the short- and long-term respiratory safety of vaping is still largely unknown. Several small studies have examined the effects of e-cigarettes on lung function, including measures such as forced expiratory volume in one second (FEV 1 ), forced vital capacity (FVC), and airway resistance. However, no evidence syntheses have been completed on this topic. Therefore, we conducted a systematic review to determine the effects of vaping on measures of lung function.
Our systematic review was conducted following a protocol developed prior to initiating the review, which was registered on the PROSPERO register of systematic reviews ( CRD42021227121 ) 10 . This systematic review is reported following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines 11 .
Search strategy and study selection
Using a search strategy (Supplementary Tables 1 – 5 ) developed by an experienced health sciences librarian (G.G.), we systematically searched EMBASE, MEDLINE, and PsycINFO databases via Ovid, the Cochrane CENTRAL database, and the Web of Science Core from 2004 (the year of the first e-cigarette patent) until July 12, 2021. We additionally conducted a gray literature search by searching the websites of key governmental and public health organizations (the World Health Organization, Health Canada, the US Centers for Disease Control and Prevention, the US Food and Drug Administration, the Canadian Center on Substance Use and Addiction, the European Centre for Disease Prevention and Control, and the European Public Health Association). Additional articles were identified by manually searching the reference lists of included publications as well as SCOPUS and Google Scholar (first ten pages). Articles were included if they reported quantitative primary data on changes in lung function associated with vaping, defined as the use of any device that functions by transforming an e-liquid to an aerosol using metal coils, among human participants of any age. Studies of cells and those conducted in animals were excluded. Studies using heat-not-burn devices were also excluded, as these do not meet the above definition of vaping. Eligible studies included randomized controlled trials (RCTs), non-randomized studies of interventions (NRSIs), and cohort studies; cross-sectional studies and case reports were excluded. We included studies that used non-users of both vaping devices and conventional cigarettes as a comparison group and those that used a pre- and post-design in which individuals acted as their own controls. Inclusion was not restricted by language or country of publication. Abstracts and conference proceedings were included if sufficient data could be extracted from these publications.
Search results were downloaded from databases into reference management software (EndNote X9) or manually added (e.g., for gray literature results). Duplicates were removed in EndNote and entries were uploaded to Covidence (Veritas Health Innovation, Melbourne, Australia), a systematic review software. Two reviewers (L.H. and K.H.) independently screened the titles and abstracts of all identified publications for eligibility. Citations considered potentially eligible by either reviewer, based on the pre-specified review inclusion/exclusion criteria (Supplementary Table 6 ), were retrieved for full-text screening and assessed for inclusion. The reasons for exclusion after full-text review were annotated in Covidence and any disagreements were resolved by consensus or a third reviewer (A.H-L.).
Data extraction
Two independent reviewers (L.H and K.H.) extracted methodological, demographic, and outcome data from included studies in duplicate; disagreements were detected in Covidence and were resolved by consensus or, if necessary, by a third reviewer (A.H-L.). Extracted data included study characteristics (first author, journal, year of publication, years(s) of data collection, funding, data source, study design, recruitment strategy, duration of follow-up, country of origin, sample size); population characteristics (sex, gender, age, race, ethnicity, socioeconomic status, dose/frequency of e-cigarette use, conventional cigarette smoking status, smoked cannabis use); and vaping behavior, including the type of vaping device used (e.g., disposable e-cigarette vs. pod device such as JUUL), vaping products used (e.g., nicotine cartridges exclusively vs. THC cartridges exclusively vs. dual use of nicotine and THC products), and source of the vaping product (informal [i.e., friends, family members, or dealers] vs. commercial [i.e., vape shops, stores, dispensaries]).
Initially, extracted outcomes of primary interest were respiratory signs and symptoms, as these are important to patients and are the early signs of respiratory disease. Secondary outcomes included: findings on lung function; Computed tomography (CT) findings of emphysema, airway remodeling, and small airway loss; respiratory-related quality of life and exercise limitations; incidence and/or prevalence of respiratory disease as well as exacerbations of previous respiratory disease; and health care resource use including respiratory disease-related ambulatory care, emergency department visits, and hospitalization. Given the limited number of studies available and the heterogeneity of the data extracted from these studies, no meta-analysis was conducted.
Risk of bias
The risk of bias in included publications was assessed independently by two reviewers (L.H. and K.H.), and discrepancies were resolved by consensus or, if necessary, by a third reviewer (A.H-L.). The risk of bias of included non-randomized studies (pre-post studies, NRSI with non-vaping reference group, cohort study) was assessed using the Risk of Bias in Non-randomized Studies—of Interventions (ROBINS-I) tool 12 . The ROBINS-I tool evaluates intervention-specific outcomes for a study through seven domains which assess the risk of bias pre-intervention, at-intervention, and post-intervention. For each outcome of interest extracted from an included study, the risk of bias within each domain was reported as “low”, “moderate”, “serious”, or “critical”. Included RCTs were assessed using the Cochrane Collaboration’s Tool for Assessing Risk of Bias (ROB V1) 13 . Similar to ROBINS-I, this tool evaluates the risk of bias through the assessment of five domains; for each outcome of interest extracted from an included study, the risk of bias for each domain was reported as “low risk of bias”, “high risk of bias”, or “unclear risk of bias.” All eligible publications were included in the qualitative synthesis regardless of their assessed risk of bias.
Reporting summary
Further information on research design is available in the Nature Research Reporting Summary linked to this article.
As our search did not identify studies which focused on the broad outcomes detailed above, we chose to limit our focus to studies on lung function. Our database searches identified 14,307 potentially eligible studies (Fig. 1 ). After duplicates were removed, 8856 titles and abstracts were assessed. After this initial screening, 44 full texts were retrieved and reviewed in further detail, yielding eight studies eligible for inclusion.
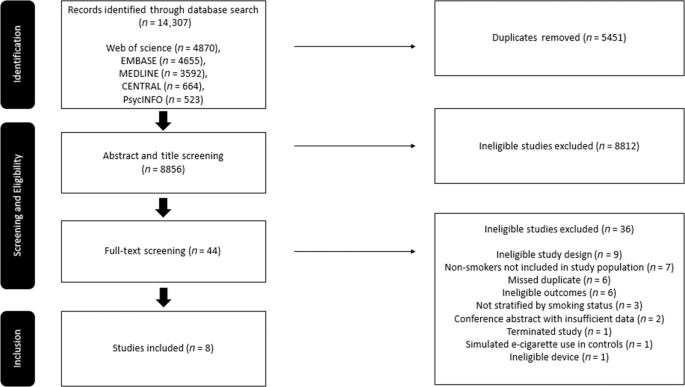
PRISMA flow diagram of included studies assessing the effect of e-cigarettes on lung function.
Study and participant characteristics
Of the eight included studies (273 total participants), seven 14 , 15 , 16 , 17 , 18 , 19 , 20 involved short-term exposure to e-cigarettes with immediate outcome assessment, and the remaining study followed vapers and non-vapers over 3.5 years 21 (Table 1 ). This prospective cohort study examined 21 participants (12 nonsmokers and nine vapers) at means of 12 (standard deviation: 1), 24 (2), and 42 (2) months after baseline 21 . Of the seven short-term studies, four were NRSIs (three pre-post studies 14 , 15 , 16 and one NRSI with a non-vaping reference group 20 ) and three were RCTs 17 , 18 , 19 . Among these seven studies, two included 70–80 participants 14 , 15 and five included 10–30 participants 16 , 17 , 18 , 19 , 20 . Exposures varied in terms of e-cigarettes, e-liquids, and vaping session timings. Most studies did not expand on their definition of “non-smoker/non-vaper” 15 , 16 , 18 , 19 , 20 , 21 , but two studies clarified that these participants were never-smokers 14 , 17 . One of these two studies further elaborated that participants had no exposure to tobacco products or e-cigarettes 17 . Few studies gave detailed information on the type of e-cigarette used. Three studies reported a specific brand or product (Blu 17 , eGo 16 , Joytech elips-C series 18 , Puff bar 20 ). Polosa et al. listed some of the various e-cigarettes used by participants throughout the longitudinal study, including standard refillable (eGo style products) and more advanced refillable (Provari, Innokin, Joytech, eVIC, Avatar Puff) 21 . The remaining studies did not report a specific brand, though one study described the e-cigarette used as a “1 st generation e-cigarette popular in Greece” 15 . All studies clarified whether the e-cigarettes used during the study contained nicotine.
The included RCTs ( n = 3) 17 , 18 , 19 had an unclear risk of bias, with each study demonstrating an unclear risk of bias in 3+ domains (Table 2 ). This was primarily due to missing information in the manuscripts required to make an adequate judgment, such as a lack of detail surrounding randomization. The risk associated with the blinding of participants and personnel was judged to be low for all 3 included RCTs. These studies were not blinded, and one was placebo-controlled. However, it was judged that this lack of blinding would not influence measures of lung function. Of the included non-randomized studies ( n = 5) 14 , 15 , 16 , 20 , 21 , four 14 , 15 , 16 , 20 were judged to be at moderate risk of bias and one 21 was found to have a serious risk of bias (Table 3 ). The most consistent source of bias in these studies was bias due to confounding, with only one 16 study judged to have a low risk of bias due to confounding. Of the remaining four studies, three 14 , 15 , 20 were found to have a moderate risk of bias due to confounding and one 21 was found to be at serious risk of bias due to confounding, with important confounding variables not accounted for in the design or analysis.
Effects of E-cigarette use on lung function
Seven studies 14 , 15 , 16 , 17 , 18 , 19 , 20 reported immediate measures of lung function after short-term exposure to e-cigarettes (Table 4 ), including FEV 1 , FVC, and FEV 1 /FVC. Two studies, Boulay et al. and Staudt. et al. suggested no changes in FEV 1 or FEV 1 /FVC after vaping among nonsmokers 17 , 19 . Kizhakke Puliyakote et al. observed lower baseline FEV 1 and FEV 1 /FVC values among nonsmokers compared to vapers 20 . Coppeta et al. found a decrease in FEV 1 and FEV 1 /FVC among nonsmokers after 1 min of vaping; however, these values returned to baseline after 15 min 16 .
Airway resistance and specific airway conductance after 10 min of vaping were measured in two 14 , 15 of the seven short-term studies (Table 4 ). Both Palamidas et al. 2013 and 2017 suggested that vaping increased airway resistance and decreased specific airway conductance among nonsmokers and smokers with and without respiratory disease. Oxygen saturation was assessed in four studies 15 , 17 , 19 , 20 . Three studies suggested no changes after vaping, with only Palamidas et. al. 2017 suggesting decreased oxygen saturation following vaping among smokers with and without asthma 15 .
Long-term changes (3.5 years) in lung function measurements were assessed in only one small ( n = 21) study (Polosa 2017) 21 . This study suggested that FEV 1 , FVC, FEV 1 /FVC, and forced mid-expiratory flow (FEF 25-75 ) did not change over time among vapers and non-vapers (Table 5 ).
This systematic review was designed to determine the effect of vaping on measures of lung function. We found that there were only eight studies in the literature assessing this issue, all of which were small, and only one examined longer-term outcomes (3.5 years follow-up). In general, these studies suggest that there are no acute changes associated with vaping. However, airway resistance and conductance may be influenced by e-cigarettes, with two studies reporting changes in these values in multiple population subgroups. It is important to note that there were few studies available for this systematic review and that most of these studies focused on the acute effects of vaping; therefore, these results are suggestive but not definitive, and future research must be conducted in this area. Furthermore, three of the included studies had an unclear risk of bias, four had a moderate risk of bias, and one had a serious risk of bias, which further limits the interpretation of this review’s findings.
In addition to the limitations above, this review lacks subgroup analyses or a meta-analysis. This is due to the heterogeneity of the included studies, both in terms of study design and outcomes. Few studies were eligible for this review due to the variation in study designs and definitions of e-cigarettes and smoking status. For example, some studies included both conventional cigarette smokers and nonsmokers in their definition of “non-vapers” and did not analyze data separately based on conventional smoking status. Other studies used a “sham” vaping session for controls where either an e-cigarette with an empty cartridge (i.e., without e-liquid) or second-hand smoke were used. More commonly, studies were conducted on smokers only, without nonsmokers as a comparison group. Future studies could analyze subgroups based on both smoking and vaping status to allow for a more detailed quantitative analysis.
E-cigarettes are becoming more popular for recreational use and are being studied for harm reduction among smokers as a smoking cessation aid, as they are believed to be less harmful to health than smoking. However, there are limited data available and virtually no long-term studies assessing how prolonged e-cigarette use could impact lung function. As the use of vaping devices evolves and becomes more widespread, the health consequences of vaping are becoming an increasingly important public health issue. This is a knowledge gap that must be addressed. Knowledge of the safety of e-cigarettes, particularly their long-term safety, will inform public health policy and e-cigarette regulations, as well as the guidance clinicians, offer to their patients on smoking harm reduction. For these policies, regulations, and guidelines to be developed, we must understand how e-cigarettes can influence one’s health. This includes establishing the effects of e-cigarettes on clinical outcomes such as respiratory symptoms (cough, dyspnea), measures of lung function, and risk of developing respiratory disease. Further research is required to elucidate the short- and long-term consequences of vaping to determine whether e-cigarettes are truly a “safer” alternative to traditional cigarettes for smoking cessation or for recreational use. Future studies should be long-term, have large sample sizes, and may include different types of e-cigarettes as well as conventional cigarettes for comparison. In addition, it is important for future research to include clinical outcomes as described above. This will allow for better translation of the research findings to help inform clinical decision-making.
Data availability
No additional data were available, as this study is a knowledge synthesis that relied on aggregate, published results available in the public domain. Any inquiries should be directed to the corresponding author.
Foulds, J., Veldheer, S. & Berg, A. Electronic cigarettes (e‐cigs): views of aficionados and clinical/public health perspectives. Int. J. Clin. Pract. 65 , 1037–1042 (2011).
Article CAS Google Scholar
Bozier, J. et al. The evolving landscape of e-cigarettes: a systematic review of recent evidence. Chest 157 , 1362–1390 (2020).
CDC. About electronic cigarettes (E-cigarettes). https://www.cdc.gov/tobacco/basic_information/ecigarettes/about-e-cigarettes.html (2020)
Blount, B. C. et al. Vitamin E acetate in bronchoalveolar-lavage fluid associated with EVALI. N. Engl. J. Med. 382 , 697–705 (2020).
Palamidas, A. et al. Acute effect of an e-cigarette with and without nicotine on lung function. Tob. Induc. Dis. 12 , A34–A34 (2014).
PubMed Central Google Scholar
Wang, J. B. et al. Cigarette and e-cigarette dual use and risk of cardiopulmonary symptoms in the Health eHeart Study. PLoS ONE 13 , e0198681 (2018).
Article Google Scholar
Chaumont, M. et al. Fourth generation e-cigarette vaping induces transient lung inflammation and gas exchange disturbances: results from two randomized clinical trials. Am. J. Physiol. Lung Cell Mol. Physiol. 316 , L705–l19 (2019).
Schweitzer, R. J., Wills, T. A., Tam, E., Pagano, I. & Choi, K. E-cigarette use and asthma in a multiethnic sample of adolescents. Prev. Med. 105 , 226–231 (2017).
McConnell, R. et al. Electronic cigarette use and respiratory symptoms in adolescents. Am. J. Respir. Crit. Care Med. 195 , 1043–1049 (2017).
Booth, A. et al. The nuts and bolts of PROSPERO: an international prospective register of systematic reviews. Syst. Rev. 1 , 2 (2012).
Moher, D., Liberati, A., Tetzlaff, J. & Altman, D. G. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 339 , b2535 (2009).
Sterne, J. A. et al. ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355 , i4919 (2016).
Higgins, J. P. T. et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343 , d5928 (2011).
Palamidas, A. et al. Acute effect of an e-cigarette with and without nicotine on lung function. Eur. Respir. J. 42 , P1054 (2013).
Google Scholar
Palamidas, A. et al. Acute effects of short term use of ecigarettes on airways physiology and respiratory symptoms in smokers with and without airway obstructive diseases and in healthy non smokers. Tob. Prev. Cessat. 3 , 5 (2017).
Coppeta, L., Magrini, A., Pietroiusti, A., Perrone, S. & Grana, M. Effects of smoking electronic cigarettes on pulmonary function and environmental parameters. Open Public Health J. 11 , 360–368 (2018).
Staudt, M. R., Salit, J., Kaner, R. J., Hollmann, C. & Crystal, R. G. Altered lung biology of healthy never smokers following acute inhalation of E-cigarettes. Respir. Res. 19 , 78 (2018).
Ferrari, M. et al. Short-term effects of a nicotine-free e-cigarette compared to a traditional cigarette in smokers and non-smokers. BMC Pulm. Med. 15 , 120 (2015).
Boulay, M.-È., Henry, C., Bossé, Y., Boulet, L.-P. & Morissette, M. C. Acute effects of nicotine-free and flavour-free electronic cigarette use on lung functions in healthy and asthmatic individuals. Respir. Res. 18 , 33 (2017).
Puliyakote, A. S. K. et al. Vaping disrupts ventilation-perfusion matching in asymptomatic users. J. Appl. Physiol. 130 , 308–317 (2021).
Polosa, R. et al. Health impact of E-cigarettes: a prospective 3.5-year study of regular daily users who have never smoked. Sci. Rep. 7 , 13825 (2017).
Download references
Acknowledgements
The authors would like to thank Jenna Glidden and Andrea Hebert-Losier for their assistance with study screening, data abstraction, and risk of bias assessment. The authors would also like to thank Francesca Frati, who peer-reviewed the search strategy. This work was funded by the Canadian Institutes for Health Research (#HEV-172891). The funder of the study had no role in study design, data collection, data analysis, data interpretation, writing of the report, or decision to submit for publication. Dr. Filion is supported by a Senior Research Scholar award from the Fonds de recherche du Québec – Santé and a William Dawson Scholar award from McGill University. Dr. Thombs was supported by a Tier 1 Canada Research Chair.
Author information
Authors and affiliations.
Lady Davis Institute for Medical Research, Jewish General Hospital/McGill University, Montreal, QC, Canada
Lucy Honeycutt, Katherine Huerne, Alanna Miller, Erica Wennberg, Kristian B. Filion, Roland Grad, Carolyn Ells, Brett Thombs & Mark J. Eisenberg
Biomedical Ethics Unit, Departments of Medicine and Social Studies of Medicine, and Division of Experimental Medicine, McGill University, Montreal, QC, Canada
Katherine Huerne & Carolyn Ells
Departments of Medicine and of Epidemiology, Biostatistics and Occupational Health, McGill University, Montreal, QC, Canada
Kristian B. Filion, Andrea Benedetti, Brett Thombs & Mark J. Eisenberg
Department of Family Medicine, McGill University, Montreal, QC, Canada
Roland Grad & Carolyn Ells
Division of Respirology, Department of Medicine, Sunnybrook Health Sciences Centre and the University of Toronto, Toronto, ON, Canada
Andrea S. Gershon
Schulich Library of Physical Sciences, Life Sciences, and Engineering, McGill University, Montreal, QC, Canada
Genevieve Gore
Respiratory Epidemiology and Clinical Research Unit, Centre for Outcomes Research and Evaluation, Research Institute of the McGill University Health Centre, Montreal, QC, Canada
Andrea Benedetti
Departments of Psychiatry, Psychology, and Biomedical Ethics Unit, McGill University, Montreal, QC, Canada
Brett Thombs
Division of Cardiology, Jewish General Hospital/McGill University, Montreal, QC, Canada
Mark J. Eisenberg
You can also search for this author in PubMed Google Scholar
Contributions
G.G. performed the search. L.H. and K.H. screened studies, extracted data, and performed a risk of bias assessment of included studies. L.H. drafted the manuscript. All authors contributed to the study design and interpretation of results, revised the manuscript for important intellectual content, and approved the final version of the manuscript. M.J.E. supervised the study and is the guarantor.
Corresponding author
Correspondence to Mark J. Eisenberg .
Ethics declarations
Competing interests.
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary information, reporting summary, rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/ .
Reprints and permissions
About this article
Cite this article.
Honeycutt, L., Huerne, K., Miller, A. et al. A systematic review of the effects of e-cigarette use on lung function. npj Prim. Care Respir. Med. 32 , 45 (2022). https://doi.org/10.1038/s41533-022-00311-w
Download citation
Received : 09 May 2022
Accepted : 06 October 2022
Published : 22 October 2022
DOI : https://doi.org/10.1038/s41533-022-00311-w
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
This article is cited by
Gender differences in e-cigarette knowledge, attitudes, and practice among adults in bahrain: a cross-sectional study.
- Adel Salman AlSayyad
- Bayan Abduljalil Alajaimi
- Azhar Faisal Hasan
Discover Public Health (2024)
Our contribution to systematic review and meta-analysis in primary care respiratory medicine
- Tiago Maricoto
- Ioanna Tsiligianni
npj Primary Care Respiratory Medicine (2023)
Quick links
- Explore articles by subject
- Guide to authors
- Editorial policies
Sign up for the Nature Briefing newsletter — what matters in science, free to your inbox daily.
Latest Cochrane Review finds high certainty evidence that nicotine e-cigarettes are more effective than traditional nicotine-replacement therapy (NRT) in helping people quit smoking
17 November 2022
Research led by the University of Oxford, and funded by Cancer Research UK, has found the strongest evidence yet that e-cigarettes, also known as ‘vapes’, help people to quit smoking better than traditional nicotine replacement therapies, such as patches and chewing gums.
New evidence published today in the Cochrane Library finds high certainty evidence that people are more likely to stop smoking for at least six months using nicotine e-cigarettes, or ‘vapes’, than using nicotine replacement therapies, such as patches and gums. Evidence also suggested that nicotine e-cigarettes led to higher quit rates than e-cigarettes without nicotine, or no stop smoking intervention, but less data contributed to these analyses. The updated Cochrane review includes 78 studies in over 22,000 participants – an addition of 22 studies since the last update in 2021.
Smoking is a significant global health problem. According to the World Health Organisation (WHO), in 2020, 22.3% of the global population used tobacco, despite it killing up to half of its users. Stopping smoking reduces the risk of lung cancer, heart attacks and many other diseases. Though most people who smoke want to quit, many find it difficult to do so permanently. Nicotine patches and gum are safe, effective and widely used methods to help individuals quit.
E-cigarettes heat liquids with nicotine and flavourings, allowing users to ‘vape’ nicotine instead of smoking. Data from the review showed that if six in 100 people quit by using nicotine replacement therapy, eight to twelve would quit by using electronic cigarettes containing nicotine. This means an additional two to six people in 100 could potentially quit smoking with nicotine containing electronic cigarettes.
Dr Jamie Hartmann-Boyce, Associate Professor at the University of Oxford, Editor of the Cochrane Tobacco Addiction Group, and an author of the new publication, said: “Electronic cigarettes have generated a lot of misunderstanding in both the public health community and the popular press since their introduction over a decade ago. These misunderstandings discourage some people from using e-cigarettes as a stop smoking tool. Fortunately, more and more evidence is emerging and provides further clarity. With support from Cancer Research UK, we search for new evidence every month as part of a living systematic review. We identify and combine the strongest evidence from the most reliable scientific studies currently available.
For the first time, this has given us high-certainty evidence that e-cigarettes are even more effective at helping people to quit smoking than traditional nicotine replacement therapies, like patches or gums.”
In studies comparing nicotine e-cigarettes to nicotine replacement treatment, significant side effects were rare. In the short-to-medium term (up to two years), nicotine e-cigarettes most typically caused throat or mouth irritation, headache, cough, and feeling nauseous. However, these effects appeared to diminish over time.
Dr Nicola Lindson, University Research Lecturer at the University of Oxford, Cochrane Tobacco Addiction Group’s Managing Editor, and author of the publication said: “E-cigarettes do not burn tobacco; and as such they do not expose users to the same complex mix of chemicals that cause diseases in people smoking conventional cigarettes. E-cigarettes are not risk free, and shouldn’t be used by people who don’t smoke or aren’t at risk of smoking. However, evidence shows that nicotine e-cigarettes carry only a small fraction of the risk of smoking. In our review, we did not find evidence of substantial harms caused by nicotine containing electronic cigarettes when used to quit smoking. However, due to the small number of studies and lack of data on long-term nicotine-containing electronic cigarette usage – usage over more than two years – questions remain about long-term effects.”
The researchers conclude that more evidence, particularly about the effects of newer e-cigarettes with better nicotine delivery than earlier ones, is needed to assist more people quit smoking. Longer-term data is also needed.
Michelle Mitchell, chief executive at Cancer Research UK, said: “We welcome this report which adds to a growing body of evidence showing that e-cigarettes are an effective smoking cessation tool. We strongly discourage those who have never smoked from using e-cigarettes, especially young people. This is because they are a relatively new product and we don’t yet know the long term health effects.“
“While the long term effects of vaping are still unknown, the harmful effects of smoking are indisputable – smoking causes around 55,000 cancer deaths in the UK every year. Cancer Research UK supports balanced evidence-based regulation on e-cigarettes from UK governments which maximises their potential to help people stop smoking, whilst minimising the risk of uptake among others.”
This work was supported by Cancer Research UK [A ref. A29845]
Notes to Editors:
https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD010216.pub7/full
doi: 10.1002/14651858.CD010216.pub7 Lead authors: Associate Professor at the Nuffield Department of Primary Care Health Sciences, University of Oxford and Editor of the Cochrane Tobacco Addiction Group, Dr Jamie Hartmann-Boyce and Senior Researcher at the Nuffield Department of Primary Care Health Sciences, University of Oxford and Managing Editor of the Cochrane Tobacco Addiction Group, Dr Nicola Lindson.
To speak to a team member about this project please contact Dr. Hartmann-Boyce, [email protected] or Dr. Lindson, [email protected] .
About Cochrane Cochrane is a global independent network of researchers, professionals, patients, carers, and people interested in health. Cochrane produces reviews which study all the best available evidence generated through research and make it easier to inform decisions about health. These are called systematic reviews. Cochrane is a not-for profit organization with collaborators from more than 130 countries working together to produce credible, accessible health information that is free from commercial sponsorship and other conflicts of interest. Our work is recognized as representing an international gold standard for high-quality, trusted information. Find out more at cochrane.org
The University of Oxford Oxford University has been placed number 1 in the Times Higher Education World University Rankings for the seventh year running, and 2 in the QS World Rankings 2022. At the heart of this success is our ground-breaking research and innovation. Oxford is world-famous for research excellence and home to some of the most talented people from across the globe. Our work helps the lives of millions, solving real-world problems through a huge network of partnerships and collaborations. The breadth and interdisciplinary nature of our research sparks imaginative and inventive insights and solutions. Through its research commercialisation arm, Oxford University Innovation, Oxford is the highest university patent filer in the UK and is ranked first in the UK for university spinouts, having created more than 200 new companies since 1988. Over a third of these companies have been created in the past three years. The university is a catalyst for prosperity in Oxfordshire and the United Kingdom, contributing £15.7 billion to the UK economy in 2018/19, and supports more than 28,000 full time jobs.
Oxford University’s Medical Sciences Division : The Medical Sciences Division is an internationally recognised centre of excellence for biomedical and clinical research and teaching and is the largest of the four academic divisions within the University. Over 5000 academics, researchers, NHS clinicians and GPs, and administrative staff, 1500 graduate and 1600 undergraduate students, together contribute to our extensive and exemplary research, teaching, and clinical portfolios. We aim to be the best university biomedical institution in Europe and amongst the best five biomedical institutions in the world and have been ranked number one for the last twelve years in the Times Higher Education World University Rankings for clinical, pre-clinical and health sciences - the only non-North American institution to be top-ranked by THE in any subject discipline.
Within the division, the Nuffield Department of Primary Care Health Sciences has been one of the world’s most important primary care centres for over 20 years; leading world-class research and training to rethink the way healthcare is delivered in general practice and other primary care settings. The department’s main research focus is on the prevention, early diagnosis, and management of common illness, bringing together academics from many diverse backgrounds to work together to produce benefits for the NHS, for populations and for patients. www.phc.ox.ac.uk .
DISCOVER MORE
- Support Oxford's research
- Partner with Oxford on research
- Study at Oxford
- Research jobs at Oxford
You can view all news or browse by category

IMAGES
COMMENTS
A scientific statement from the American Heart Association reviews the current evidence on e-cigarette use and its impact on the heart and lungs. It highlights the need for more studies on the short- and long-term effects of e-cigarettes and their ingredients.
Here, we review the growing body of literature investigating the impacts of vaping on respiratory health. We review the clinical manifestations of vaping related lung injury, including the EVALI outbreak, as well as the effects of chronic vaping on respiratory health and covid-19 outcomes.
New research from the Institute of Psychiatry, Psychology & Neuroscience (IoPPN) at King’s College London has found that the use of vaping products rather than smoking leads to a substantial reduction in exposure to toxicants that promote cancer, lung disease and cardiovascular disease.
Researchers at Massachusetts General Hospital found fibrosis and injury in the small airways of four chronic e-cigarette users, similar to chemical inhalation damage. The study suggests that quitting vaping can partially reverse the condition, but not completely due to residual scarring.
The findings, which appear today in the journal Arteriosclerosis, Thrombosis, and Vascular Biology, add to growing evidence that long-term use of e-cigarettes can harm a person’s health. Researchers have known for years that tobacco smoking can cause damage to blood vessels.
Numerous in vivo and in vitro studies have been performed to better understand the impact of these new inhalable compounds on human health. Results of toxicological analyses suggest that e-cigarettes can be safer than conventional cigarettes, although harmful effects from short-term e-cigarette use have been described.
Two studies show that long-term e-cigarette use can significantly impair the function of the body’s blood vessels, increasing the risk for cardiovascular disease. The studies also suggest that combining e-cigarettes with regular cigarettes may increase health risks and that airway irritation may be the main cause of blood vessel damage.
The report highlights the latest data and evidence on e-cigarette use, also called vaping, and its potential harm to the heart and lungs. It also recommends research priorities to better understand the long-term impact of these products on human health.
Given the increasing use of e-cigarettes and uncertainty surrounding their safety, we conducted a systematic review to determine the effects of e-cigarettes on measures of lung function.
Research led by the University of Oxford, and funded by Cancer Research UK, has found the strongest evidence yet that e-cigarettes, also known as ‘vapes’, help people to quit smoking better than traditional nicotine replacement therapies, such as patches and chewing gums.